Background: Undocumented immigrants comprise an estimated 3% of the US population. In many regions, this population is ineligible for public insurance programs like Medicaid and Medicare and typically receive coverage only for emergency services. In addition to lacking health insurance, many face barriers such as poverty, food insecurity, homelessness, unemployment, illiteracy, stigmatization, and fear of deportation. These challenges highlight the need to understand their healthcare utilization and outcomes.
Methods: We reviewed electronic medical records of self-pay patients seen at our institution’s Primary Care Center (2020-2023). Patients were divided into two cohorts: 1) Undocumented (no health insurance and SSN, labeled as “undocumented” in social work notes, n=162), and 2) U.S. citizens (SSN on file, no health insurance, n=124). Demographics, social determinants of health (SDOH), medical comorbidities, healthcare utilization (ED visits, charges, readmissions, length of stay), and primary diagnosis codes were analyzed.
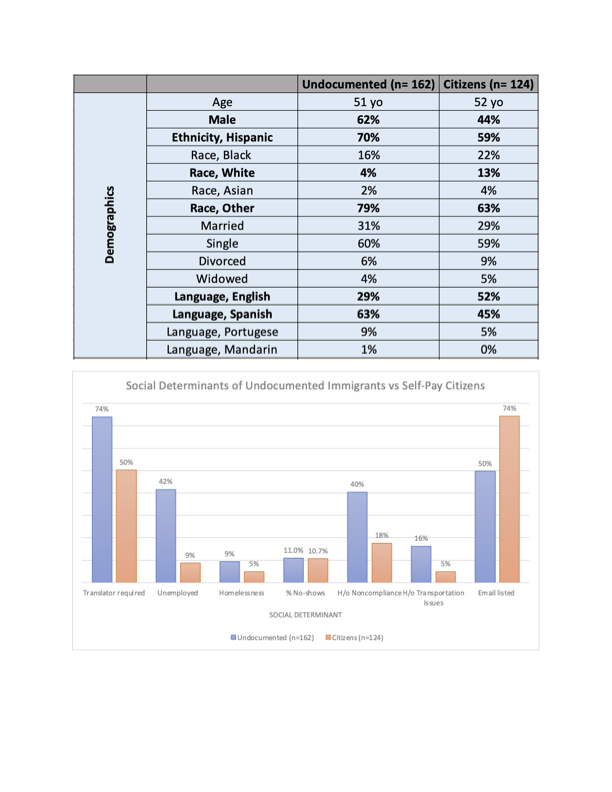
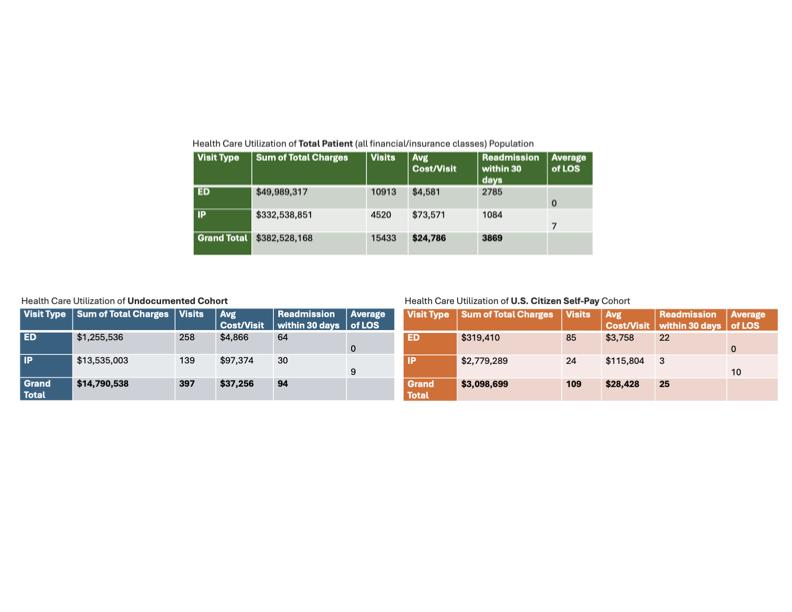
Results: Compared to U.S. citizens, undocumented patients were more likely to require a translator (50% vs 74%), be unemployed (9% vs 42%), have medication noncompliance (18% vs 40%), and experience transportation issues (5% vs 16%). Higher rates of diabetes (22% vs 30%), chronic kidney disease (3% vs 10%), depression (17% vs 28%), alcohol use disorder (10% vs 17%), and suicidal ideation (2% vs 8%) were observed in the undocumented group. The first abnormal A1C recorded was also higher in undocumented patients (8.1 vs 8.9). Regarding healthcare utilization, undocumented patients had more ED visits (258 vs 85), hospitalizations (139 vs 24), higher mean hospital charges ($37,256 vs $28,428), and higher re-admission rates (94 vs 25) compared to the self-pay U.S. citizen cohort. Undocumented patients also demonstrated higher proportions of ED diagnoses for mental/behavioral disorders (12.5-fold), infections (10-fold), gastrointestinal conditions (6.5-fold), and endocrine/metabolic disorders (6-fold) compared to U.S. self-pay citizens. Among the undocumented cohort, mental and behavioral ED visits were predominately represented by alcohol-related disorders (19 of 25; 76%), infection-related visits by COVID-19 (6 of 10; 60%), and endocrine visits by diabetes with complication (5 of 6; 83%).
Conclusions: Compared to uninsured self-pay U.S. citizens, undocumented patients had more SDOH barriers and a higher prevalence of medical and psychiatric conditions. These observed differences suggest worse overall health status, which aligns with higher rates of ED visits, inpatient admissions, and readmissions. The higher healthcare utilization translates to higher health care costs. Our findings highlight the need for improved care coordination and targeted outpatient interventions. Future work should involve larger interventional studies to address these observed differences between uninsured U.S. citizens and undocumented immigrants.