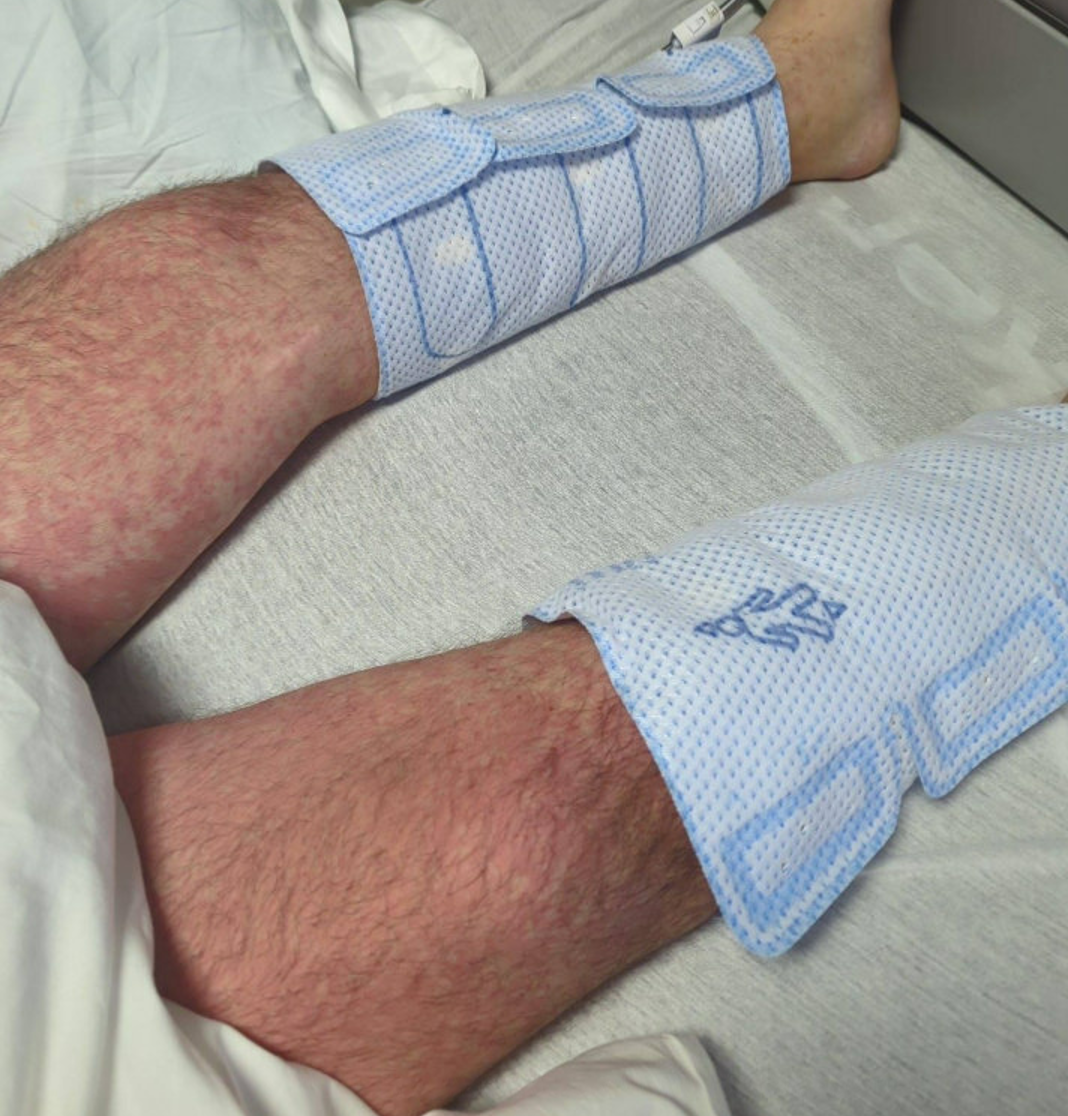
Case Presentation: A 38-year-old male with presumed seronegative rheumatoid arthritis (RA), irritable bowel syndrome with diarrhea (IBS-D), and reported Lyme disease (negative serology) presented with acute dyspnea, pleuritic chest pain, and chronic relapsing fevers. Initial treatment with broad-spectrum antibiotics failed, and he developed acute hypoxic respiratory failure, requiring transfer to the Medical Intensive Care Unit (MICU). Imaging revealed acute mediastinitis, bibasilar pneumonia, and pericarditis. Despite treatment with antibiotics, his condition deteriorated, and further infectious disease, rheumatology, and hematology workups were inconclusive. Steroids initially improved his hypoxia, but fever resurgence and a morbilliform rash upon attempted steroid taper prompted consideration of adult-onset Still’s disease (AOSD), despite atypical features. Cervical node biopsies supported an underlying rheumatic disorder, and treatment with high-dose methylprednisolone and Anakinra controlled symptoms and inflammation. The patient was transitioned to Canakinumab and Anakinra upon discharge, with a final diagnosis of AOSD complicated by peripheral macrophage activation syndrome (MAS).
Discussion: This case underscores the importance of including adult-onset Still’s disease (AOSD) in the differential diagnosis for patients with unexplained chronic arthralgia, recurrent fever, morbilliform rash, and serositis. The Yamaguchi criteria provide a structured framework for diagnosis, with major criteria encompassing persistent fever, arthralgia, and fever-dependent rash, and minor criteria such as sore throat, lymphadenopathy, hepatosplenomegaly, and negative ANA and RF serology. While the patient fulfilled several diagnostic criteria, atypical findings like mediastinitis and a fever-independent rash complicated the diagnostic process, emphasizing the variability in AOSD presentations.The progression of this patient’s condition highlights the critical need to recognize macrophage activation syndrome (MAS), a severe and potentially fatal complication of AOSD. MAS involves excessive activation of macrophages and lymphocytes, leading to a cytokine storm and multi-organ dysfunction. In this patient, features such as escalating fever patterns, hepatosplenomegaly, pleural effusions, and lymphadenopathy raised concerns for MAS. The resurgence of symptoms during steroid tapering further supported this diagnosis. Early initiation of high-dose corticosteroids and targeted biologic therapies, including Anakinra and Canakinumab, was pivotal in achieving clinical stability.
Conclusions: This case exemplifies the diagnostic challenges posed by adult-onset Still’s disease, especially when complicated by macrophage activation syndrome. It demonstrates the importance of a comprehensive and multidisciplinary approach in evaluating patients with persistent fever, arthralgia, and rash, particularly when atypical findings are present. Effective management hinges on the prompt recognition of MAS and the tailored use of corticosteroids and biologic agents. Early diagnosis and intervention are vital to improving outcomes in these complex and life-threatening conditions.