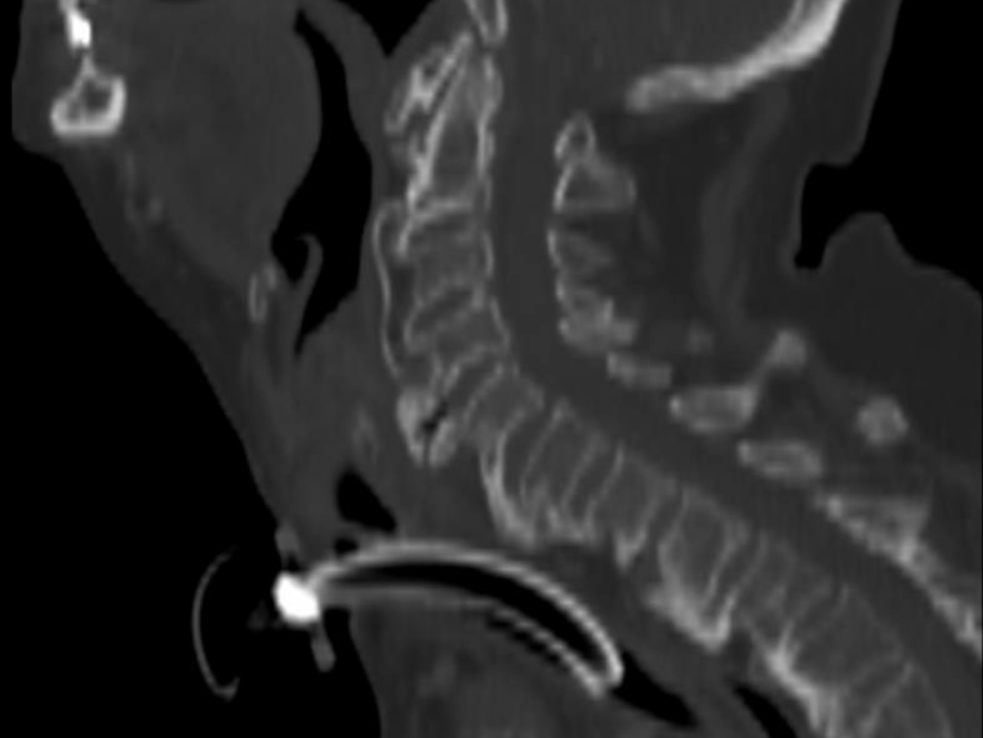
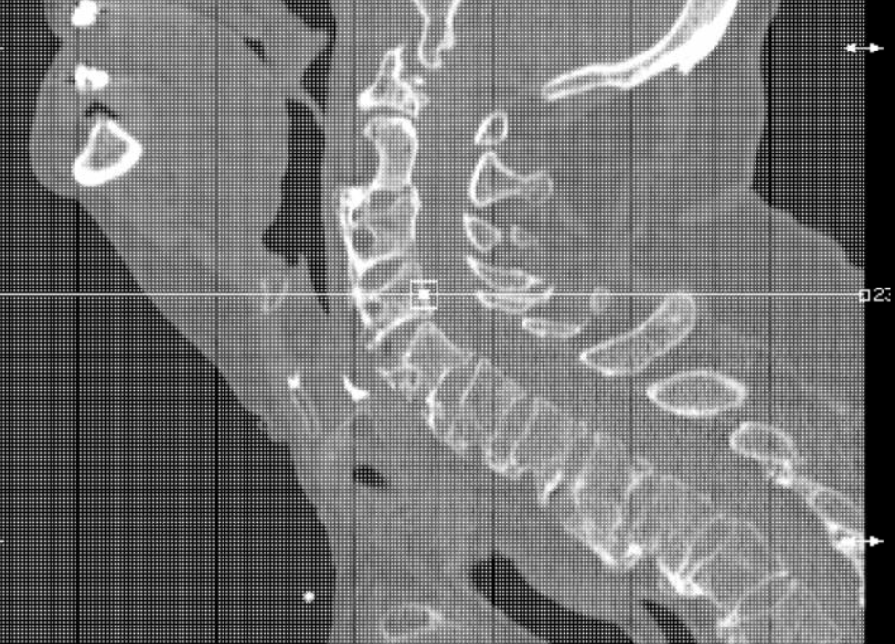
Case Presentation: An 89-year-old woman presented to the emergency department with dyspnea and dysphagia. She gave a one-year history of progressive hoarseness of voice, intermittent dyspnea, and dysphagia. Physical exam was positive for stridor, but negative for any neurological, thyroid, or pulmonary disease. Initial management involved administration of dexamethasone and urgent transnasal flexible fiberoptic laryngoscopy, which showed bilateral vocal fold palsy. An emergency tracheostomy was performed. Neck soft tissue radiography and brain MRI were unremarkable. CT of the soft tissues of the neck with contrast showed diffuse edema of the hypopharynx and bulky anterior cervical osteophytes. Chest CT showed findings of DISH in the thoracic spine, with no evidence of compression of the recurrent laryngeal nerves. A modified barium swallow showed aspiration and she underwent gastric tube placement. Definitive treatment with anterior cervical vertebrectomy and osteophyte removal of C4, C5, and C6 was performed with remarkable improvement. After a period of rehabilitation, both the feeding tube and the tracheostomy were successfully removed.
Discussion: Diffuse idiopathic skeletal hyperostosis (DISH) is common in the elderly, but the majority of cases remain asymptomatic. DISH has a predilection for involving the insertion sites (enthuses) of the ligaments, tendons and joint capsules, causing tortuous paravertebral masses. Thoracic spine is the most commonly affected location, but serious complications are usually related to involvement of the cervical spine. DISH findings are commonly overlooked in the workup of patients with vocal cord palsy with subsequent delay in diagnosis and management.
Conclusions: Giant osteophytes causing direct pressure on the hypopharynx and vocal cords or pressure on the recurrent laryngeal nerves should be kept in mind during evaluation of elderly patients with dysphagia, stridor, and dysphonia.