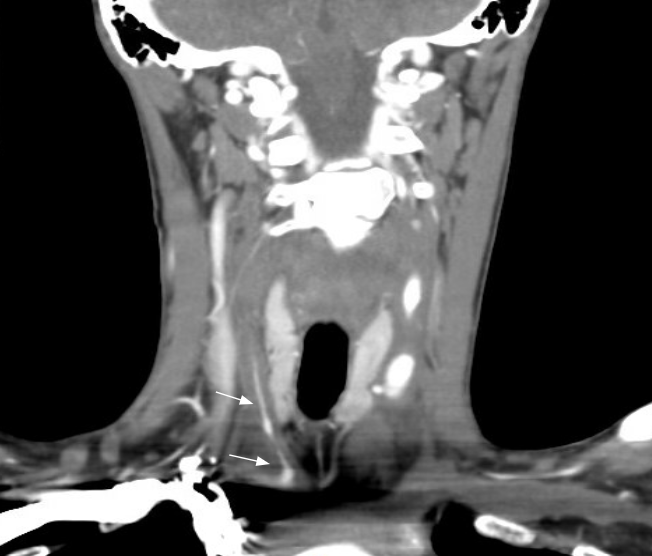
Case Presentation: A 23-year-old woman with juvenile idiopathic arthritis, large vessel vasculitis, and prior pulmonary embolism presented with progressive dyspnea, fatigue, and hemoptysis. Diagnostic evaluation revealed large vessel vasculitis and right-sided pneumonia on imaging; echocardiography showed a dilated left ventricle with global hypokinesis, severe aortic insufficiency (ejection fraction 39%), and moderate hypertrophy. Her cardiac catheterisation confirmed moderate pulmonary hypertension, significant aortic regurgitation, and nonobstructive coronary disease. She was initiated on tocilizumab and oral prednisone taper for treatment of her acute aortitis. Aortic valve replacement was deferred due to active inflammatory disease, and she was discharged with outpatient rheumatology and cardiology follow-up. Seven days post-discharge, she was readmitted with acute decompensated heart failure requiring emergent intubation and transfer to the cardiovascular ICU for refractory heart failure (BNP >25,000 pg/mL). Following multidisciplinary evaluation by cardiology, cardiothoracic surgery, and rheumatology, she underwent emergent TAVR with a 34mm Medtronic Evolut valve. Given her active vasculitis, young age, and prohibitive surgical risk, TAVR was favored over traditional surgery. Post-procedure management included a steroid taper, mycophenolate mofetil, and tocilizumab infusions, which resulted in a remarkable clinical recovery, with an improvement in ejection fraction from 40% pre-TAVR to greater than 56% at one-year follow-up.
Discussion: The overlap of juvenile idiopathic arthritis and TA is uncommon but significantly increases risks of cardiovascular morbidity through chronic inflammation, accelerated atherosclerosis, and valvular complications. Severe AR in TA results from chronic inflammatory involvement of the aortic root and valve apparatus, leading to progressive left ventricular dysfunction. ACC/AHA guidelines recommend urgent intervention for symptomatic severe AR with LVEF < 55% to prevent irreversible myocardial damage.While SAVR is the traditional gold standard, ongoing inflammation in TA increases the risk of prosthetic valve complications. TAVR represents a viable alternative in high-risk patients, though its application for isolated AR presents technical challenges.This case underscores the importance of multidisciplinary collaboration among rheumatology, cardiology, and cardiac surgery, with vigilant monitoring of disease activity and valve function. It contributes valuable data to the limited literature on TAVR in TA, demonstrating feasibility and excellent outcomes with individualised, evidence-based management. Early recognition of TA-associated AR and timely intervention can prevent irreversible heart failure progression, with TAVR offering a promising option in appropriately selected high-risk patients requiring careful perioperative planning.
Conclusions: As TAVR technology advances, its role in managing valvular complications of inflammatory large vessel disease warrants further investigation. This case supports consideration of TAVR in young, high-risk patients with active vasculitis when immediate intervention is necessary. Prospective studies are needed to define optimal timing, patient selection criteria, and long-term durability of TAVR in this unique population.
.png)