Background: Patients with a pre-existing diagnosis of advanced cancer who discharge to a skilled nursing facility (SNF) after an acute care hospitalization rarely receive future oncologic treatment, have high readmission rates, and minimal hospice use. We aimed to evaluate survivorship of patients discharging to a SNF with a new diagnosis of cancer based on their subsequent clinical trajectory after an acute care hospitalization.
Methods: We conducted a population-based cohort study using the Surveillance, Epidemiology, and End Results (SEER)-Medicare database of patients newly diagnosed with stage II – IV colorectal, pancreatic, urinary bladder, or lung cancer between 2011-2013 who had an acute care hospitalization and discharged to a SNF. A total of 6,791 cases were identified and patient groups of interest were compared descriptively using means and standard deviations for continuous variables and frequencies and percentages for categorical variables. Cox proportional hazards analysis was performed to estimate the Hazard Ratio (HR) of death (ratio of conditional probabilities of death given alive) by clinical trajectory. Subsequent clinical trajectories were categorized into 4 groups: 1) no treatment and no hospice 2) no treatment and hospice 3) treatment and no hospice and 4) treatment and then hospice.
Results: After discharge to the SNF, 45.7% of patients received no treatment and no hospice (43% of whom died within 6 months), 25% received no treatment and hospice (88% died within 6 months), 20.8% received treatment and no hospice (29% died within 6 months), and 8.5% received treatment and hospice (85% died within 6 months). The 4 groups were largely similar, except patients with no treatment/no hospice were much more likely to have colorectal and stage II/III cancer than patients who receive treatment and then hospice. Adjusting for covariates in Cox model, HRs compared to patients with treatment/no hospice are 1.6 (for no treatment/no hospice), 2.1 (treatment/hospice), and 2.9 (no treatment/hospice).
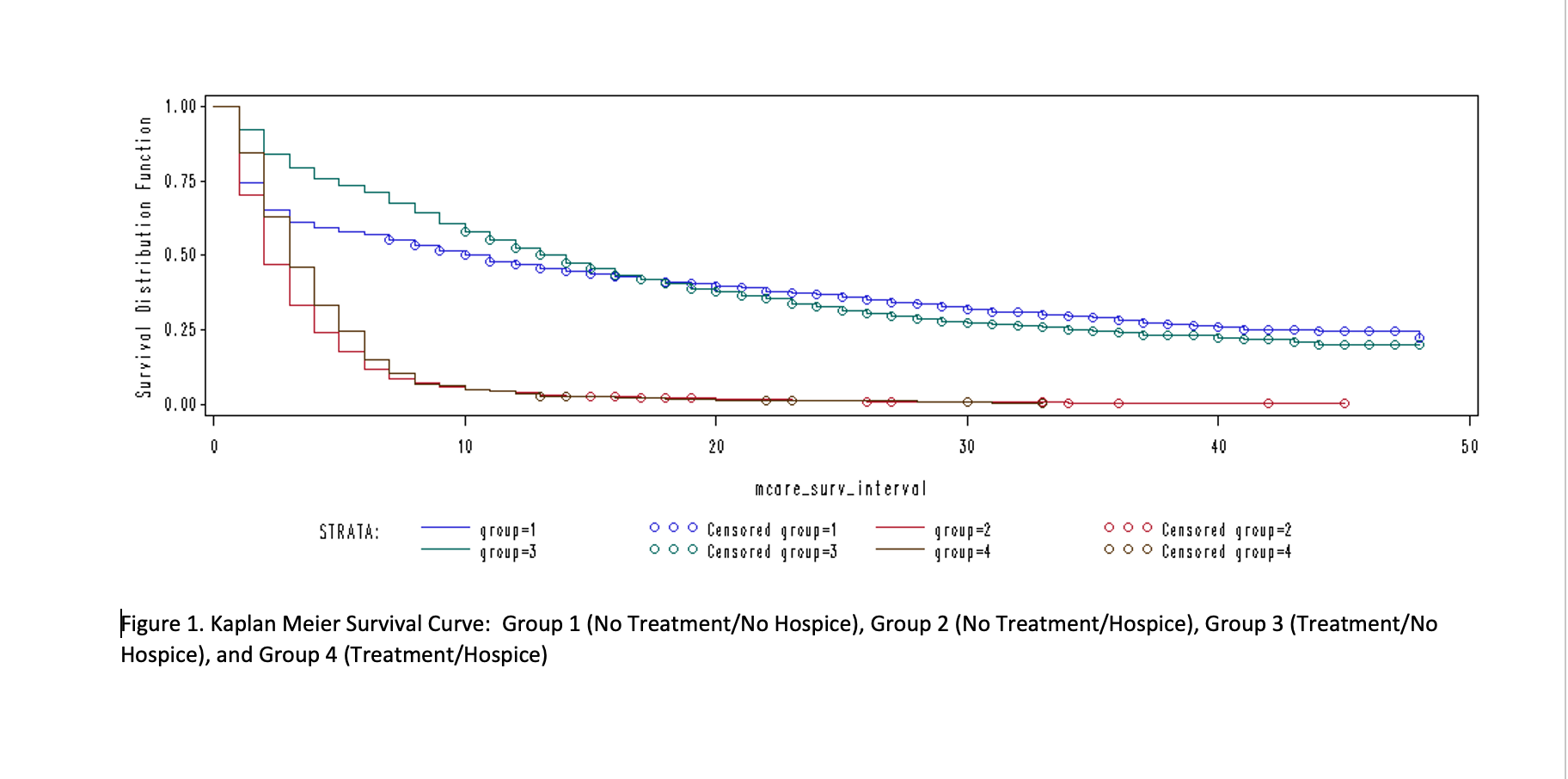
Conclusions: Seventy one percent of patients diagnosed with new cancer during an acute care hospitalization do not go on to receive further cancer treatment after discharge to a SNF. Patients in group 1 (no treatment, no hospice), group 2 (no treatment, hospice) and group 4 (treatment and then hospice) had decreased survival (about 50-200% more chance of dying if alive) compared to patients in group 3 (treatment, no hospice), where differences between groups 1 and 4 becoming small after adjusting for patient characteristics. These findings suggest that patients with a new cancer diagnosis discharging to a SNF are unlikely to benefit from the rehabilitative intent of skilled nursing facility care. Next steps include better understanding patient goals of care when discharging to a SNF and developing and implementing targeted palliative care delivery models in the SNF setting.