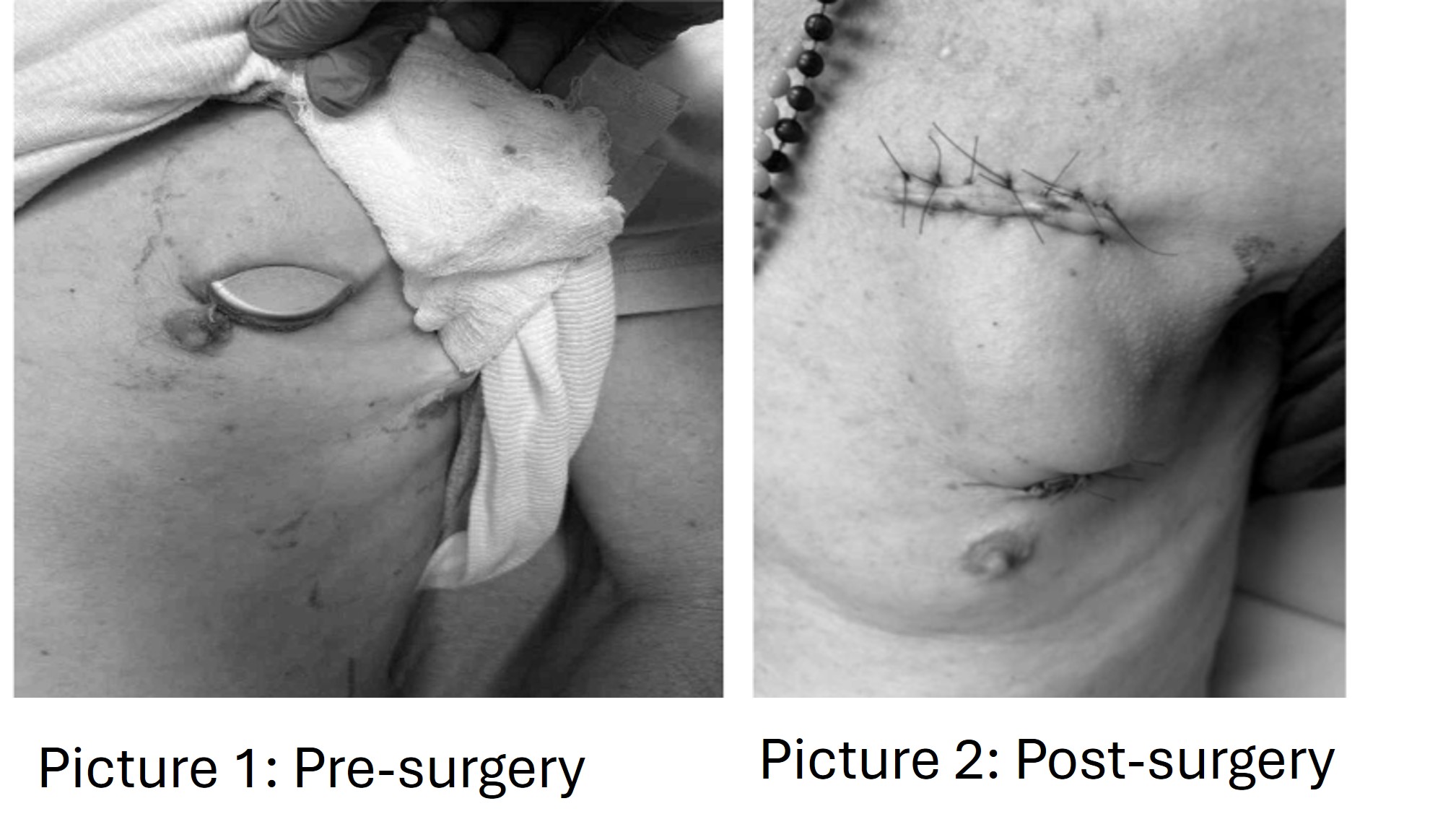
Case Presentation: A 65-year-old man with permanent atrial fibrillation on apixaban, non-ischemic cardiomyopathy, complete heart block post CRT-D implantation, prior mitral valve repair with annuloplasty ring, and bioprosthetic aortic valve replacement presented with new exposure of his CRT-D generator. His history included methicillin-sensitive Staphylococcus epidermidis endocarditis managed with long-term cefadroxil suppression.He noticed the exposure after minor trauma months earlier, but continued normal activities without symptoms. He denied fever, chills, dyspnea, or pain. Exam showed a visible generator without erythema. He was afebrile and hemodynamically stable. Labs were unremarkable; blood cultures were negative. EP and ID teams were consulted; empiric vancomycin plus ceftriaxone was started. Transesophageal echocardiography was planned.Initially, the patient requested patient-directed discharge based on his perception of clinical stability, noting that he had been engaged in everyday activities during the months his device had been exposed. After risk-benefit discussions, he agreed to percutaneous laser extraction. The CRT-D generator, two coronary sinus leads, a dual-coil defibrillator lead, and a right atrial pacing lead were removed, followed by leadless pacemaker implantation. Operative cultures grew Staphylococcus epidermidis and Corynebacterium. He received 6 weeks of IV vancomycin and oral metronidazole, then lifelong doxycycline suppression. He recovered well and resumed normal activities.
Discussion: Cardiac implantable electronic devices (CIEDs) are vital for the management of arrhythmias and heart failure. Generator erosion/extrusion occurs in 1–7% of implants and is serious, potentially fatal. Once the device breaches the skin, it is universally considered infected regardless of systemic findings. Prior reports document similar outcomes of pocket erosion and extrusion with pacing failure—all required removal and reimplantation, aligning with our management approach. This case highlights the management of CIED extrusion in a patient with multiple prior surgeries and chronic infection, emphasizing multidisciplinary care and individualized decision-making.Pacemaker extrusion represents end-stage pocket erosion and mandates complete system removal. Guidelines from the Heart Rhythm Society and the European Heart Rhythm Association stress that any exposed or infected CIED should be fully extracted, as conservative therapy carries high recurrence and mortality risk (Blomström-Lundqvist et al., 2020; Kusumoto et al., 2017). Prior reports: Nichev et al. (2009) described complete extrusion after pocket infection; Santarpia et al. (2008) reported progressive erosion; Masuno et al. (2022) noted pacing failure post-extrusion; Vijayvergiya et al. (2012) described very late extrusion without infection.
Conclusions: This case reinforces that exposed cardiac devices are presumed infected, even without systemic signs or positive cultures. Complete extraction is curative; partial removal or antibiotics risk relapse. Lifelong suppressive therapy may prevent recurrence when eradication is uncertain. Successful outcomes depend on coordinated care among electrophysiology, infectious disease, and surgical teams, guided by evidence-based practice and patient-specific considerations.