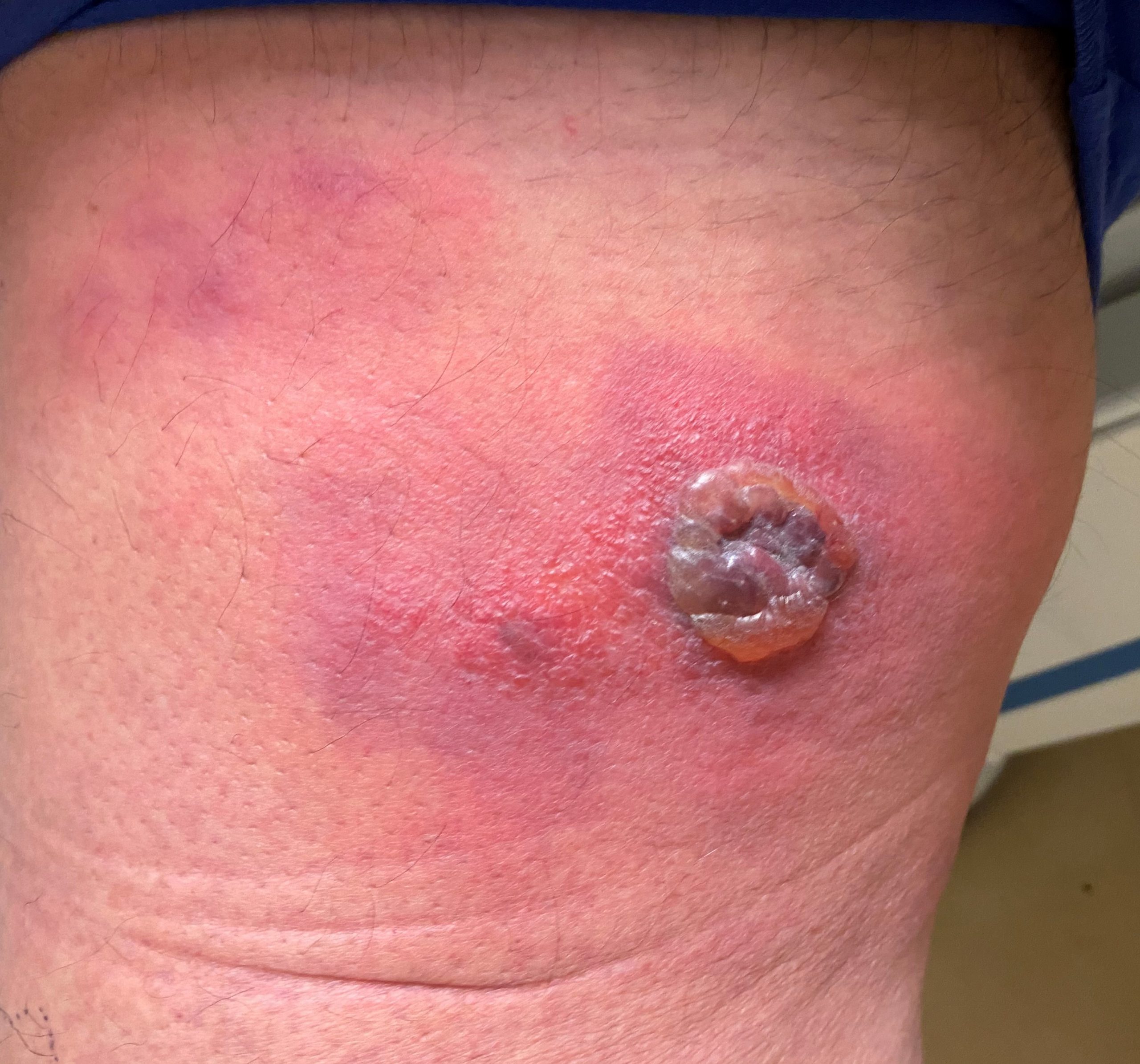
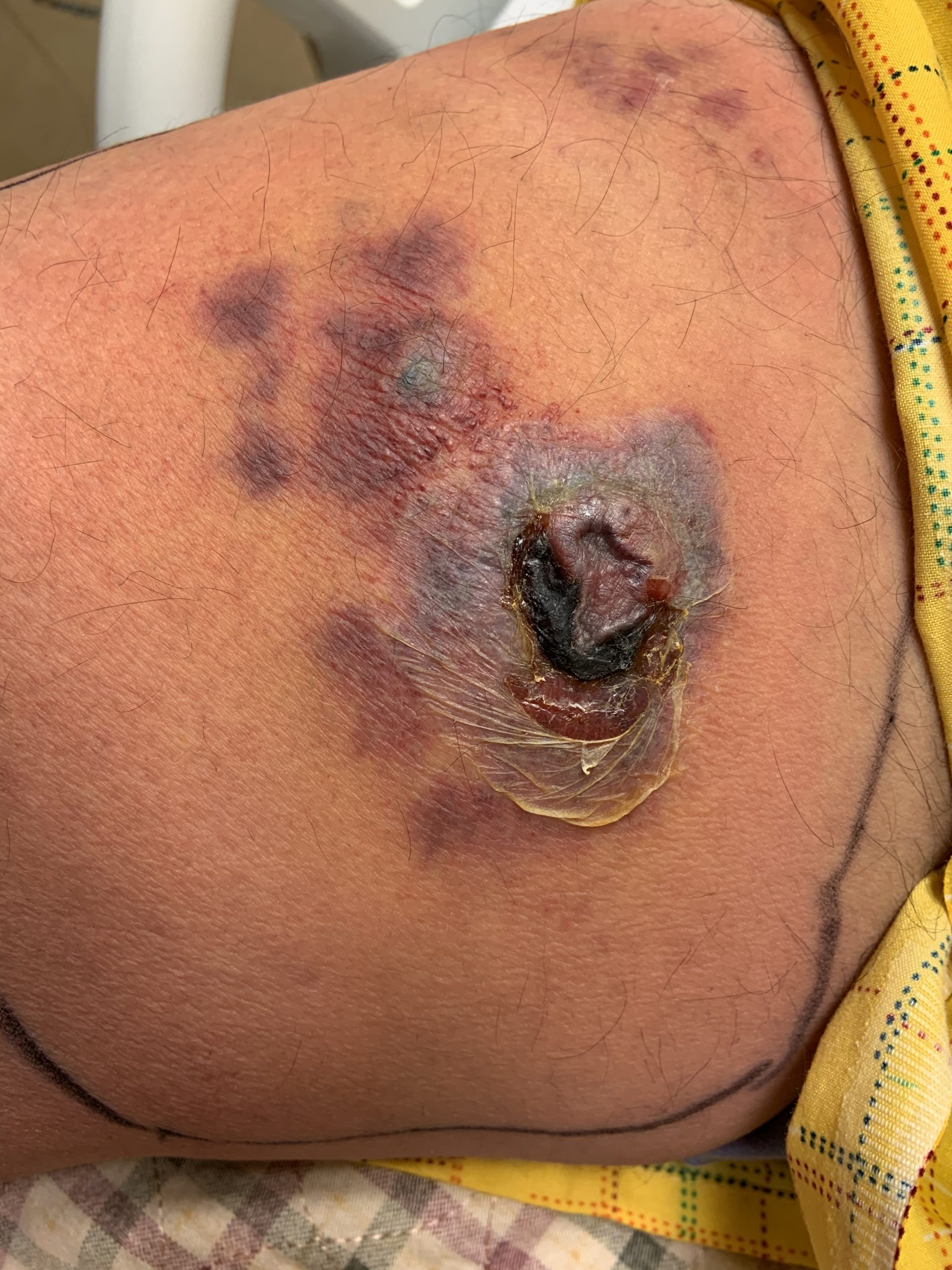
Case Presentation: A 63-year-old Hispanic male with relapsed refractory IgD-kappa plasma cell myeloma on 5th line salvage chemotherapy and remote high-grade invasive papillary urothelial carcinoma / prostatic adenocarcinoma status post cystoprostatectomy three years prior was admitted to the hospital for evaluation of a fall and sepsis secondary to cellulitis. The patient reported that he noticed a new skin lesion on his right inner thigh three days prior, that he takes rivaroxaban daily, and that his last chemotherapy infusion was nine days ago. Initial vitals showed temperature of 100.9 F, pulse of 98, blood pressure of 102/62, and SPO2 of 99%. Physical exam was significant for an un-accessed right implanted subclavian port, non-infected right urostomy bag, and an 8 x 5 cm erythematous indurated rash surrounding centrally grouped violaceous vesicles located on the medial right thigh. Emergent CT head imaging was negative for acute neurological processes and confirmed presence of known skull lytic lesions. The trauma team cleared the patient and initial bloodwork reported WBC of 15,300 (ANC 11,600) with lactic acid of 2.64. Blood cultures were collected with prompt initiation of fluids and broad-spectrum antibiotics. Rapid PCR-based blood culture identification returned positive for Pseudomonas aeruginosa initially, as did conventional blood cultures later. Over the next few days, the underlying erythema increased in size to 12 cm diameter initially before improving, but the central lesions worsened, now demonstrating a central area of eschar and necrosis. Repeat blood cultures were drawn and an ultrasound was performed, ruling out an abscess. General surgery was consulted, who recommended getting a biopsy and potential debridement, seconded by oncology due to suspected insect bite and envenomation etiology. After reviewing the infectious disease specialist and primary team’s assessment that the lesion was likely a case of ecthyma gangrenosum, the patient declined any surgical interventions, opting to further monitor the lesion. With continued antipseudomonal medical management, the lesion demonstrated improvement, and the patient was discharged on oral levofloxacin once blood cultures from the implanted port returned negative.
Discussion: Ecthyma gangrenosum is a relatively uncommon clinical manifestation of Pseudomonas aeruginosa bacteremia that presents with skin lesions which can progress quickly from painless macules and surrounding induration to pustules/bullae with gangrenous ulcers. While the condition has been observed in non-pseudomonal bacterial infections, it is most commonly associated with pseudomonal species in immunocompromised patients. As is seen in this case, the rapidity of lesion evolution and disconcerting appearance can lead to aggressive interventions that may not be medically necessary, as a thorough review of the patient’s history and multi-specialty team approach can identify more likely etiologies consistent with individual patient risk factors. Once the diagnosis is suspected and/or confirmed, ecthyma gangrenosum typically responds to antipseudomonal antibiotic therapy, rarely requiring additional intervention.
Conclusions: When the etiology is unknown, a careful review of the patient’s history and individual risk factors empowers the hospital provider to identify the etiology with the highest likelihood and subsequently recommend the most appropriate course of action in pursuit of the diagnosis and management.