Background: Laboratory testing is one of the highest volume medical activities in a health system. Despite their central role in driving clinical decision making, laboratory diagnostics are highly variable and expensive. The annual cost estimate in the U.S. for low value screening, testing, or procedures range from 17.2 billion to 27.9 billion dollars.1 Excessive laboratory testing can be painful, disturb sleep, decrease satisfaction, increase length of stay, increase transfusions, lead to venipuncture complications, and is labor intensive. Physician trainees often order extraneous labs due to a lack of understanding of what is necessary and fear of supervisor criticism. Electronic medical systems have simplified the ordering of lab tests, which can lead to recurrent ordering without much consideration.
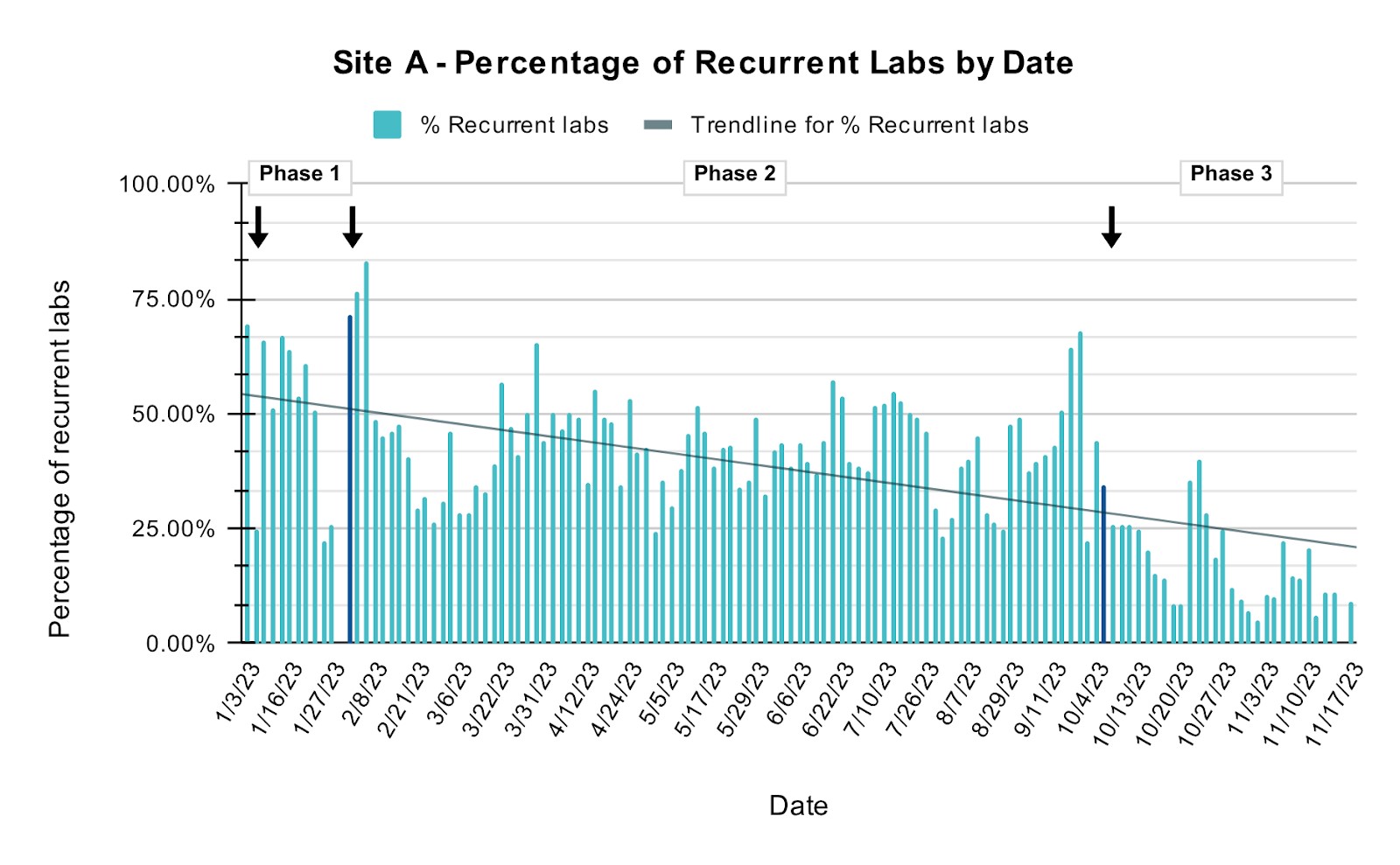
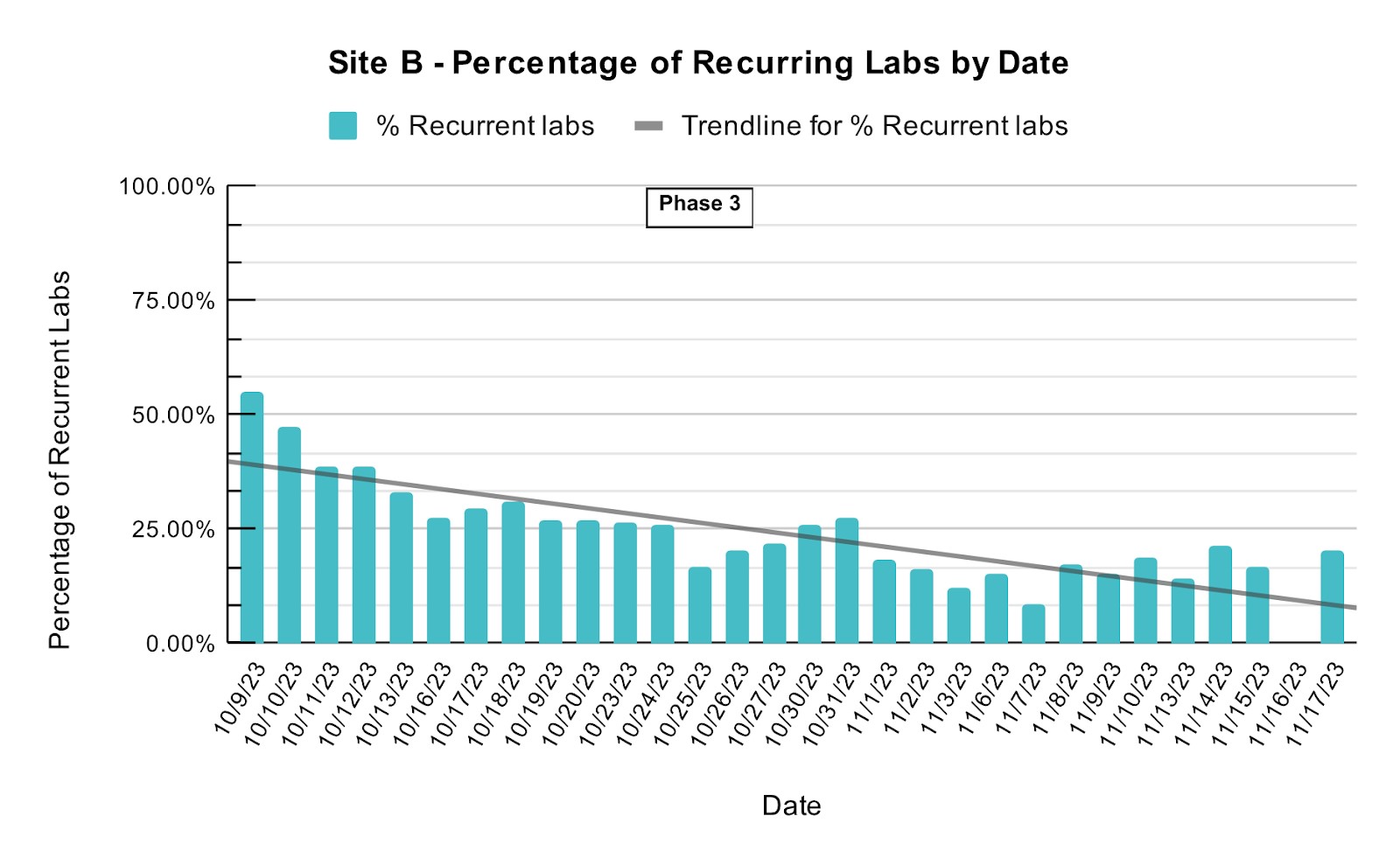
Methods: Our primary endpoint was to reduce the number of common labs ordered on the inpatient medicine services per patient by 10% over six months. Our process measure was the percent of inpatients with recurrent lab orders (labs ordered for multiple days). We created a “recurrent labs” flag in the electronic health record (EHR), audited patient charts five times a week, and provided feedback to the teams. We also queried the EHR for the total numbers of the most common venous blood studies. These included CBC, BMP, CMP, LFTs, PT/INR, APTT, Magnesium, Phosphorus, and T+S. The study was divided into three phases: Phase 1 (Jan. 3-20, 2023) established baseline data. Due to the low percentage of recurrent labs being ordered on the non-teaching service, we focused on the teaching service, where rates were much higher. Phase 2 (Jan. 20 – Oct. 4, 2023) combined chart audits, team feedback, and educational sessions for residents, advanced practice practitioners, and hospitalists to emphasize the principles of effective lab stewardship. We distributed mouse pads, chocolates, and handouts with a QR code linked to an intranet site outlining the initiative. During phase 2 we also surveyed the house staff anonymously to assess barriers in reducing recurring lab orders. Phase 3 (starting from Oct. 9, 2023) broadened the aforementioned interventions to a second site (Site B) and introduced incentives for the team with the fewest recurring lab orders over each two-week period.
Results: Between January 3rd and November 17th, we audited 10,144 charts. The mean percentage of recurrent lab orders on the teaching service at Site A fell from 57% pre-implementation (phase 1) to 42.49% and 17.08% in phases two and three, respectively. At Site B, the mean percentage of recurrent lab orders fell from 55% to 23.76% during phase 3. In the first 6 full months, the common lab orders per patient decreased by 14% at Site A over the prior year baseline, meeting our primary goal. Additionally, our House staff survey during phase 2 revealed that the most significant barrier to reducing recurring lab orders was the additional workload that is required to check lab orders daily (87%), coupled with the concern over missing information (52.2%). The most frequently recommended approach to reduce recurring labs was to take the time to discuss lab orders collectively as a team during rounds.
Conclusions: Successful strategies to improve lab stewardship included educating providers on the harms of unnecessary lab orders, understanding when to order labs, avoiding recurring lab orders, discontinuing unnecessary labs, and discussing labs on rounds. While education and constructive feedback improved the rate of recurrent labs, positive incentives were most effective.