Background: Real-Time Prescription Benefit (RTPB) tools remain underutilized by hospitalists, partly due to concerns surrounding the tools’ availability and accuracy of the co-payment estimates provided. The RTPB tool’s functionality is contingent on the patient’s pharmacy benefit manager (PBM) identification and selection in the electronic health record (EHR). This study aims to investigate the availability of RTPB tools and the accuracy of its estimates for medications prescribed at the time of hospital discharge.
Methods: Retrospective data collection on a focus cohort of 3542 patients discharged from the general medicine service of an academic medical center in Massachusetts was conducted over a 5-month period. Primary EHR data collection included: patient’s insurance payer, insurance plan, PBM and co-payment estimate availability for medications prescribed at discharge. Deceased patients and patients with restricted chart access were excluded to preserve privacy. Data were analyzed to determine the proportion of patients with PBMs identified and selected and the proportion of patients with prescription co-payment estimates or actionable RTPB messages available. For a sub-group of patients whose prescriptions were filled at the hospital’s outpatient pharmacy, the co-payment estimate provided by the tool was compared to the actual price paid to determine the accuracy of the tool’s estimates.
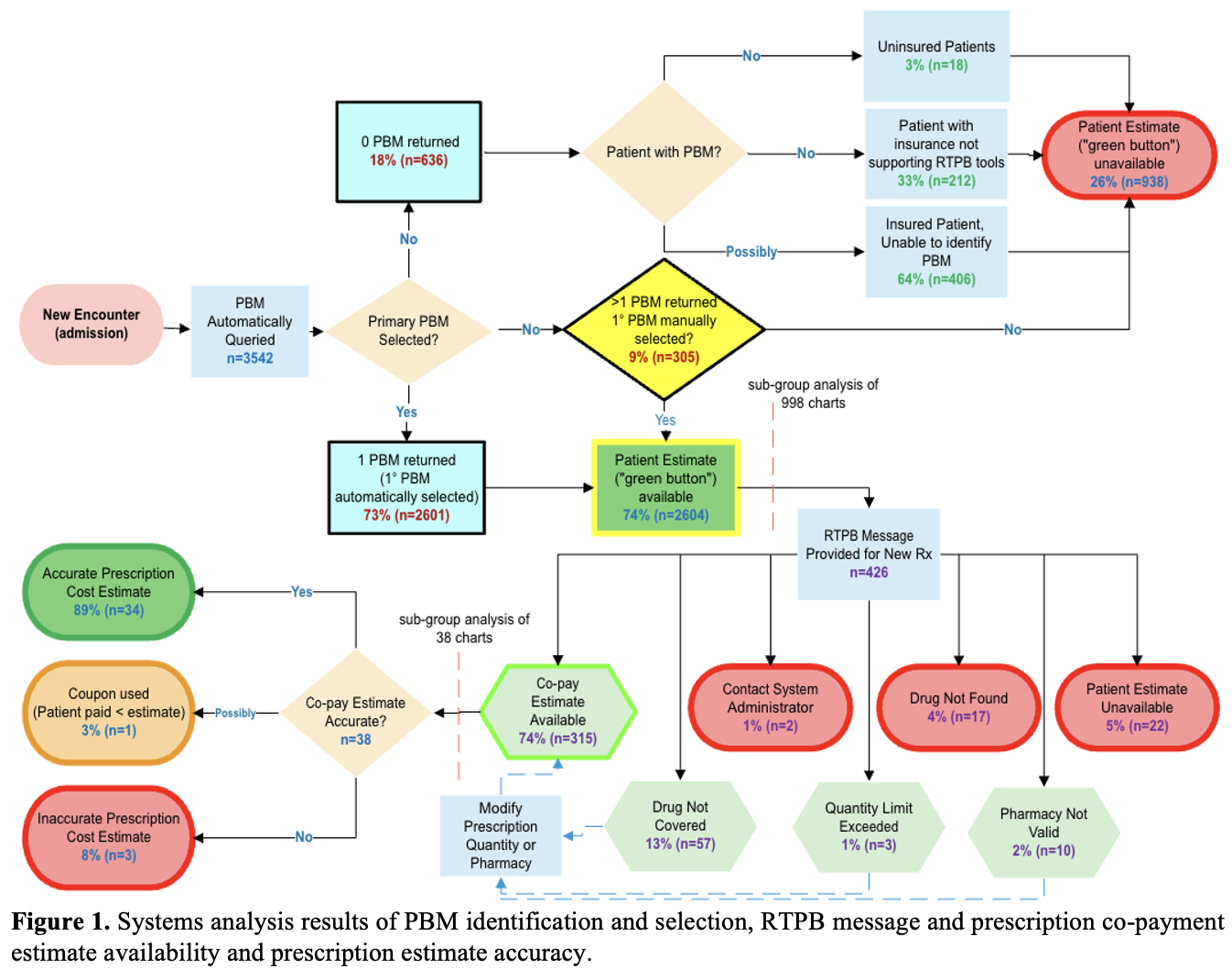
Results: 3542 charts were analyzed, with PBM data and prescription co-payment estimate availability summarized in Figure 1. The RTPB tool was unavailable for 26% (n=938) of patients: 18% (n=636) had no PBM identified and 8% (n=302) had more than 1 PBM with no primary PBM manually selected. 33% of cases with no PBM identified (n=212) were due to Massachusetts Medicaid (MassHealth) not participating in electronic transmission of copayment data. The RTPB tool was available for 74% (n=2604) of patients. Sub-group analysis of 998 of these charts revealed 426 cases with a new prescription at discharge, for which 74% (n=315) a co-payment estimate was returned and an additional 15% of cases (n=70) an actionable RTPB message was returned (e.g., quantity limit exceeded). Preliminary sub-group analysis of 38 charts where prescriptions were filled at the hospital’s outpatient pharmacy showed an 89% (n=34) accuracy of prescription co-payment estimates compared to the actual price paid within a $3 margin. The co-payment estimate was inaccurate 8% of the time (n= 3), predominantly overestimating the co-payment price (n=2).
Conclusions: The RTPB tool is accessible 74% of the time and returns a co-payment estimate or actionable RTPB message 89% of the time, for an overall availability of 66%. The accuracy of the RTPB tool’s co-payment estimate is 89%. Expanding health policy mandates for all prescription plans to support RTPB tools, along with system improvements and provider education, may increase RTPB tools’ availability and use to promote prescription price transparency, affordable medication selection, and medication adherence after hospitalization.