Background: As of 2017, 96% of non-federal acute care hospitals had an electronic health record (EHR). Hospitalists interact with the EHR for several hours each day. Many studies have suggested a direct correlation between physician burnout and frustrations with the EHR. Data has been published regarding physician time studies in the outpatient setting, but there is a paucity of data regarding time spent in the EHR in the inpatient setting. We sought to understand the variability in efficiency and opportunities with the EHR in our hospital medicine (HM) group.
Methods: Data for 19 days in September 2018 was obtained from our EHR vendor, Epic, that tabulated the time each hospitalist in our large, academic safety net hospital spends with the EHR as mean active minutes. The number of notes completed was also reported. We then calculated the mean number of minutes spent per note over the study period which we extrapolated to time spent in the EHR to care for 14 patients – our average daily patient census. We then used these efficiency data to stratify the physicians to quartiles. We compared mean efficiency of 1st quartile and 4th quartile physicians and estimated time opportunity of improving efficiency of all to 1st quartile. Using MGMA data, we converted time opportunity into FTE and dollars. We then correlated the time spent in the EHR with years of experience. We excluded physicians on teaching services, nocturnists, and physicians whose primary role was admissions.
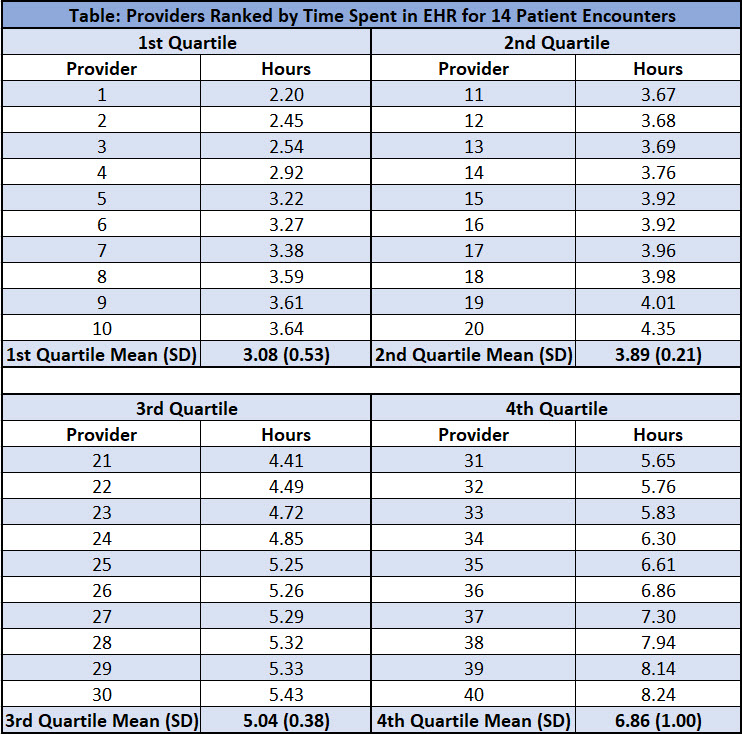
Results: 40 physicians in our group had data for the study period. On average, rounding physicians in our group spent 4.7 hours/day (SD 1.6hrs) to care for 14 patients. The mean time spent in the EHR by 4th quartile providers was 6.86 hours, 3.78 hours more than the 3.08 hours spent on average by the physicians in the top quartile (p<0.05) (Table). Improving the efficiency of the bottom three-quartile physicians to match that of the top quartile would result in a savings of 1.6hrs/physician/day. 5 of the 10 physicians in the 4th quartile had less than 1 year of experience as a hospitalist (p<0.05 v 1st quartile).
Conclusions: There is a large variance in time spent in the EHR, even when comparing providers in the same HM group working at a single hospital. For the 30 providers in the bottom 3 quartiles, 10,738 hours could be saved/year or nearly 5 FTE translating to $1.52 million annually, not including the cost savings of decreasing burnout. These data suggest resources should be invested to improve hospitalist EHR efficiency. Further studies are needed over longer time periods and comparing time in the EHR with quality metrics.