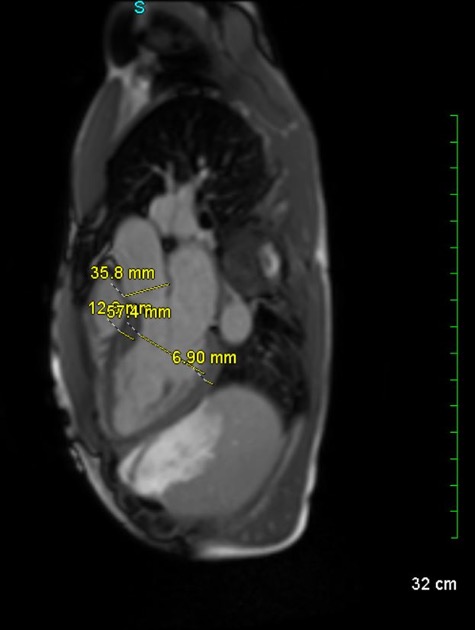
Case Presentation: A 39-year-old man presented with family history of arrhythmogenic right ventricular cardiomyopathy (ARVC). He reported palpitations with exercise. Cascade genetic testing was positive for plakophilin-2 gene mutation. EKG demonstrated sinus bradycardia with possible epsilon wave in V1 and right-axis deviation. Transthoracic echocardiogram was normal. Cardiac MRI (CMR) showed right ventricular free wall thinning and abnormal enhancement suggestive of fatty infiltrates. Genetic testing, EKG, and CMR supported ARVC. Holter revealed intermittent intraventricular conduction abnormality varying from narrow to wide complex with varying PR interval consistent with an intermittent RBBB. Mobile cardiac telemetry uncovered a wide complex rhythm reaching 150 bpm, lacking discernible P-waves, suggesting monomorphic ventricular tachycardia in suspected ARVC or possible supraventricular tachycardia with aberrant conduction. Electrophysiology study revealed atrioventricular node reentrant tachycardia (AVNRT) with an intermittent RBBB. Second opinion disputed previous CMR findings ruling them inconsistent with ARVC. Our patient was diagnosed with AVNRT with aberrant conduction and underwent ablation with no planned cardiac defibrillator for now.
Discussion: ARVC is a rare inherited cardiomyopathy characterized by progressive fibrous or fibro-fatty replacement of myocardium leading to abnormal heart rhythms and increased risk of sudden cardiac death (SCD). Significant disease heterogeneity has been reported. Our patient was gene-positive for ARVC, but phenotypically negative. Both ARVC and AVNRT share similar medication management; however, prognosis differs significantly regarding SCD and mortality. Our patient was gene-positive but phenotypically negative signifying incomplete penetrance ARVC with concurrent AVNRT. A literature review yielded no reports correlating the two disease processes. Accurate diagnosis is critical as select ARVC patients benefit from AICD placement, whereas AVNRT is treated with catheter ablation. Literature review yielded no cases correlating ARVC and AVNRT.
Conclusions: Treatment of both ARVC and AVNRT may involve beta blockers and catheter ablation, but only ARVC has a role for AICD. Current therapeutic approaches to ARVC aim to prevent SCD and reduce symptom burden, but do not prevent disease progression.