Background: The opioid crisis remains a threat to public health nationwide. In NYC, there were 3,046 drug overdose deaths in 2023, a decrease of only 1% from 2022, with fentanyl involved in 80% of these fatalities. In 2021, the emergency department at our institution began distributing take-home naloxone kits to at-risk individuals on discharge through the Opiate Overdose Prevention Program (OOPP), sponsored by the New York City Department of Health (DOH). There remained a gap, however, in addressing the needs of patients at risk of overdose in the inpatient setting due to a lack of an established protocol and a process for patient identification and kit dispensing.
Methods: Our goal was to achieve a 20% naloxone kit dispensing rate among at-risk patients discharged from the medicine service between October 2023 and March 2024. Naloxone dispensing criteria were established based on guidance from the NYC DOH and the Centers for Disease Control and Prevention, and disseminated to our internal medicine residents, advanced practice practitioners, and attending physicians. Clinicians became certified dispensers of naloxone after completing a 30-minute training session led by our OOPP Director. A kit dispensing algorithm was developed (Figure 1) and a SmartPhrase was created within the EMR for standardized documentation of naloxone dispensing by providers. Several PDSA cycles were implemented from October 2023 to March 2024, including: 1) manual chart audits and secure chat reminders sent to primary teams, 2) nursing education on naloxone dispensing, 3) provider education paired with a raffle incentive, and 4) secure chat reminders sent only for eligible patients who were within 24 hours of discharge.
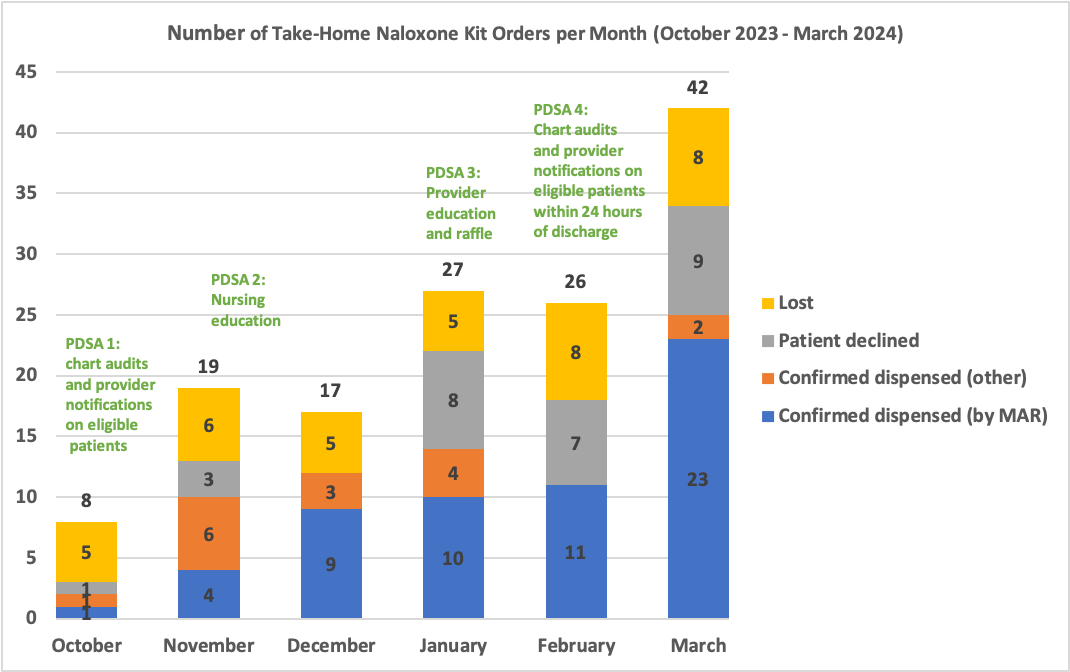
Results: Baseline data was obtained using ICD-10 codes and prescription reports from January through March 2023, and indicated an average of 71 at-risk patients discharged from the medicine service per month. A patient database with take-home naloxone orders and the order administration record were generated biweekly. Manual chart reviews of unadministered orders were conducted to determine any documentation of kit dispensing outside of the medication administration record (MAR). A separate report was generated using the provider dispensing SmartPhrase to determine the number of patients who declined a kit. Data collected from October 2023 to March 2024 showed a marked increase in the number of take-home naloxone kit orders placed, rising from 8 in October 2023 to 42 in March 2024 (Figure 2). Monthly naloxone orders were analyzed and categorized into four groups: 1) orders confirmed as dispensed via a checkmark in the MAR, 2) orders confirmed as dispensed via documentation in the chart (other than the MAR), 3) orders that were declined by patients, and 4) orders that could not be confirmed as dispensed or declined after chart review, thus labeled as “lost”.
Conclusions: By March 2024, the number of naloxone kit orders placed reached 59% of the expected monthly target, exceeding our goal of 20%. While this outcome is encouraging, our primary challenge moving forward will be sustainability. The most effective strategy so far has been manual chart audits and secure chat reminders for eligible patients within 24 hours of discharge. However, this intervention is labor-intensive and not sustainable in the long term. Next steps include collaborating with a multidisciplinary team across our health system to implement a best practice advisory alert within the EMR, which we believe is essential to the continued success of this initiative.