Background: Opioid use disorder (OUD) is a major public health challenge. Medications for opioid use disorder (MOUD) are effective and life-saving treatments.(1) Unfortunately, a minority of OUD patients receive MOUD.(2) Over the past decade, there have been several implementation efforts to address this, including inpatient addiction medicine (AM) consult services and removal of the DEA X-waiver.(3-5) Our objective was to examine the frequency of MOUD receipt among OUD patients at our institution over the past six years and the impact of these efforts.
Methods: A retrospective cohort study of OUD patients admitted from July 2018 to June 2024 to an academic, tertiary care hospital located in the Midwest. Participants were included if they were (1) between 18 and 85 years of age, and (2) have at least one of the following: (i) an active problem list entry for opioid-related disorder at the time of admission (ICD-10 F11.*), or (ii) received an encounter diagnosis for opioid-related disorder before or during admission (ICD-10 F11.*), or (iii) a positive urine drug screen (with or without confirmatory test) for fentanyl during the encounter or up to six months prior to the encounter. Descriptive statistics and multivariable logistic regression were used to examine predictors of MOUD use. Patients were classified as receiving MOUD if they were administered at least one dose of buprenorphine or methadone during their hospital encounter. At our institution, AM consults are shared between psychiatry and medical toxicology consult services. Patients were considered to have received an AM consult if they had a completed consult order for either psychiatry or toxicology. When a patient had repeat hospitalizations during the study period, we randomly selected one hospitalization per patient.
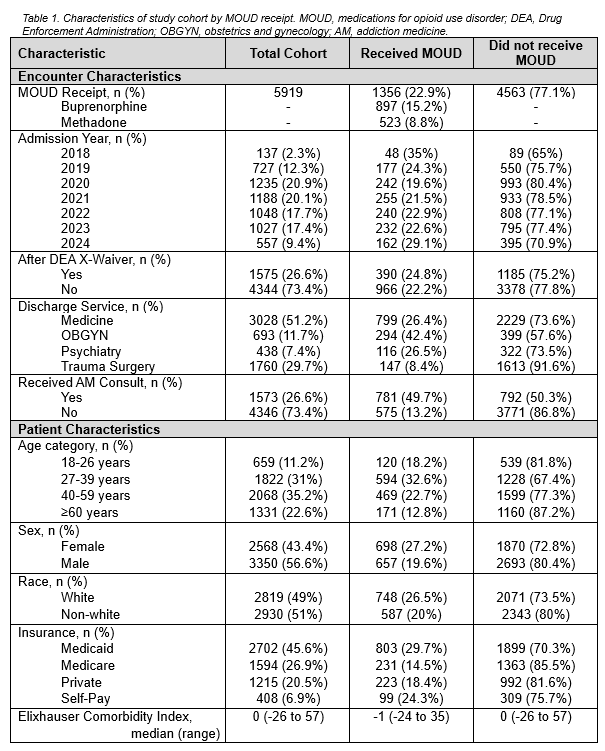
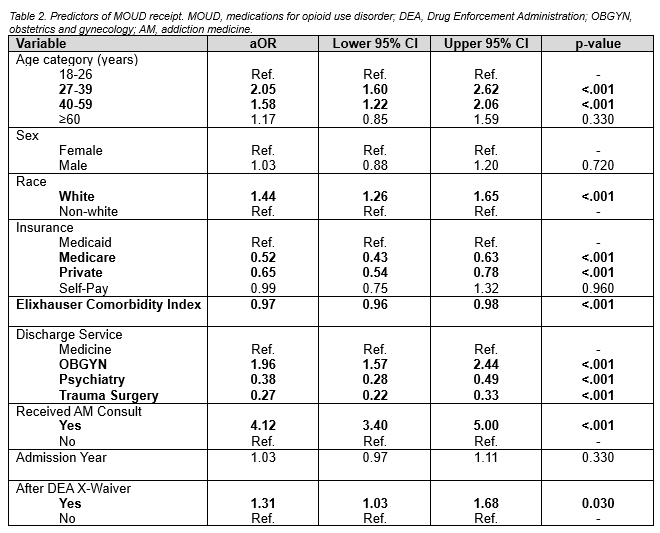
Results: 5,919 patient encounters were included in the analysis. Patients were predominantly between 27-59 years in age (3,890, 66.2%), non-white (2,930, 51.0%), and men (3,350, 56.6%). A minority of patient encounters received MOUD (1,356, 22.9%). More patients received buprenorphine (897, 15.2%) compared to methadone (523, 8.8%). AM consultation was strongly associated with an increased odds of MOUD receipt (aOR 4.12, 95% CI 3.40 to 5.00, p-value < 0.001). Compared to patient encounters on the medicine service line, patient encounters on the OBGYN service had a greater odds for MOUD receipt (aOR 1.96, 95% CI 1.57 to 2.44, p-value < 0.001). Patient encounters on psychiatry (aOR 0.38, 95% CI 0.28 to 0.49, p-value < 0.001) and trauma surgery (aOR 0.27, 95% CI 0.22 to 0.33, p-value < 0.001) service lines were associated with a lower odds of MOUD receipt.
Conclusions: A minority of patients received MOUD. AM consultation and specialty service lines strongly predicted inpatient MOUD use. Future research should explore how clinicians can work together, across specialties, to improve MOUD implementation.