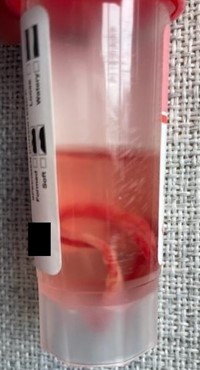
Case Presentation: A 63-year-old man with a history of atopy recently started on dupilumab presented to a hospital in Central Appalachia with 1-week of flu-like symptoms, rigors, and right upper abdomen pain. He was hypoxic with SpO2 75% on room air, febrile to 103.3°F, tachycardic to 105 bpm. He was placed on 2 L nasal cannula. Exam revealed right upper abdominal tenderness and clear lungs. Initial labs showed normal white blood count, creatinine 1.63 mg/dL, total bilirubin 3.5 mg/dL, aspartate aminotransferase 102 U/L, alanine transaminase 150 U/L, alkaline phosphatase 396 U/L, lactic acid 3 mmol/L. Chest x-ray (CXR) was non-acute. Computed tomography showed 2 large densities in the right hepatic lobe consistent with liver abscesses.He received vancomycin and piperacillin-tazobactam. Jackson-Pratt (JP) drains were placed in the liver abscesses. Blood and abscess cultures were positive for Streptococcus intermedius. On hospital day 3, he again became tachycardic, tachypneic, and developed diffuse wheezing and hypoxia requiring bilevel positive airway pressure. He was positive for Respiratory Syncytial Virus and CXR showed diffuse bilateral airspace opacities. He was treated with albuterol, methylprednisolone, furosemide, and metoprolol. By day 5, his respiratory distress completely resolved and repeat CXR was normal without evidence of prior opacities. At discharge, one JP drain was removed and was found to have a worm in it (Figure 1). It measured 2.5 feet in length when stretched out and its appearance was consistent with Ascaris lumbricoides. Unfortunately, the specimen was lost during transport to an outside laboratory and was unable to be definitively identified. The patient was treated with albendazole at the time of discharge and 8 weeks later and has done well since. His final diagnosis was disseminated ascariasis secondary to dupilumab immunosuppression complicated by Streptococcal hepatic abscess and bacteremia.
Discussion: The Ascaris lifecycle involves migration into the portal venous system, explaining the liver abscesses, and then into the lungs resulting in a phenomena called Löffler syndrome in which the patient develops respiratory distress with rapid resolution as the larvae move through the lung parenchyma.1,2 Despite having RSV, our patient’s spontaneous resolution of CXR abnormalities within 48-hours is more consistent with the transient nature of Löffler syndrome. His diagnosis is strengthened by the presence of Streptococcus intermedius bacteremia, which is normal flora of the gastrointestinal and respiratory tracts, likely seeded from Ascaris during its migration.3Dupilumab is an immune modulator used for atopic disease that reduces the amount of circulating IgE which is active in both atopy and parasitic infections.4,5 Although this author could not find published reports of disseminated helminth infection during dupilumab treatment, the drug manufacturer recommends treating such infections before starting the drug as it is unknown if it will affect a patient’s immune response.6
Conclusions: Despite the lack of data on current prevalence of Ascaris in Appalachia, we can infer its presence based on historical data.7 Providers should include helminth infection on their differential in patients with atypical presentation and serial imaging. This case emphasized the need for more research into how dupilumab may affect immune response to helminths and how to best manage patients on this medication who develop such infections.