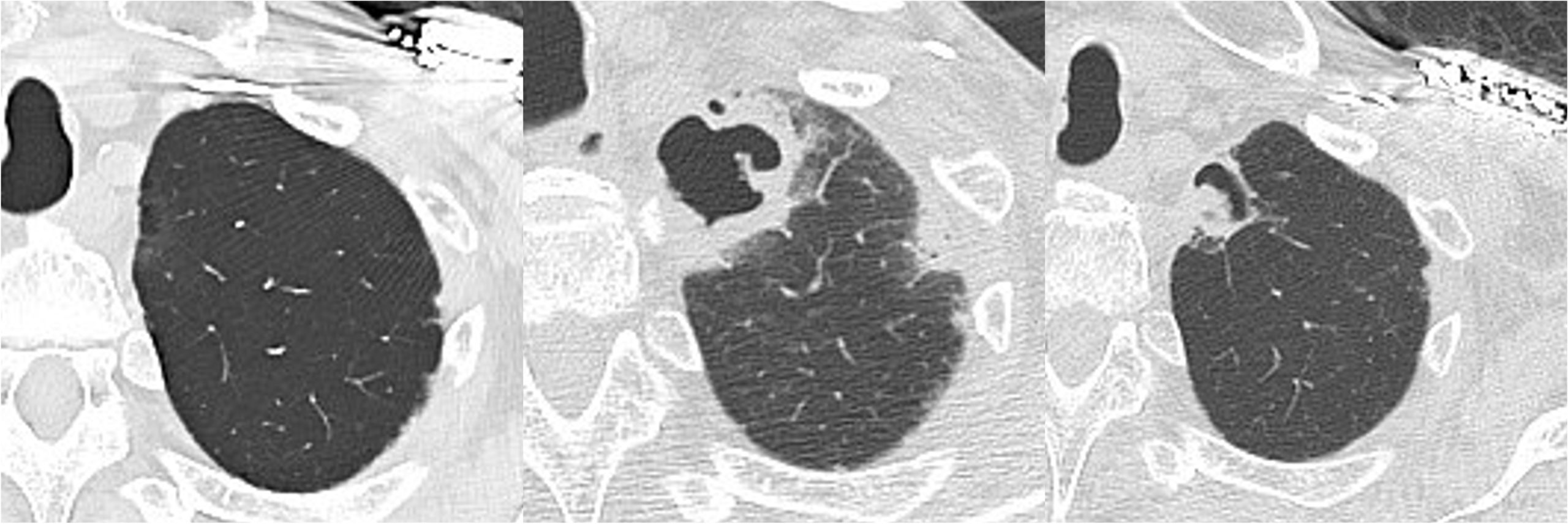
Case Presentation: A 77-year-old man presented with altered consciousness. His medical history included type 2 diabetes mellitus, hypertension, and complete atrioventricular block managed with a pacemaker. Three months earlier, corticosteroid therapy was initiated for acute lung injury of unknown etiology, with symptom improvement followed by dose tapering. He had no history of tuberculosis, mycobacterial infections, or smoking.On the day of presentation, he was found unresponsive by family members. On admission, his vital signs included a body temperature of 34.3°C, heart rate of 78 bpm, respiratory rate of 18 breaths/min, oxygen saturation of 98% on room air, and blood pressure of 117/60 mmHg. His Glasgow Coma Scale score was E4V2M5. Physical examination revealed diminished breath sounds bilaterally in the upper lung fields.Laboratory tests showed severe hypoglycemia (blood glucose 21 mg/dL), leukocytosis (16,000/μL), and elevated C-reactive protein (14.72 mg/dL). Serum Aspergillus galactomannan antigen was positive (index 0.7), and β-D-glucan was mildly elevated (10.2 pg/mL). Chest CT revealed a thin-walled cavity in the right apex and a thick-walled cavitary lesion in the left apex. Acid-fast bacillus smear tests were negative.Hypoglycemia was corrected, and the patient’s consciousness improved. Broad-spectrum antibiotics (ceftriaxone) were initiated, and bronchoscopy with bronchoalveolar lavage and biopsy confirmed the presence of Aspergillus fumigatus, leading to a diagnosis of chronic pulmonary aspergillosis (CPA). Voriconazole therapy was started after discharge. Follow-up CT at three and six months revealed reduced cavitary lesions and development of a fungal ball (aspergilloma) in the left cavity.
Discussion: This case demonstrates the rapid onset of CPA within three months of corticosteroid therapy, emphasizing its potential for accelerated progression in immunosuppressed individuals. While CPA typically evolves over months to years, this case highlights the need for early inclusion of CPA in the differential diagnosis of cavitary lung lesions, especially in patients on corticosteroids.The subacute presentation observed in this case aligns with poorer prognostic outcomes, underscoring the urgency of prompt diagnosis and initiation of antifungal therapy. Early treatment with voriconazole likely contributed to the patient’s favorable clinical and radiological outcomes.Dynamic imaging findings further distinguish this case. Initial CT revealed cavitary lesions without aspergillomas, while follow-up imaging after antifungal therapy showed the emergence of a fungal ball within the cavity. This progression illustrates the importance of longitudinal imaging in monitoring CPA’s course and response to treatment. Such observations also shed light on the interaction between host immune status and disease progression.The role of the hospitalist was critical in this case. Early recognition of CPA and coordination with pulmonologists and infectious disease specialists ensured timely diagnosis and treatment. Multidisciplinary collaboration, coupled with imaging-guided monitoring, allowed for effective management of this complex case.
Conclusions: We have detailed a case of chronic pulmonary aspergillosis that developed subacutely after initiation of corticosteroid therapy.Early diagnosis, timely antifungal therapy, and multidisciplinary collaboration are essential to optimize outcomes in immunosuppressed patients with cavitary lung lesions.