Background: Social drivers of health (SDoH) significantly impact health outcomes, including readmissions and mortality in hospitalized patients post-discharge. The National Academies of Medicine, Engineering, and Sciences (NASEM) created a “5As framework” to categorize activities that health systems can perform to integrate social care into medicine (awareness, adjustment, assistance, alignment, and advocacy), but the frequency of these activities in the inpatient setting is unknown. Adjustment, or adjusting clinical care to accommodate social risk, is particularly relevant to clinical reasoning education: prior studies suggest that providers are more likely to make medical errors for standardized patients who are socially complex. There is a need for a flexible assessment tool to characterize baseline behaviors in addressing SDoH, both to identify educational needs and reliably assess the impact of future educational interventions.
Purpose: We aimed 1) to develop an observation tool to assess how medical teams address SDoH on inpatient rounds using NASEM’s 5As framework through a hybrid classical/modified Delphi method and 2) to establish tool reliability during pilot observations.
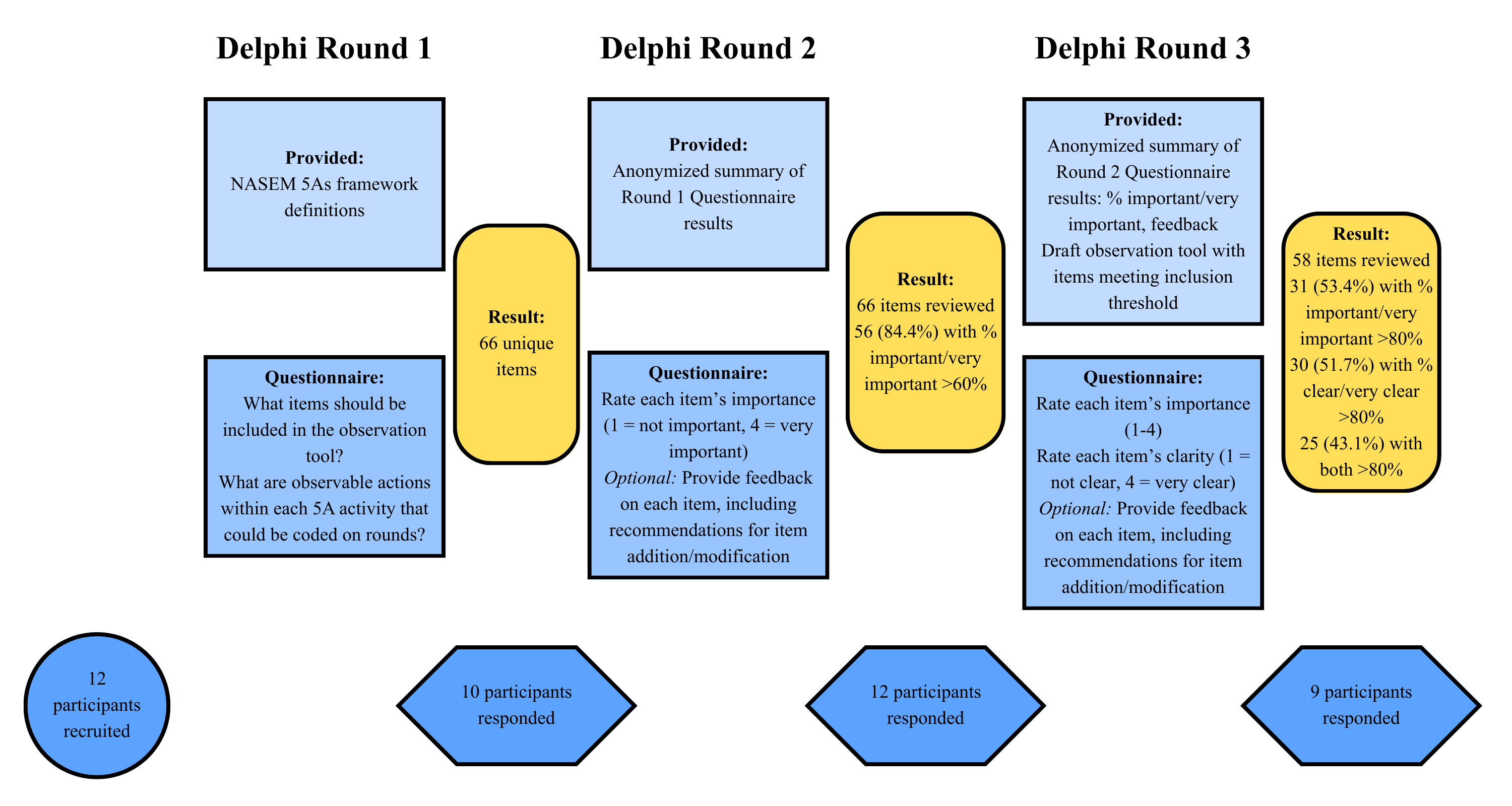
Description: Delphi group participants were recruited by email by snowball sampling. Twelve participants across 9 institutions were successfully recruited. Participation was incentivized with authorship for participation in all three Delphi rounds. The presenting author served as panel convener.Prior to convening the Delphi panel, we defined the completion of the panel as occurring after three Delphi rounds (Figure 1). We set a threshold for item inclusion at the panel completion at 80% consensus on importance (important/very important rating) and clarity (clear/very clear rating; both rated on a 4-point Likert scale). In Delphi round 1, participants were prompted to suggest items for the observation tool in a questionnaire, including items within each of the 5As activities. In rounds 2 & 3, participants were provided with anonymized summaries of the prior round’s questionnaire, and in the current round’s questionnaire, rated items and provided narrative feedback. At the conclusion of the panel, participants received an anonymized summary of round 3 results and the proposed observation tool (Table 1). Eight participants participated in all Delphi rounds (66.7%). Following development of the observation tool, we plan to pilot the tool on inpatient medicine rounds to establish tool reliability. We will train observers on the tool items and observers will use the tool in dyads on medical rounds to assess patient encounters. We will assess tool reliability qualitatively through response process validity, confirming that observers discussed their level of agreement with coding after each observation session. We will quantitatively assess the tool’s inter-rater reliability through calculating Cohen’s kappa.The study was acknowledged as exempt by the IRB.
Conclusions: We successfully developed a novel observation tool through a multi-institution Delphi panel, which will allow us to characterize the behavior of medical teams in addressing SDoH on inpatient rounds. Pilot reliability data will be available by March 2026. This tool will support research assessing the association between addressing SDoH in hospitalized patients and patient outcomes, allowing institutions to identify targets for improvement.
.png)
