Background:
Duty‐hour limitations have increased the number of handoffs of patient responsibility in academic medical centers, raising concerns about discontinuity of care and patient safety (Charap, Annals of Internal Medicine, 2004). Fourth‐year medical students perform the duties of interns, which include transferring patient care responsibilities. We sought to develop and teach a structured, standard method for conducting patient handoffs in an attempt to improve the transfer of information by medical students during their subinternship rotations.
Methods:
We developed a handoff selective that was offered as part of the Integrated Clinician's Course, a 2‐week course created to prepare medical students for their fourth year. Each class session was 2 hours in length. There were between 6 and 8 students per class. The first hour was spent in a didactic session discussing the evidence for the increasing importance of handoffs as well as communication theory. The second hour was spent practicing handoffs from case scenarios we developed. Students would first prepare a written handoff and then engage in role play, transferring care of their patient to another student. We developed a 2‐part survey. The first part was designed to determine the medical students' perceived skills, attitudes, and knowledge about handoffs. The second part was designed to obtain feedback on the usefulness of various aspects of the class. We administered surveys to students taking the selective both before and after the class. The first part of the survey was also administered once to students not taking the selective.
Results:
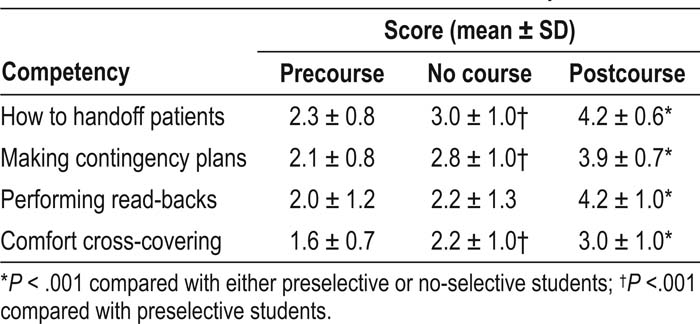
Ninety‐two percent of students believed that the handoff selective was “useful” or “extremely useful,” and 100% of the students believed that the role‐playing activity was “useful” or “extremely useful.” Although 86% of students believed that the didactic was “useful” or “extremely useful,” this was a significantly lower rating than for the role‐playing activity (P < .001). The major theme generated in the open ended comment section of the survey was that “this should be a required course and not a selective.” The effects of the program on the students' self‐perceived skills and knowledge about handoffs are summarized in Table 1 (5‐point Likert scale with 5 representing “strongly agree”).
Conclusions:
Although medical students entering their fourth‐year subinternship believed that patient care handoffs were important, they did not feel confident about their ability to transfer patient care safely and efficiently. A 2‐hour handoff selective increased their knowledge and skills about handoffs as well as their confidence in performing handoffs. This difference held true when they were compared to students who did not choose the selective. Compared with role playing with feedback, medical students found didactic sessions about handoffs to be relatively ineffective.
Author Disclosure:
E. Chu, none; M. Reid, none; T. Schulz, none; M. Burdn, none; D. Dingwell, none; R. Albert, none.