Background: Medical Emergency Teams (METs) are utilized in an inpatient setting to identify patients who exhibit signs of clinical deterioration. Patients, family, or staff activate the team by calling a Code MET when there is a change in clinical status. Patients with End-Stage Renal Disease (ESRD) fare worse than age-, gender-, and race-matched populations. We compared the utilization of Code MET and outcomes between patients with and without ESRD.
Methods: All patients over the age of 18 admitted to Emory University Hospital Midtown and had a Code MET called from January 1, 2017-July 17, 2018 were retrospectively reviewed. Code MET data was manually collected at the time of every Code MET. ESRD diagnosis and demographics were matched with each Code MET using the Emory Data Warehouse by matching MRNs.
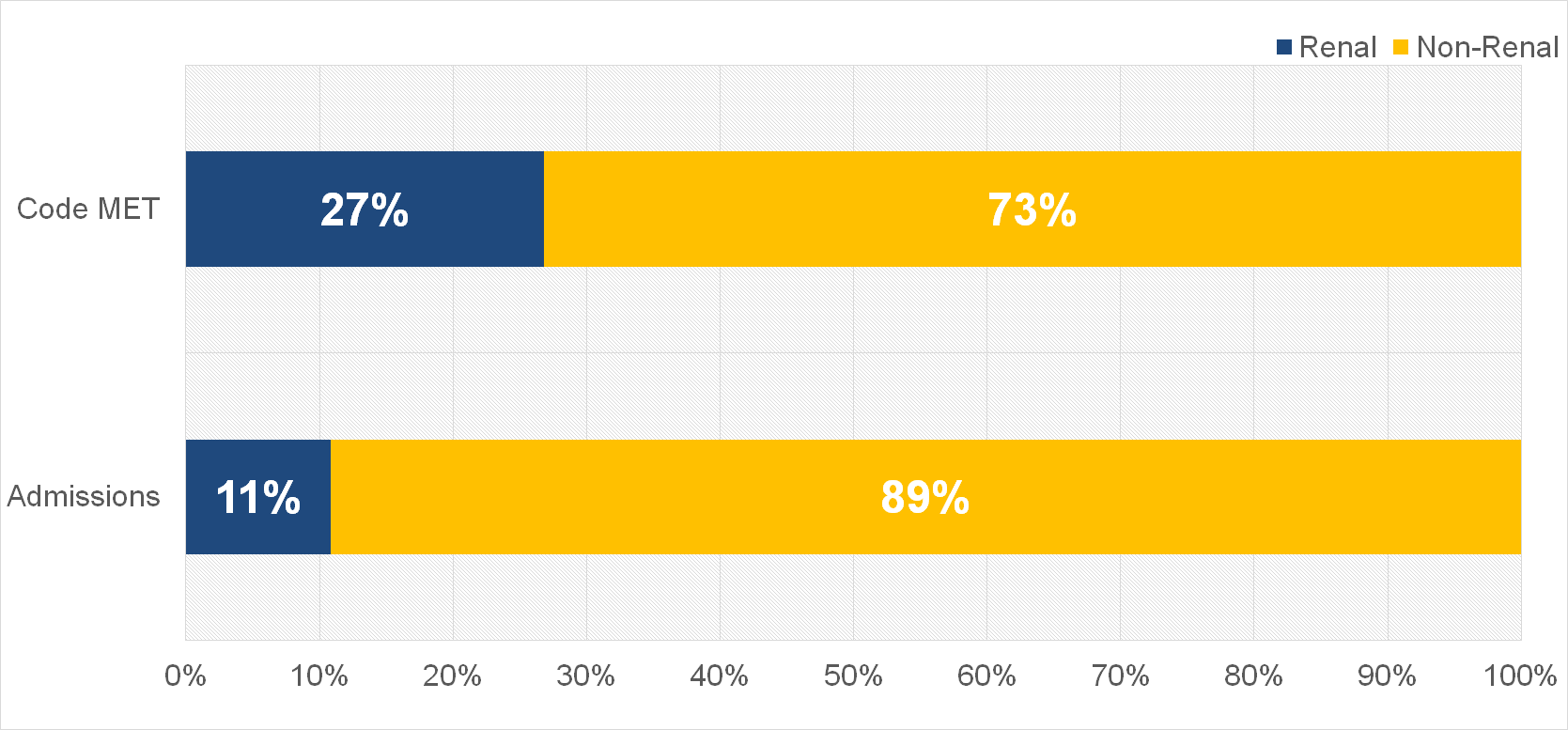
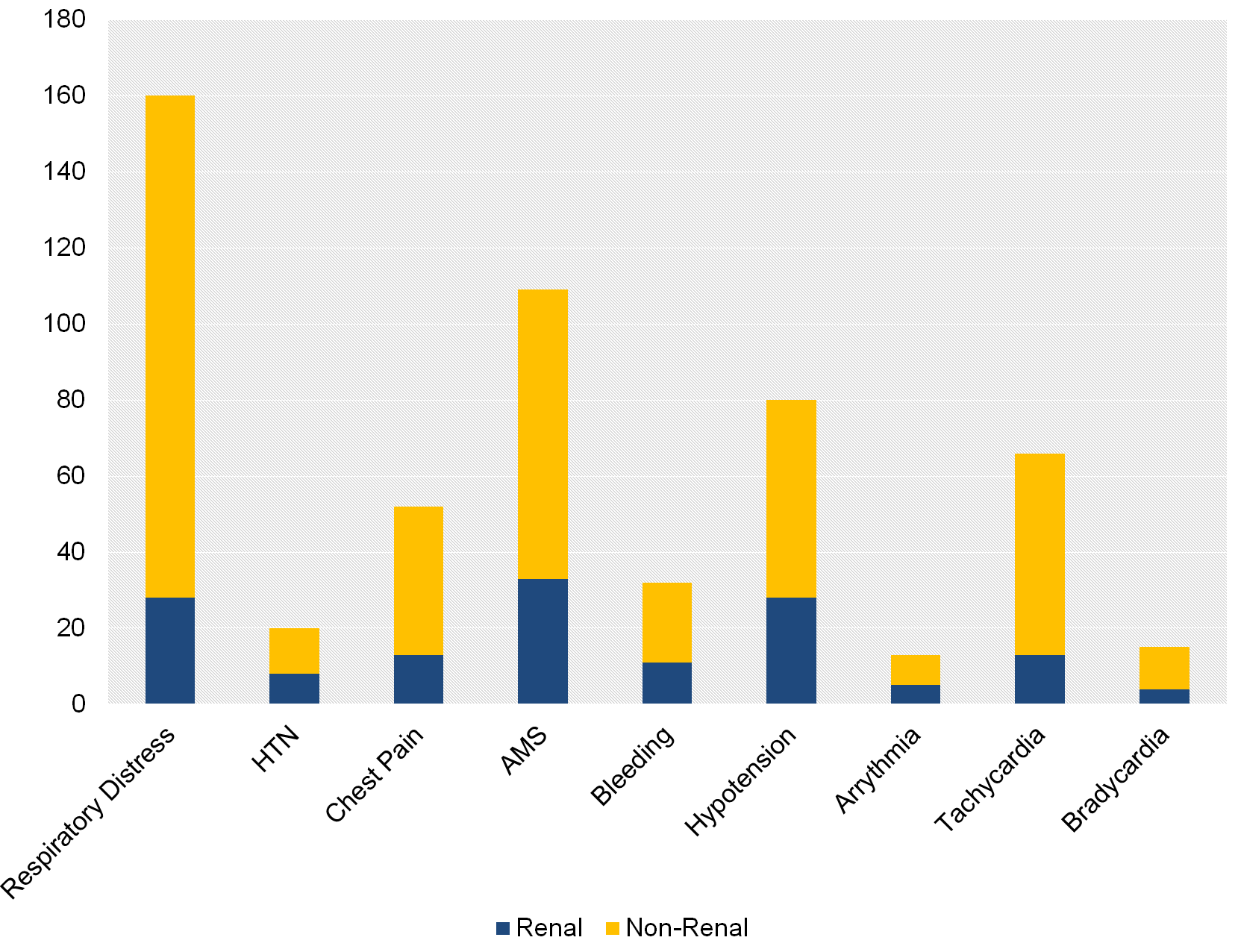
Results: 16,761 admissions to the hospital occurred during the reviewed time period. 1,819 (10.8%) of those patients had ESRD. Code METs occurred more frequently in encounters with ESRD patients with 131 (7.2%) encounters compared to 408 (2.4%) of non-ESRD encounters (p < 0.01). There was no difference in causes of Code MET including Hypertension, Respiratory Distress, Hypoxia, Bleeding or Altered Mental Status. There was a trend towards significance with Hypotension which made up 18.3% of Code METs in ESRD patients compared to 11.5% in non-ESRD patients (p = 0.06). The most common causes for Code MET were Respiratory Distress (26.1%), AMS (17.8%) and Hypotension (13%). Outcomes were similar in terms of maintaining same level of care (remaining on the floor/ward), escalating the level of care (transfer to the ICU), and death. There was no difference in duration of Code MET.
Conclusions: The ESRD population is a population that is at higher risk of having an acute event that requires aggressive, emergent care while in the hospital with increased utilization of the Code MET. More information is needed to determine if any unique interventions can be made for the ESRD population to detect clinical deterioration.