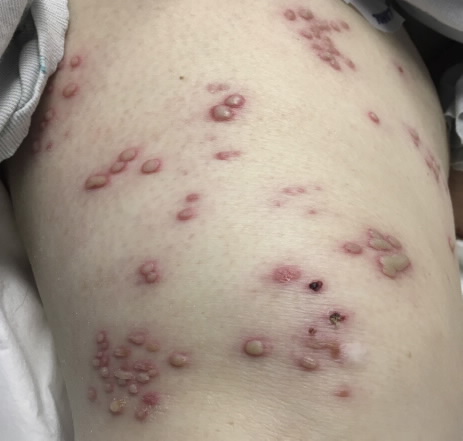
Case Presentation: Herpes simplex virus 2 (HSV-2) infection often presents in a disseminated pattern in immunocompromised hosts. Immunocompetent hosts typically present with genital or oral lesions or have HSV-2 or varicella-zoster virus (VZV) that follows along a dermatomal pattern. Here we present a herpetiform rash, which was culture positive for HSV-2 on biospy, that disseminated across an immunocompetent patient’s lower extremities after a T1-T6 spinal cord injury. She had no previous known history of HSV-2 and was exposed to VZV as a child with chicken pox, but presented with a new herpetiform rash disseminated across lower extremities and abdomen after neurosurgical repair. Our patient was 40 year old caucasian female was transferred from the surgical ICU to a general internal medicine service. The patient had been involved in a motor vehicle accident which involved T1-T6 fracture and had needed chronic tracheostomy management. She had been treated for ventillator associated pneumonia with 2 weeks of antibiotics and had responded well. However, during hospitalization, a new herpetiform rash was noted with vesicles and erythema across bilateral lower extremities and abdomen across multiple dermatomes without any distinguishable pattern except that it was below the level of her previous injury. She was afebrile, not taking any immune-modulating or immunosuppressive agents, and was not systemically ill. HIV antibody screen was negative. She did not note any symptoms secondary to her lower extremity paraplegia. Antiviral therapy was initiated using acyclovir and a skin biopsy with culture, VZV, HSV1&2 fluorescent antibodies, and HSV cultures were obtained. The patient was scheduled for punch biopsy with a referral to dermatopathologist after antibodies for VZV and HSV were negative, however HSV culture grew HSV-2. Patient then responded to acyclovir and vesicles begin to scab over and erythema decreased significantly.
Discussion: This case presents a unique diagnostic challenge of a rash that visually appears consistent with a herpetic form rash that would be consistent with HSV-1 or HSV-2. However, the distribution was not at all consistent with typical HSV-1 presentations and exceedingly atypical for HSV-2. The difficulty in obtaining a diagnosis was compounded by the fact that the system no longer retains inpatient hospital consultation services for Dermatology. While HSV-1 and 2 were of low suspicion given the patient’s immunocompetent status and rash distribution, direct antibody testing and culture were obtained as initial workup. The uniqueness of an immunocompetent patient developing bilateral herpetic rash only and exclusively underneath the level of their spinal injury as the first presentation of HSV-2 without any documented genital lesions has yet to be reported elsewhere. The mechanism of traumatic spinal cord injuries in modulating the immune system’s response in HSV-2 infections is unknown, but this case suggests some interplay.
Conclusions: This case suggests that more than traditional immunosuppression can predispose patients to HSV-1 and HSV-2. This case demonstrates a physical insult as well as the lengthy stay on a ventilator contributed to this patients presentation of a disseminated cutaneous form of HSV-2. It also highlights the importance of how to proceed when a dermatologist consult service is not available. In this case, punch biopsies and shave biopsies were obtained with the help of Infectious Disease specialists.