Background: Malignant bowel obstruction (MBO) is a common complication, estimated 3-15% [1], in patients with gastrointestinal and gynecologic malignancies. It is usually a sign of advanced disease and often necessitates extended hospital admission.Hospitalists are increasingly involved in treating patients with MBO and the major challenge is fragmented nature of medical care and coordination across multiple subspecialties and support staff involved in the care of patients with a MBO (oncologists, surgeons, gastroenterologists, palliative care physicians, interventional radiologists, gynecologic oncologists, dieticians, and nurses). Although MBO is a common complication, there are no guidelines on MBO treatment approaches.
Purpose: This innovation aimed to improve the immediate identification and unify the management of a MBO in an inpatient setting by creating and implementing an EMR integrated pathway, AgileMD.
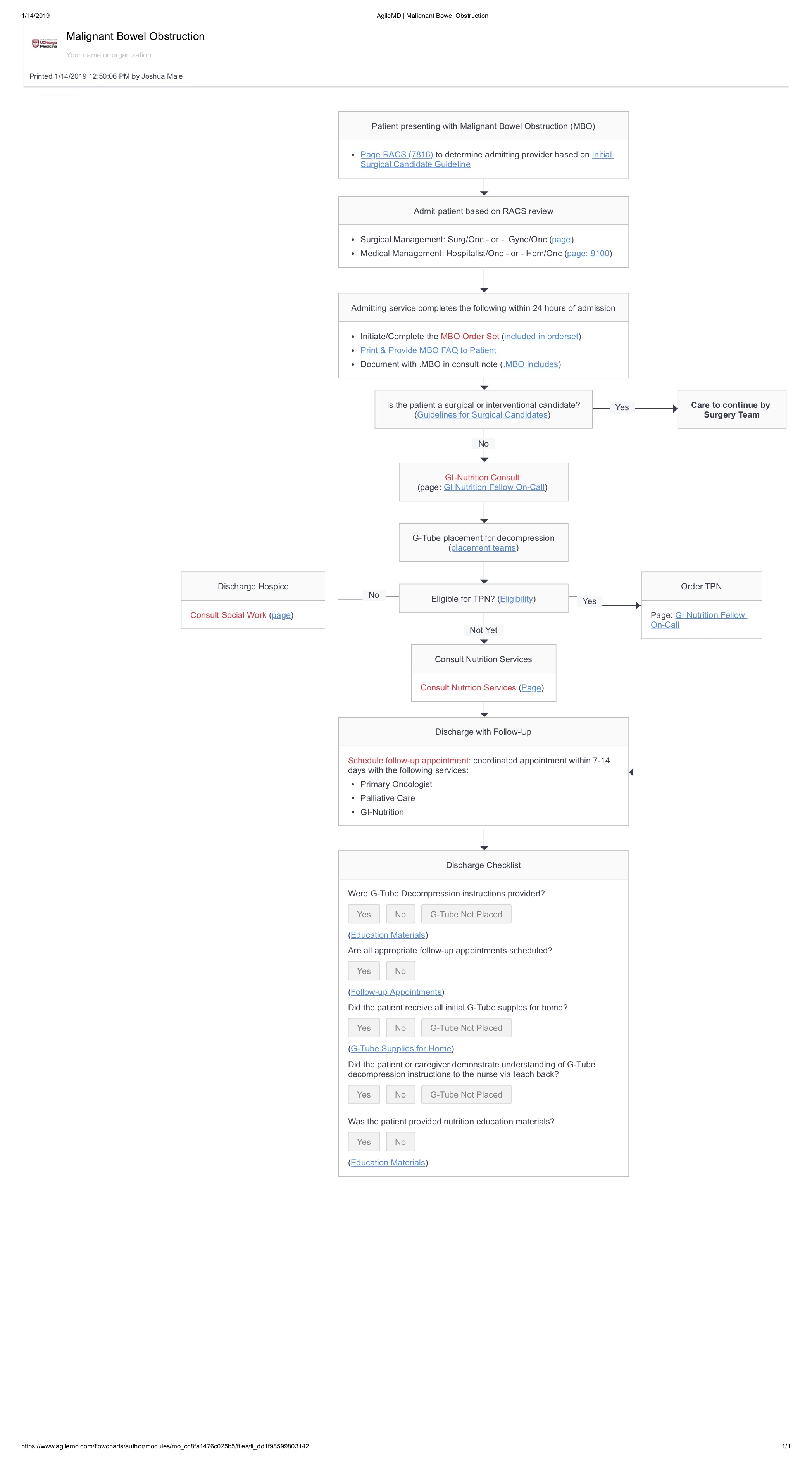
Description: To address a complex clinical challenge in the management of MBO we gathered a dedicated interprofessional MBO team consisted of surgical oncology, gynecological oncology, medical oncology, gastroenterology, interventional radiology, hospital medicine, palliative care, nutrition, and nursing. After iterative meetings from 8/2018 to 4/2019, MBO group developed the following: (1) standardized protocols for immediate identification and MBO triage (2) expert consensus MBO algorithms for the inpatient management; including specific order set (3) patient education materials. The pathway was distributed via EMR integrated web-platform, AgileMD.Since the implementation of MBO AgileMD pathway in April 2019, until September, 9th, 2019, the pathway has been activated 56 times and implemented 21 times (37.5%). Linked educational materials have been accessed 56 times (100%).
Conclusions: The creation of a comprehensive, interprofessional MBO program and implementation via EMR pathway significantly affects patient care and may improve outcomes.