Background: The hands of hospitalists are often the source for transmitting multidrug resistant organisms (MDROs), and as such are the target of numerous hand hygiene interventions. Despite this focus, the prevalence of various MDROs on healthcare personnel (HCP) hands during routine patient care has not been well established. Therefore, we conducted a systematic review to: 1) determine the burden of MDRO prevalence on HCP hands during routine patient care and 2) understand factors that may influence hand contamination.
Methods: We performed serial searches of MEDLINE, Web of Science, CINAHL, Embase, and Cochrane CENTRAL in December of 2016 and June 2017 to identify studies that reported the culturing of HCP hands for MDROs in the hospital setting. MDROs included Methicillin-resistant Staphylococcus aureus (MRSA), Vancomycin-resistant enterococcus (VRE), Clostridium difficile (C. difficile), Acinetobacter baumannii (A. baumannii), and Pseudomonas aeruginosa (P. aeruginosa). Data abstraction and risk of bias were independently assessed by two investigators. Meta-analysis was performed to determine a pooled prevalence by organism, with further subgroup analysis by care setting, study design, geographic location, and collection method.
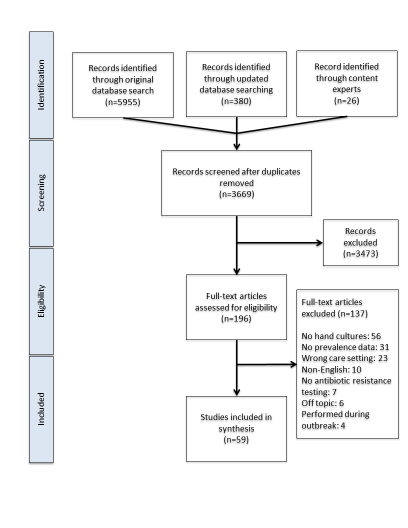
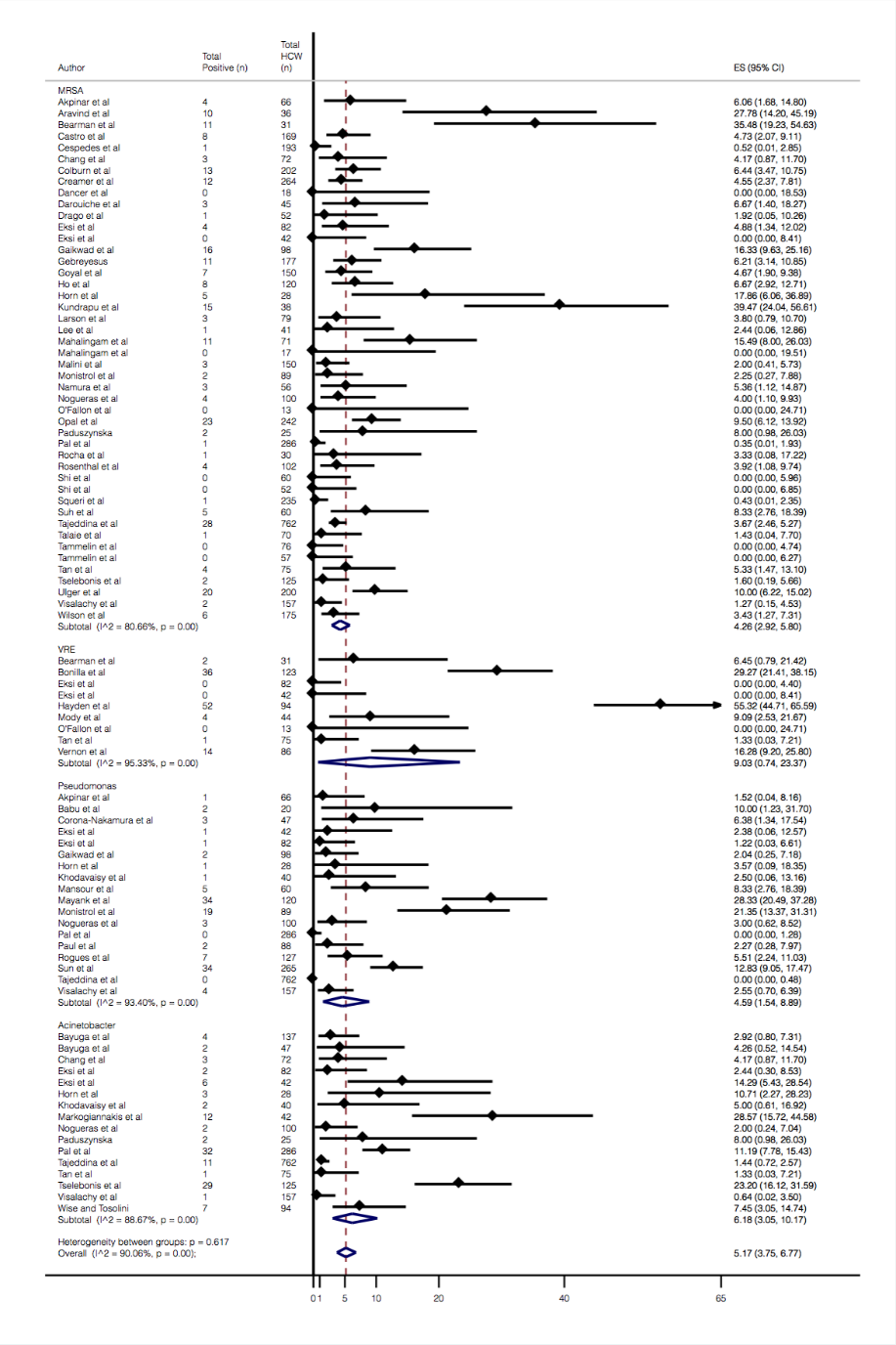
Results: Fifty nine articles were included in the review (Figure 1), comprising a total of 6,840 cultures. Study designs included cross-sectional (47), pre-post (7), randomized control (3), and mixed (2). Twenty three studies were conducted in Asia, 18 in North America, 13 in Europe, 2 each in South America and Africa, and 1 in Australia. The pooled prevalence for MRSA, P. aeruginosa, A. baumannii, and VRE were 4.26%, 4.59%, 6.18%, and 9.03%, respectively (Figure 2). Subgroup analysis was mainly limited to MRSA, as most studies (42) tested for its presence. The highest MRSA rate was observed in North America at 8.28%, twice that of Asia, the next highest at 3.96%. MRSA rates were also higher on general wards (5.14%) compared to ICU (2.20%). Comparing cross-sectional studies to all other designs, MRSA rates were 3.25% vs 12.49%. Regarding MRSA sample collection method, all were comparable at 4-7%, except for agar direct contact which was much lower at 1.55%.
Conclusions: This review demonstrates that the prevalence of MDROs on HCP hands in the hospital vary by pathogen, care setting, and geography. Furthermore, culture acquisition method and study design also appear to influence detection rates. HCP hand hygiene can be improved by utilizing this data to enhance knowledge, practice, and research surrounding hospital acquired infection prevention.