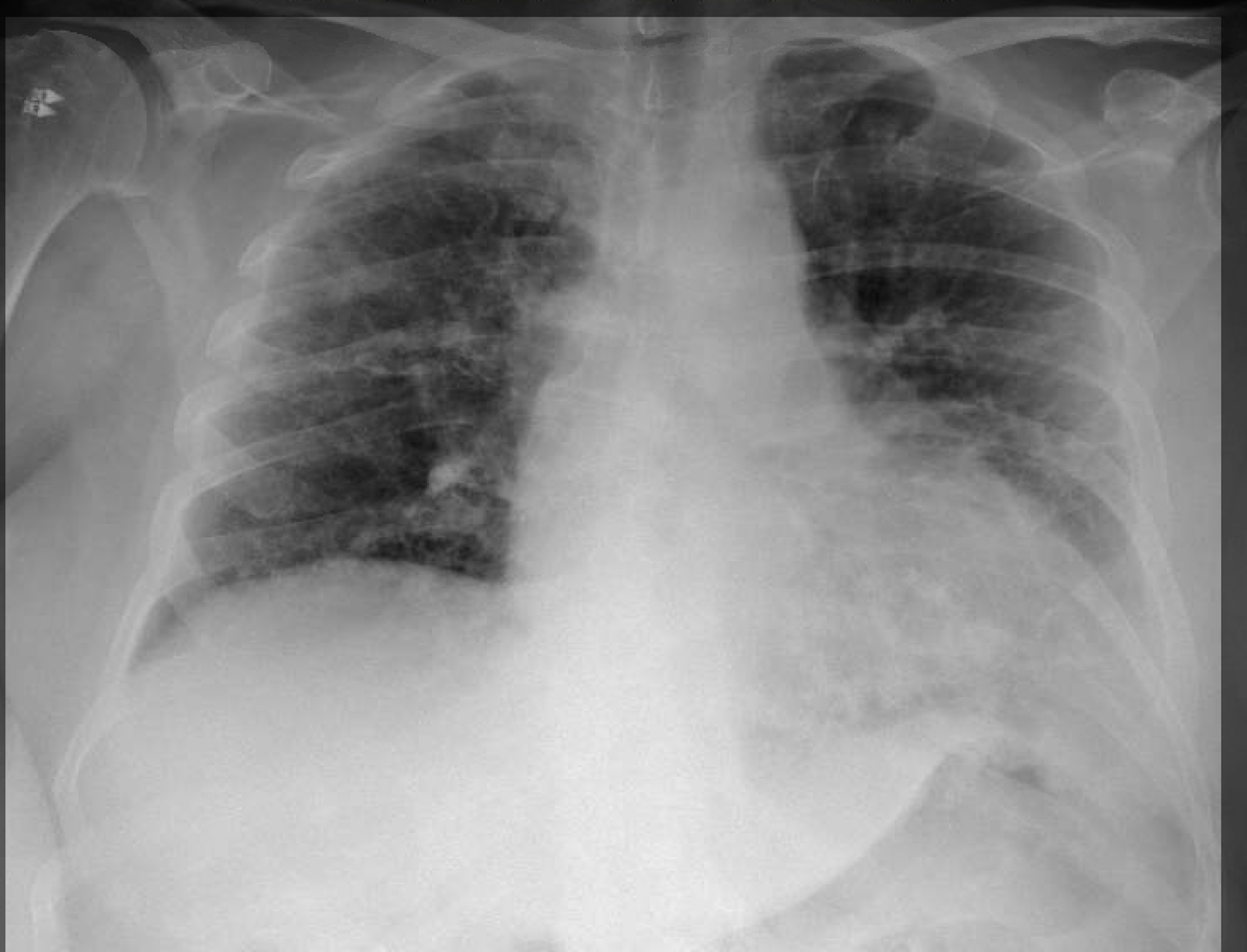
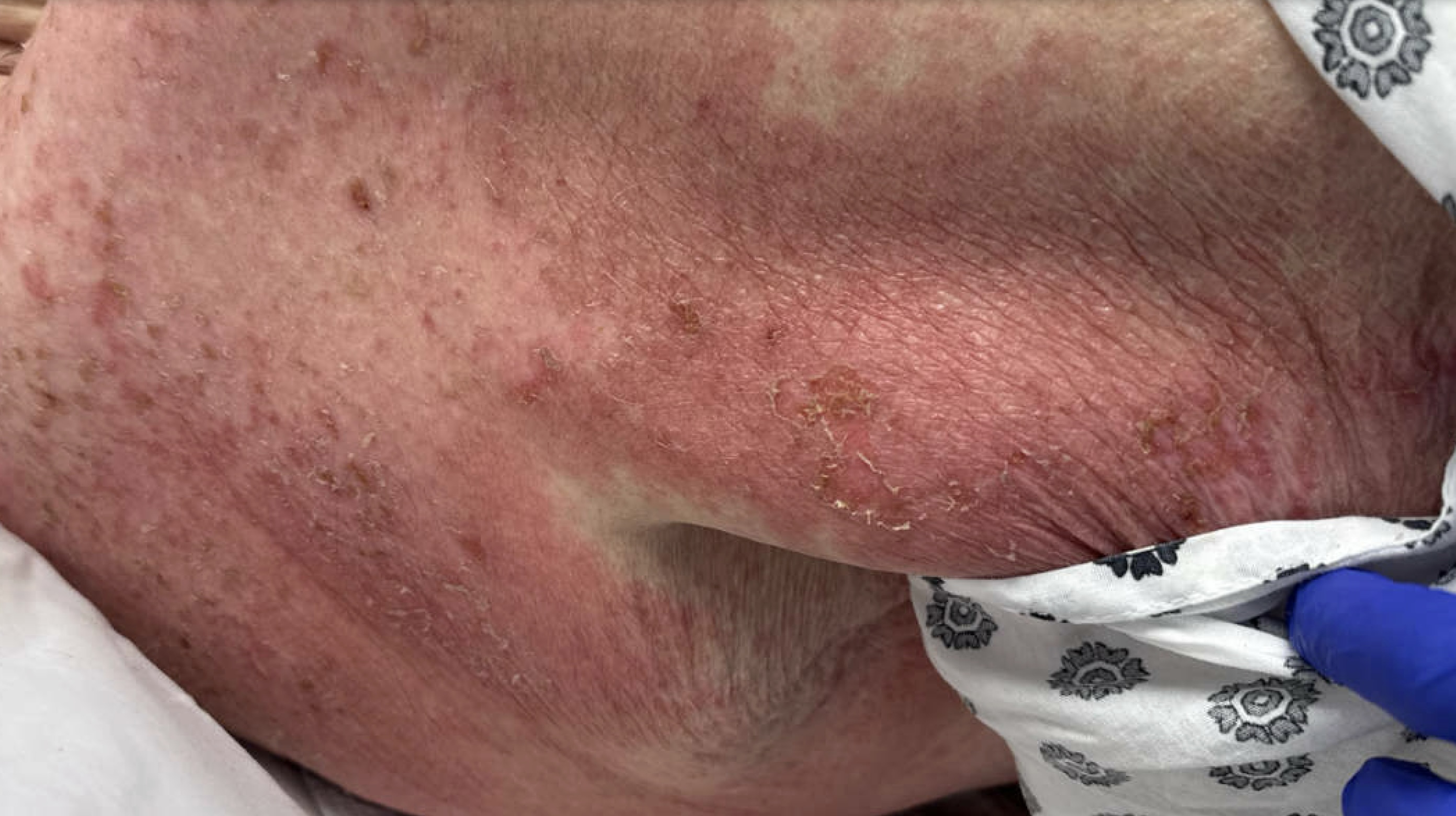
Case Presentation: A 71-year-old female with a past medical history of atrial fibrillation treated with amiodarone and apixaban presented due to a three-week history of diffuse, erythematous, macular rash associated with petechiae and minimal desquamation, without mucosal involvement. She described the rash as pruritic and painful. Previously attempted outpatient therapies included topical and low dose oral steroids without significant relief. Initial workup with a chest x-ray showed findings concerning for pneumonitis, therefore, amiodarone was stopped on admission. She was started on vancomycin, which was shortly discontinued due to low concern for infectious etiology. Her hospital course was complicated by episodic pleuritic chest pain, elevated liver function tests, and pancytopenia. Further investigation into possible autoimmune causes of her rash revealed a positive antinuclear antibody and an elevated anti-histone antibody level, while anti-double stranded DNA antibody was negative. She underwent a punch biopsy which showed lichenoid interface dermatitis. Multiple consultants were involved in the case including the burn team due to initial concerns for Stevens-Johnson syndrome, hematology due to pancytopenia, infectious disease, allergy and immunology, and finally rheumatology. The consulting rheumatologist agreed that the clinical picture was highly suspicious for drug-induced lupus due to serologic findings and associated pleurisy and pancytopenia. The causative drug was thought to be amiodarone, which had been initiated six months prior to symptom onset. She started a course of high dose oral prednisone with significant improvement.
Discussion: Medications such as procainamide and hydralazine are well-established causes of drug induced lupus erythematosus (DILE), although few cases have been reported of DILE related to amiodarone use. DILE should be considered in patients with an unexplained rash and a history of amiodarone use, especially with the presence of other findings frequently associated with this condition, such as pleurisy, pancytopenia, and positive anti-nuclear and anti-histone antibodies. This condition may occur weeks to months after starting the offending agent, making diagnosis difficult. DILE resolves with discontinuation of the causative medication; however, it may take weeks to months for complete resolution. Serious manifestations can be treated with oral steroids.
Conclusions: This case raises awareness of the potential for amiodarone to cause DILE. Drug-induced lupus can be a difficult diagnosis due to the extensive list of medications that can trigger this phenomenon. This complexity is heightened, leading to further diagnostic uncertainty, when a less commonly implicated medication causes DILE. While the prognosis is favorable, early recognition is important to avoid prolonged hospitalization and unnecessary interventions.