Background: Physicians spend more time on documentation and less on direct patient care. Burnout and career disengagement have been linked to time spent documenting in the electronic health record. A scribe program could reduce the documentation burden on hospitalists, increase revenue capture and improve the efficiency of the admission process.
Purpose: We implemented a prospective 20-week scribe pilot pairing hospitalists on admitting shifts with a scribe. Baseline and post-intervention surveys measured physician satisfaction (n=17). We also measured number of patients seen per shift, number of patients waiting to be seen at end of shift and Relative Value Unit (RVU) capture. Emergency department throughput was measured by the time from which an emergency department provider made the decision to admit (ADT9) to the time when the admitting provider placed a bed request order (ADT1), as well as the ADT9 to emergency department departure time.
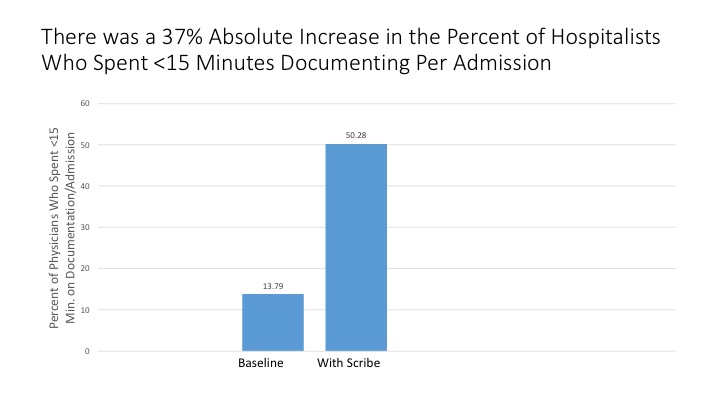
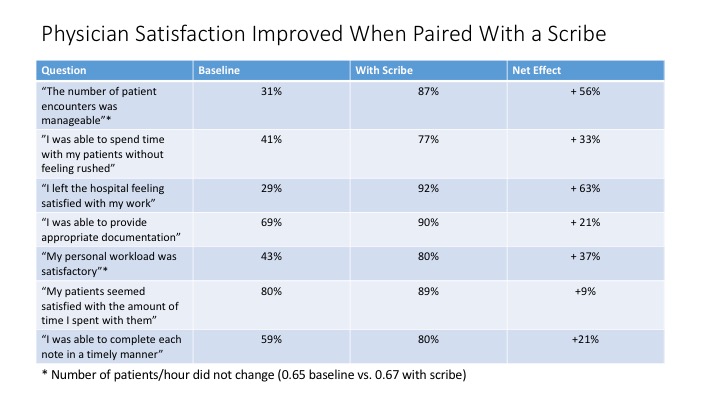
Description: At baseline, only 13% of hospitalists reported spending less than 15 minutes on documentation per admission. After the pilot, 50% of hospitalists reported this when paired with a scribe. There was also an increase in the percent of hospitalists who reported spending time with patients without feeling rushed (41% vs. 77%), an increase in the percent of hospitalists who completed their admission shift satisfied with their work (29% vs. 92%), and an increase in the percent of hospitalists who were satisfied with their documentation (69% vs. 90%). Significantly, there was a 56% absolute increase in the percent of hospitalists who felt the number of patient encounters was manageable (31% vs. 87%), while the actual number of patients was similar (0.65 patients/hour at baseline vs. 0.67 patients/hour).
There was no difference in the number of patients waiting to be seen at end of shift or RVUs per patient, but there were improvements in emergency department throughput. ADT9-ADT1 times decreased by almost 10% (36 minutes vs. 32.5 minutes), while ADT9-Emergency department departure times decreased by nine minutes (127 minutes vs. 118 minutes).
Conclusions: Pairing hospitalists with scribes during admitting shifts led to a reduction in time spent on documentation without any decrease in RVUs. It was also associated with a perception of a more manageable census despite the number of patient encounters being the same. Emergency department throughput was also faster, which has the potential to improve revenue and patient satisfaction.