Background: Over 35 million people are hospitalized annually in the United States, many of whom experience decline in physical functioning due to insufficient physical mobility. The geriatric patient population is at the highest risk of impairment in their baseline activities of daily living (ADL), falls, frailty and prolonged disability from insufficient physical mobility. The geriatric hospitalist service at our large academic tertiary care hospital aimed to improve mobility in all patients on our medical surgical floor by ambulating a minimum of 100 feet distance at least once during their hospital stay from the baseline of 37% in February 2018 to 80% by November 2018. We launched a quality initiative process utilizing a smart EMR reporting tool to identify older adults (70 years and older) with risk factors for functional decline and poor outcomes. An interdisciplinary rounding model, vACE: Virtual Acute Care for Elders, was instituted with the goal to share meaningful information to improve mobility and care for patients.
Purpose: To describe the planning, implementation, monitoring, and initial data of vACE rounds at an academic tertiary care hospital to improve mobility during hospital stay.
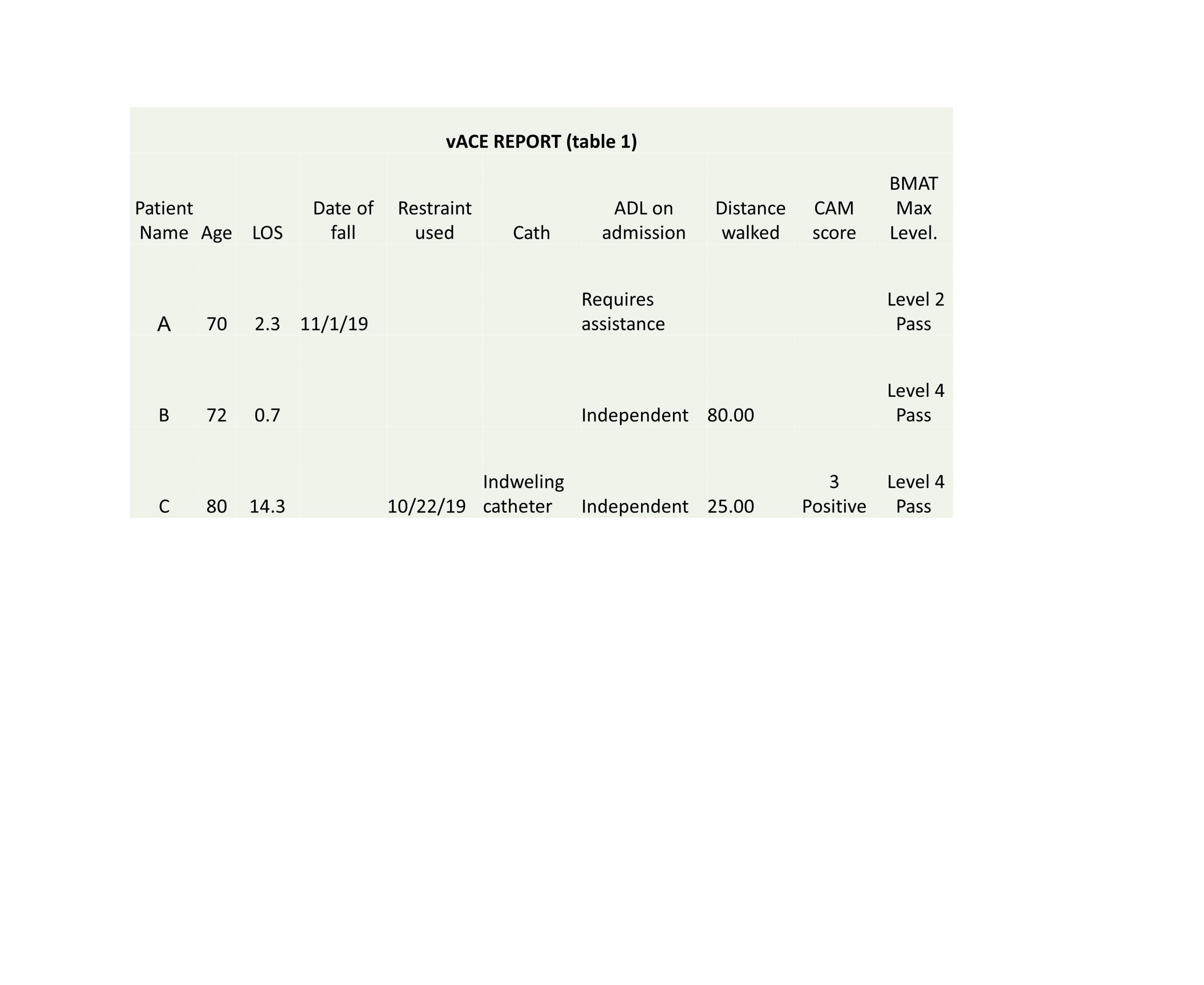
Description: vACE rounds include an interdisciplinary team approach comprising of a geriatrician, gerontology nurse practitioner, unit in-charge nurse, social worker and pharmacist. The team meets Monday through Thursday to conduct a 15-minute huddle on medical and surgical floors. A daily automated report is generated as a spreadsheet and it serves as a guide for discussion. The variables in the report include: age, length of stay, falls, physical restraints, urinary catheters, ADL on admission, Confusion Assessment Method score, Banner Mobility Assessment Tool (BMAT) level and distance ambulated in last 24 hours. For patients with BMAT level 3 or 4 the target is set to ambulate a minimum of 100 feet distance. For patients who are not ambulating with a BMAT level of 3 or 4, barriers are identified and efforts are made to overcome like removing urinary catheter or implementing delirium mitigation strategies. Nurse managers then discuss these measures with the floor nurses to encourage ambulation.
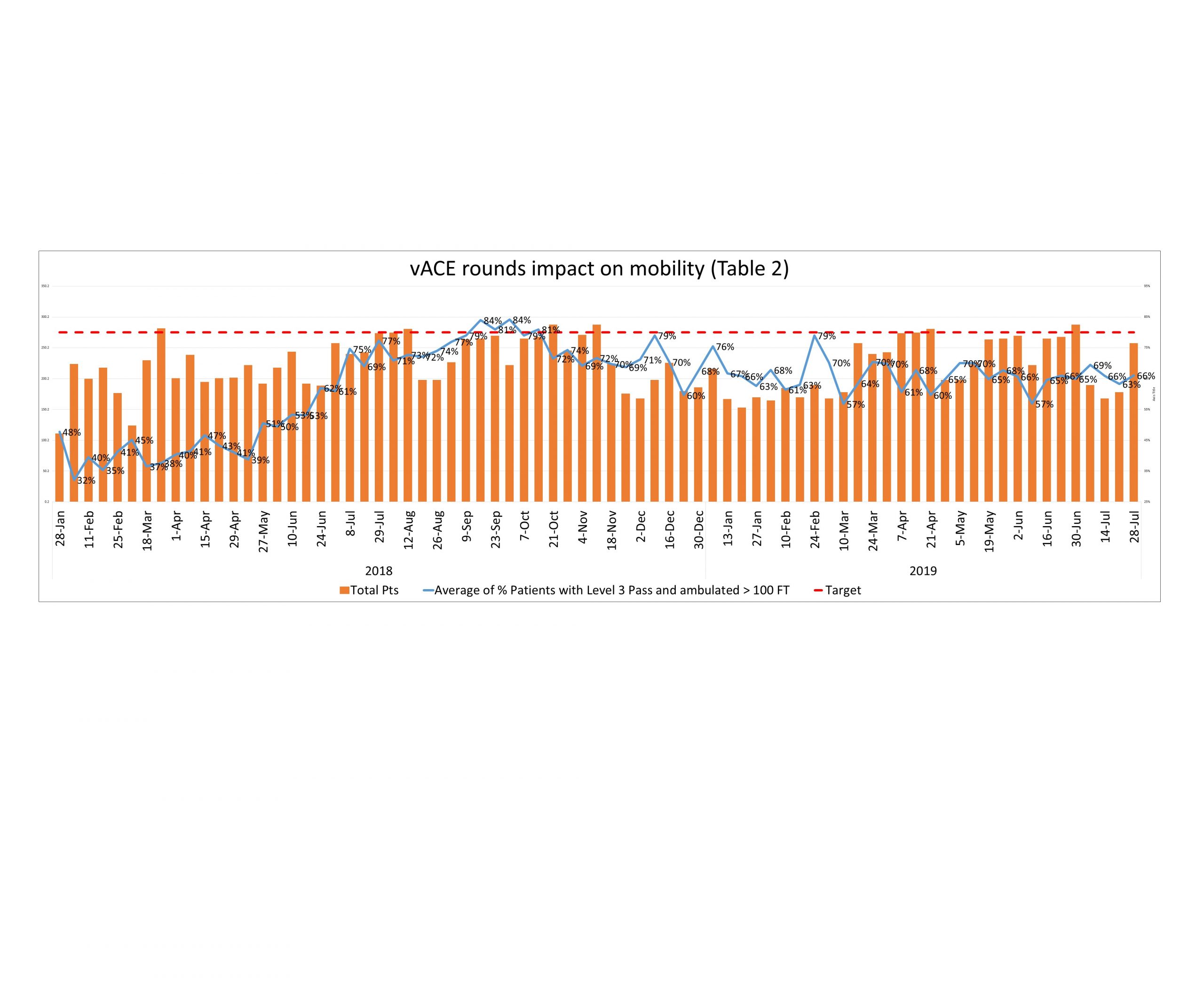
Conclusions: vACE rounds were initiated on March 01, 2018. A successful adoption of the new initiative was seen after winning nursing leadership support in May 2018. We met our benchmark of 80% patients with BMAT level 3 or 4 ambulating a minimum of 100 feet distance by September 2018. However, this trend was not sustained and dropped to 65%. This new baseline has since then been stable. Our interventions have made an improvement in mobility and care of all adult patients even though vACE rounds included only patients above the age of 70.This is a simple and innovative way of improving mobility in the hospitalized patients using a multimodal approach, smart use of current EMR technology and minimal utilization of resources.