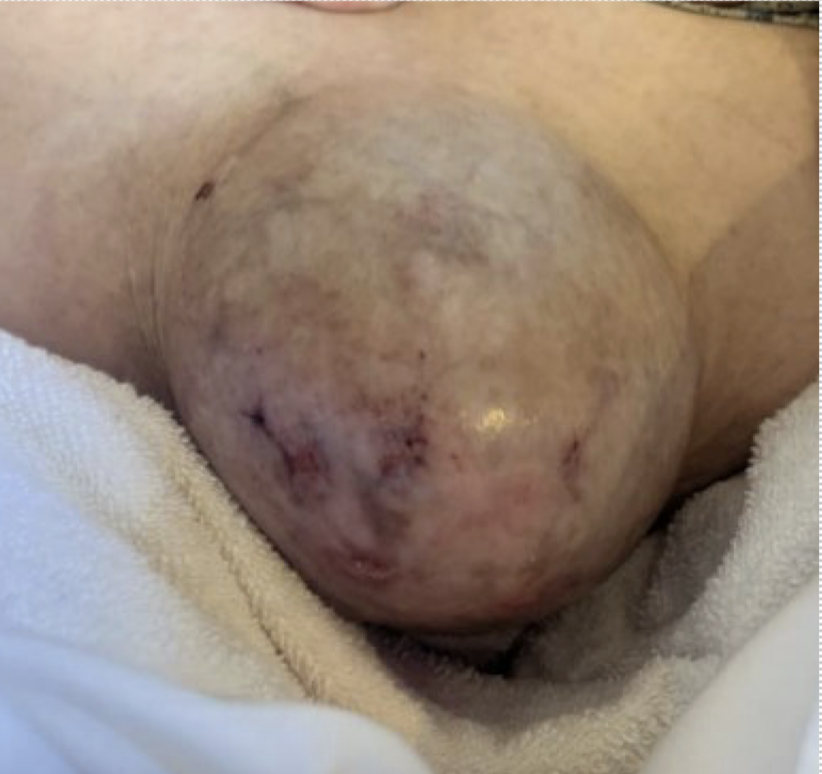
Case Presentation: A 74-year-old female with MASH cirrhosis presented to a local hospital with blood-tinged drainage from her umbilical hernia. Patient endorsed frequent large volume paracenteses (LVP) with 10-15 liters removal every 2 weeks for recurrent ascites refractory to diuretic therapy. The frequency increased to weekly LVP with 6-7 liters per session. CTAP showed liver cirrhosis, small to moderate ascites, large ventral midline abdominal wall hernia containing a dependent ascitic fluid, and diffuse mesenteric edema consistent with chronic third spacing/anasarca. LVP with 5-liter removal was performed before transferring to a tertiary medical center for surgical evaluation of Flood Syndrome. On presentation patient was A&Ox3, stable, no asterixis, abdomen was distended with a large nontender umbilical hernia. Admission labs revealed mild pancytopenia (WBC 2.79 k/µL, Hgb 9.8 g/dL, Plt 84 k/µL), elevated BUN 27 mg/dL, and creatinine 1.10 mg/dL; MELD was 10. Hepatology and Transplant Surgery were consulted. Patient was not a surgical candidate due to uncontrolled ascites and high infection risk. Symptomatic management was pursued with pressure dressings and an abdominal binder. She had periodic hypotension, treated with oral midodrine and volume repletion. Evaluation for adrenal insufficiency and infection were negative; hypotension was attributed to rapidly reaccumulating ascites and a leaking hernia. Underwent EGD with variceal banding. Additional LVPs were performed with >12 liter removal and ultimately, Transjugular Intrahepatic Portosystemic Shunt (TIPS) was performed. Patient tolerated the procedure with resolution of the ascitic drainage from her hernia. She was discharged with eventual follow up for future hernia repair.
Discussion: While first noted in 1901, Frank B Flood reported a case series of cirrhotic patients with massive ascites with spontaneous perforation of the umbilicus in 1961 and coined the term Flood Syndrome. This uncommon complication occurs due to rapid accumulation of large volume ascites which increases the intrabdominal pressure and weakens the abdominal wall over time, causing rupture of the hernia. Although the incidence of umbilical hernia in patients with cirrhosis is reported to be approximately 20%, the incidence of Flood syndrome remains uncommon compared to other complications of cirrhosis (1). Several emergent complications of Flood syndrome can arise, including bowel incarceration, sepsis, and hypotensive shock from fluid shifts (2). Flood syndrome requires prompt recognition by the patient’s primary team, generally the hospital medicine team, to take immediate actions to mitigate the risk of these complications. A CT scan may be used to rule out bowel incarceration. Surgical evaluation is often necessary to determine if the umbilical hernia can be repaired. Also, the best practice in preventing recurrence of Flood syndrome is to prevent ascites (3). Therefore, hepatologists may need to weigh in for evaluation for TIPS candidacy.
Conclusions: Flood syndrome is a rare but potentially fatal complication of ascites in patients with cirrhosis that requires prompt recognition by hospitalists to prevent serious complications, such as bowel incarceration, infection, and shock. We promptly ordered appropriate imaging to rule out incarceration, consulted surgery to determine if the umbilical hernia could be repaired, and consulted hepatology to assess whether the patient was a candidate for TIPS, given refractory ascites.