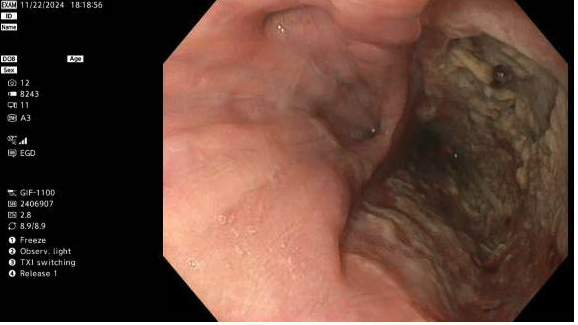
Case Presentation: Patient is an older female with PMHx of HTN, hypothyroidism, anxiety, who presented to an outside hospital with 2 weeks of SOB, DOE and RLE swelling. In the OSH, RLE Doppler revealed a DVT and she was found to have bilateral PE with moderate interstitial pulmonary edema. She also reported symptoms of dark ‘Coca-Cola’ colored urine. Renal biopsy revealed pauci-immune glomerulonephritis concerning for vasculitis and pulmonary renal syndrome. The patient developed worsening respiratory distress. Bronchoscopy performed revealed diffuse alveolar hemorrhage. CT chest performed due to ongoing cough with sputum production that revealed a posterior mediastinal fluid collection concerning for esophageal perforation. Patient was transferred for a higher level of care. Upon arrival, EGD confirmed the presence of a large perforation in the mid esophagus. A repeat EGD two days later was done to place an endoluminal sponge for vacuum therapy of the perforation with the plan to perform an EGD every 3-4 days to replace the sponge to promote perforation closure.12Then, the patient started to complain of severe abdominal pain. KUB findings were suggestive of intraperitoneal air. Follow up CT revealed a large volume pneumoperitoneum centered in the upper abdomen. Based on the location and distribution of the pneumoperitoneum, a stomach or duodenal perforation was suspected. The patient was sent for a diagnostic laparoscopy. Initial findings showed inflammatory adhesions of small bowel and colon to the anterior abdominal wall in the RLQ that was unable to be dissected, so the procedure was converted to an ex-lap with peri-umbilical incision. A punctate hole was noted in the sigmoid colon, so wedge resection of the sigmoid was performed. Stamm gastrostomy was performed given the esophageal perforation with no enteral access. An end colostomy was created, and the abdomen was closed.
Discussion: Granulomatosis with polyangiitis (GPA) is a vasculitis caused by the formation of antibodies against proteinase-3, resulting in inflammation of small and medium vessels. Patient typically present with manifestations dependent on the vessels affected. The typical triad of GPA includes necrotizing vasculitis of small arteries, upper/lower respiratory tract manifestations, and pauci-immune glomerulonephritis.The small arteries of the esophagus include the inferior thyroid artery, esophageal branch of the thoracic aorta, and the left gastric artery3. Involvement of the GI tract is rare but has been reported in the literature. In Eriksson et. Al, 6.5% (14/216) of patients with GPA had GI manifestations, with abdominal pain and GI bleeding being the most common manifestations4. Ledo and Petho describe a case in which an 18-yr old male patient presented with GI symptoms (abdominal pain, vomiting, diarrhea)5. This patient was initially diagnosed with IBD, which delayed the proper immunosuppressive therapy.
Conclusions: GPA is a vasculitis that causes vascular inflammation in small to medium vessels. GPA commonly presents with renal, pulmonary, and ENT symptoms, but can affect any small to medium-sized vessels. This case demonstrates the potential of GI complications via in patients with GPA and the importance of monitoring patient’s symptoms while hospitalized to determine the severity of the vasculitis and intervene when necessary to avoid severe complications. This case emphasizes the importance of prompt initiation of systemic corticosteroid therapy to prevent disease progression and multi-system involvement.