Case Presentation: A 31-Year old Caucasian female with a history of skin biopsy proven Sweet’s syndrome presented with rapid worsening of left-sided periorbital redness, swelling, proptosis, and binocular diplopia. No fever or chills. On physical exam, extra ocular movements were intact. Pupils were equal, round and reactive to light and accommodation. Visual acuity and fields were normal.Lab tests were negative for ANA, ds DNA, SSA/SSB, SCL 70, Jo 1, Ribosomal P, CCP antibodies. Normal CPK /RF levels/sed rate/CRP. Normal IgG subclass levels.
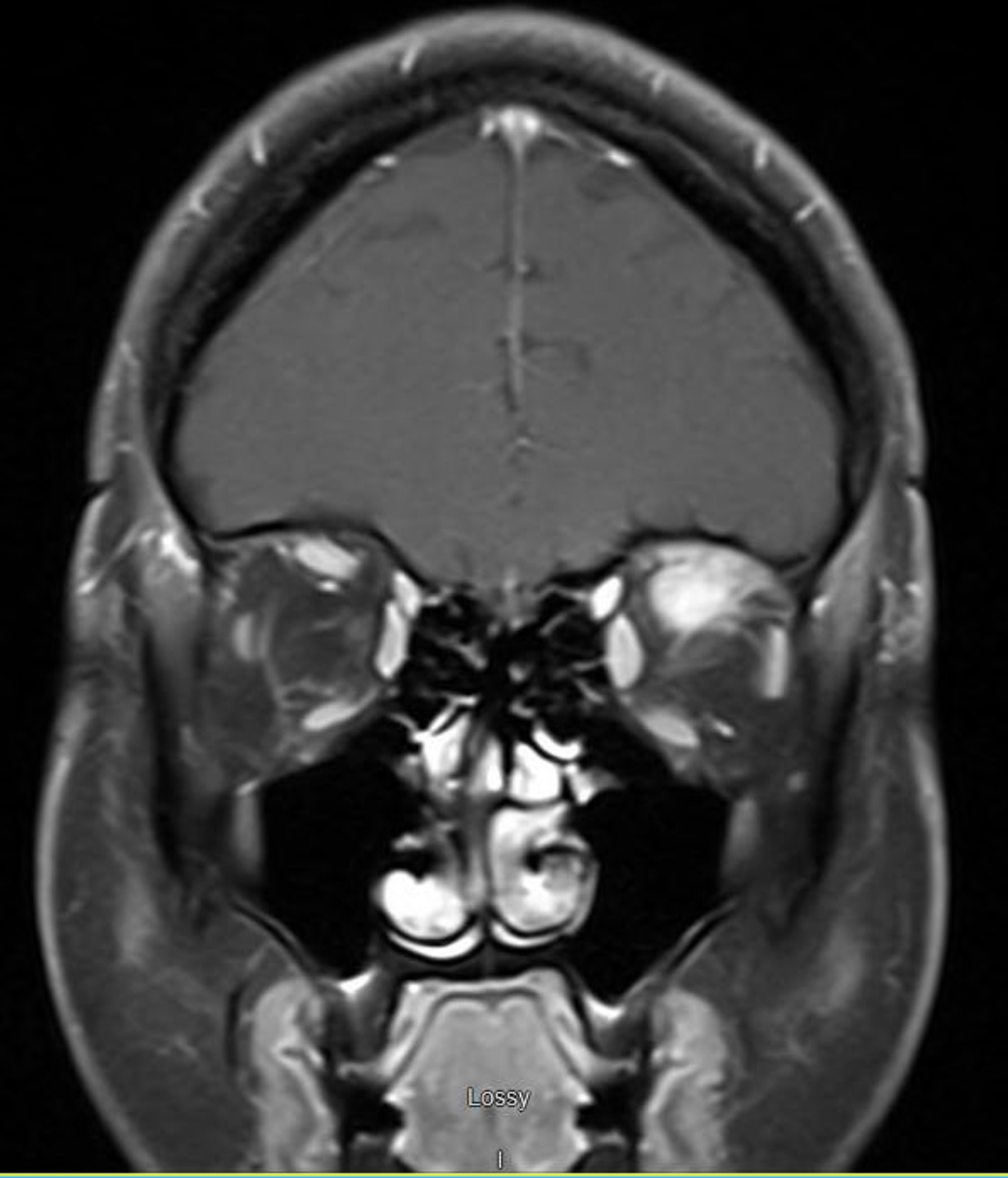
MRI of brain and orbit demonstrated 27x12x8.2 mm mass-like enhancement in the superior part of the left orbit involving the left superior rectus muscle. This exerted mass effect on the infraorbital segment of the left optic nerve. Infectious work up was negative. CT of the neck, chest, abdomen, and pelvis were negative for lymphadenopathy or similar lesions.
Patient was diagnosed with compressive neutrophilic lesion, a rare complication of Sweet’s syndrome. Biopsy was not performed because of difficulty with access to the lesion.
Treatment was started with high dose of oral prednisone at 80 mg daily and intraocular Kenalog. Patient’s ophthalmic symptoms improved. Treatment continued with Methotrexate as steroid sparing agent along with Hydroxychloroquine and colchicine. 6 months later, patient relapsed and had difficulty tapering prednisone below 20 mg. She has been treated with rituximab with good response.
Repeat MRI of brain showed regression of the orbital mass.
Discussion: Sweet’s syndrome is a rare inflammatory disease, characterized by sudden onset painful and erythematous plaques, fever and neutrophilia. It can be associated with extra cutaneous involvement. We report a case of Sweet’s syndrome with a posterior orbital compressive mass. To our knowledge, there has been only one similar case report by Koay et al in 2013. They presented a case of compressive optic neuropathy and blurry vision.Our patient presented with diplopia, which is a unique presentation of Sweet’s syndrome. The first step in management is to exclude differential diagnoses such as lymphoma.
Corticosteroid is first line treatment for Sweet’s syndrome. Local and small lesions can be treated with topical or intralesional corticosteroids. In our patient, clinical finding, lab results, and quick improvement after steroid treatment further supported diagnosis of orbital lesion secondary to Sweet’s syndrome.
Recent data has shown efficacy of biologic agents such as Anakinra, Rituximab in treatment of recurrent or refractory Sweet’s syndrome
Conclusions: Posterior orbital lesion is a unique manifestation of Sweet’s syndrome. Patient can present with diplopia and proptosis (secondary to extraocular muscles involvement) or blurry vision (secondary to compressive optic neuropathy). Lesion usually respond promptly to corticosteroids. In refractory or recurrent cases, Rituximab is an alternative.