Background: Burnout among hospital medicine physicians has been reported to be 50-60%, with prevalence likely increasing during the COVID-19 pandemic (1-3). Prior studies suggest burnout may be lower in the Veterans Administration (VA) compared to non-VA healthcare settings (4, 5). However, specific data examining burnout in VA Hospital Medicine (HM) physicians are lacking. To address this gap, we (1) describe burnout prevalence across VA HM sections, and (2) identify correlations between burnout and facility and hospital medicine section characteristics.
Methods: We assessed self-reported burnout across VA HM sections using data from the VA All Employees’ Survey (AES), a national survey distributed in 2023 to all federal government work units. Burnout was defined as an individual reporting at least one of the following three domains: high exhaustion, high depersonalization, and at least weekly frequency of reduced personal achievement. Respondents were aggregated by section to calculate a “section-level prevalence of burnout”. Facility-level characteristics were described using VA administrative data sources, while hospital section characteristics were abstracted from a 2023 national survey of VA HM section chiefs (HM survey). The primary outcome was higher section-level burnout, defined as prevalence higher than the median. Descriptive statistics were used to analyze facility and section characteristics associated with burnout.
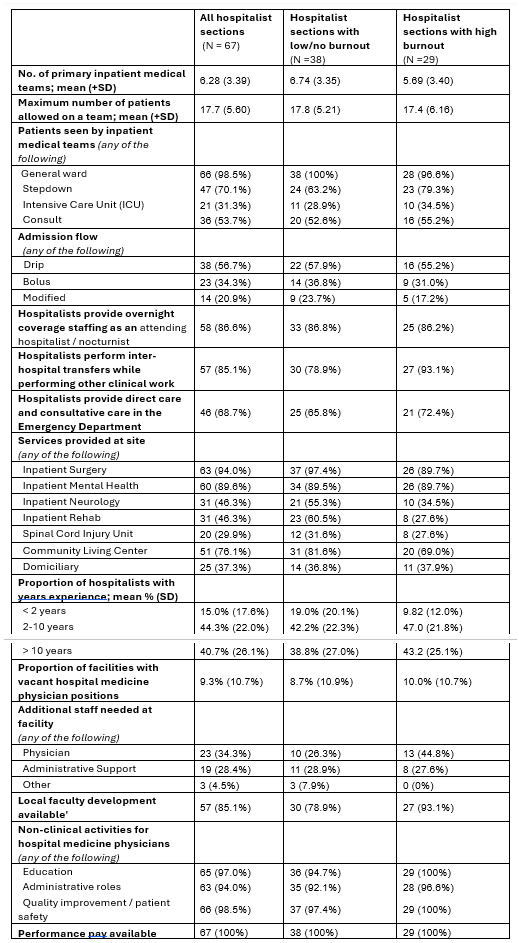
Results: A total of 67 VA Hospital Medicine sections had complete AES and HM survey data. Among these, 29 sections (43.3%) reported burnout higher than the median of 41.6%. Lower section burnout prevalence was associated with the following characteristics: working at the highest-complexity facilities (31.0% of sections with higher burnout vs. 52.6% of sections with lower burnout), academic affiliation (86.2% vs. 94.7%), the presence of physician trainees, including residents/fellows (75.9% vs. 89.5%) and/or medical students (82.8% vs. 92.1%), and having access to a broad array of clinical specialty services, such as neurology (34.5% vs. 55.3%). Conversely, sections with higher burnout often had additional simultaneous clinical responsibilities outside general ward care, such as caring for stepdown (79.3% vs. 63.2%) and/or ICU patients (34.5% vs. 28.9%) or performing inter-hospital transfers (93.1% vs. 78.9%). Additionally, higher burnout was more prevalent in facilities with physician staffing shortages (44.8% vs. 26.3%, Tables 1 and 2).
Conclusions: In a national sample of VA Hospital Medicine sections, hospitalists working in higher complexity facilities with greater available clinical and educational resources, including academic affiliations and subspecialty services, reported lower prevalence of burnout. Many of these associated characteristics are non-modifiable, including high facility complexity and academic affiliation. However, VA leaders and health care providers looking to decrease hospitalist burnout may be able to focus on potentially modifiable workload factors, such as reducing when hospitalists perform multiple high-complexity tasks (e.g. caring for ICU patients and performing inter-hospital transfers) while simultaneously caring for general wards patients. Addressing such section-level characteristics and bolstering opportunities for education and access to specialty services could improve the hospital medicine work environment, and subsequently improve burnout among hospitalists.