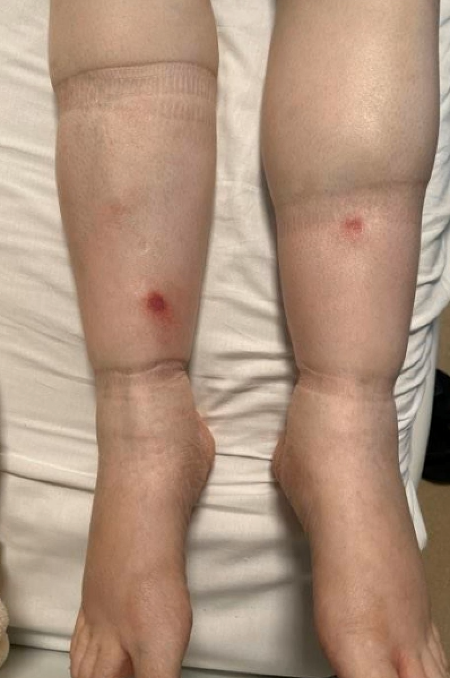
Case Presentation: A 54-year-old woman with a history of uterine fibroids developed six weeks of progressive abdominal swelling and unintentional weight loss. Initial supportive care at an outside clinic failed to relieve symptoms. A month later, abdominal CT scan demonstrated extensive peritoneal carcinomatosis with bulky retroperitoneal adenopathy, moderate intra- and extrahepatic ductal dilatation, featureless pancreas, and moderate bilateral pleural effusions. She was referred to the Emergency Room for further workup. Physical examination revealed trace scleral icterus and jaundice, decreased breath sounds in bilateral lung bases, and positive abdominal fluid wave. The patient’s lipase was 409, total bilirubin 5.6, alkaline phosphatase 436, INR 1.3, CA-19-9 and LDH elevated at 54 and 2,7466, respectively, CA-125 and CEA negative. She received IV furosemide for suspected pulmonary edema, and CT guided biopsy of a left retroperitoneal lymph node was performed on third day of hospitalization. On the morning of the procedure, the patient reported erythematous, indurated, circular, subcutaneous nodules on bilateral shins (see image). Punch biopsy of a shin lesion showed: subcutaneous fat necrosis, suppurative inflammation, and evidence of saponification, with AFB, PAS, Gram and Giemsa stains negative for infectious organism. Overall clinical picture and pathology were consistent with pancreatic fat necrosis. Given absence of pancreatic abnormalities (other than elevated lipase), ERCP and EUS were deferred pending biopsy results. On day five of hospitalization the lymph node biopsy showed preliminary B-cell lymphoma, and subsequent immunohistology confirmed Diffuse large B-cell lymphoma, germinal center type. Treatment was initiated with intravenous corticosteroids and R-CHOP chemotherapy and patient transferred to the Hematology-Oncology team for continued care. The patient’s liver enzymes and abdominal symptoms improved, and she discharged home for continued outpatient management.
Discussion: This case illustrates the importance of physical exam to the clinical reasoning process and highlights a rare skin manifestation of undiagnosed malignancy. Subcutaneous fat necrosis, also known as “pancreatic panniculitis” (PP), is a rare skin condition most frequently associated with acute or chronic pancreatitis, pancreatic carcinoma or neuroendocrine tumor (specifically of the adrenal gland). The differential diagnosis for PP is broad and includes erythema nodosum, neutrophilic dermatoses including Sweet syndrome, nodular vasculitis, and infectious as well as non-infectious (e.g., sarcoid) panniculitides. Pathogenesis of PP may be secondary to focal lipid necrosis and inflammatory reaction related to circulating high levels of pancreatic enzymes, whether benign or malignant in etiology. Large B-cell lymphoma rarely presents as acute pancreatitis, but pancreatic panniculitis from non-pancreatic lymphoma has been reported only in intravascular subtypes. PP skin lesions often precede symptoms of underlying disease or malignancy by several months, and while rare, early recognition of this condition may lead to more timely diagnosis and treatment of malignancy.
Conclusions: Subcutaneous fat necrosis (pancreatic panniculitis) has infrequently been described in nonpancreatic and extranodal malignancy. Skin manifestations of undiagnosed malignancy may provide important clues for timely diagnosis in challenging cases.