Background: Many electronic health record (EHRs) systems offer secure messaging which allows for asynchronous, text message-based communication. Increasingly electronic messaging is replacing more traditional methods of communication such as paging, yet there is limited research on the impact of this transition. Studies have shown that healthcare workers find text communication to be more efficient than paging, but this is potentially offset by harms such as increased workload due to messaging volume, communication misunderstandings, and frequent interruptions which may increase risk of medical errors.This study characterizes the quantity and patterns of secure electronic messaging use at a single academic institution to better understand its impact on clinician workloads and work patterns. Additionally, we propose that secure messaging volume can serve as an efficient and innovative measure of work volume. This measure may offer deeper insight into provider workloads than traditional measures such as encounters and work relative value units (wRVUs) and can be used to evaluate the impact of work design interventions.
Methods: We conducted a retrospective observational study of Epic Secure Chat (ESC) use between April 1, 2023 to April 30, 2023 at a large academic hospital. ESC data was limited to chat messages sent and accessed by physicians and advanced practice providers (APPs) working on daytime hospital medicine teams. We analyzed the number of conversations per day, number of chats sent and accessed (read) per hour, and average time between when a chat was sent and accessed by the clinician (lag time). These values were plotted against patient volumes and time of day. Pearson Correlation Coefficients were used to analyze the relationship of the volume of secure chats and lag time with patient volumes.
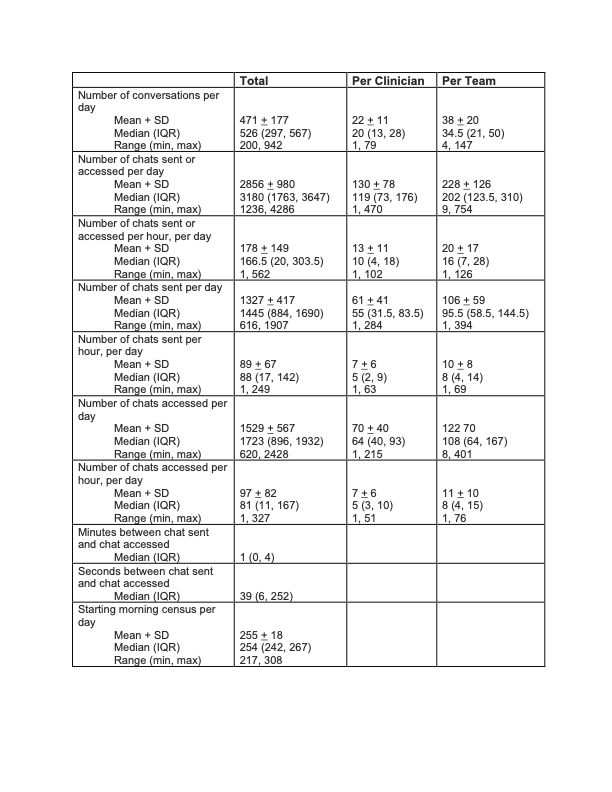
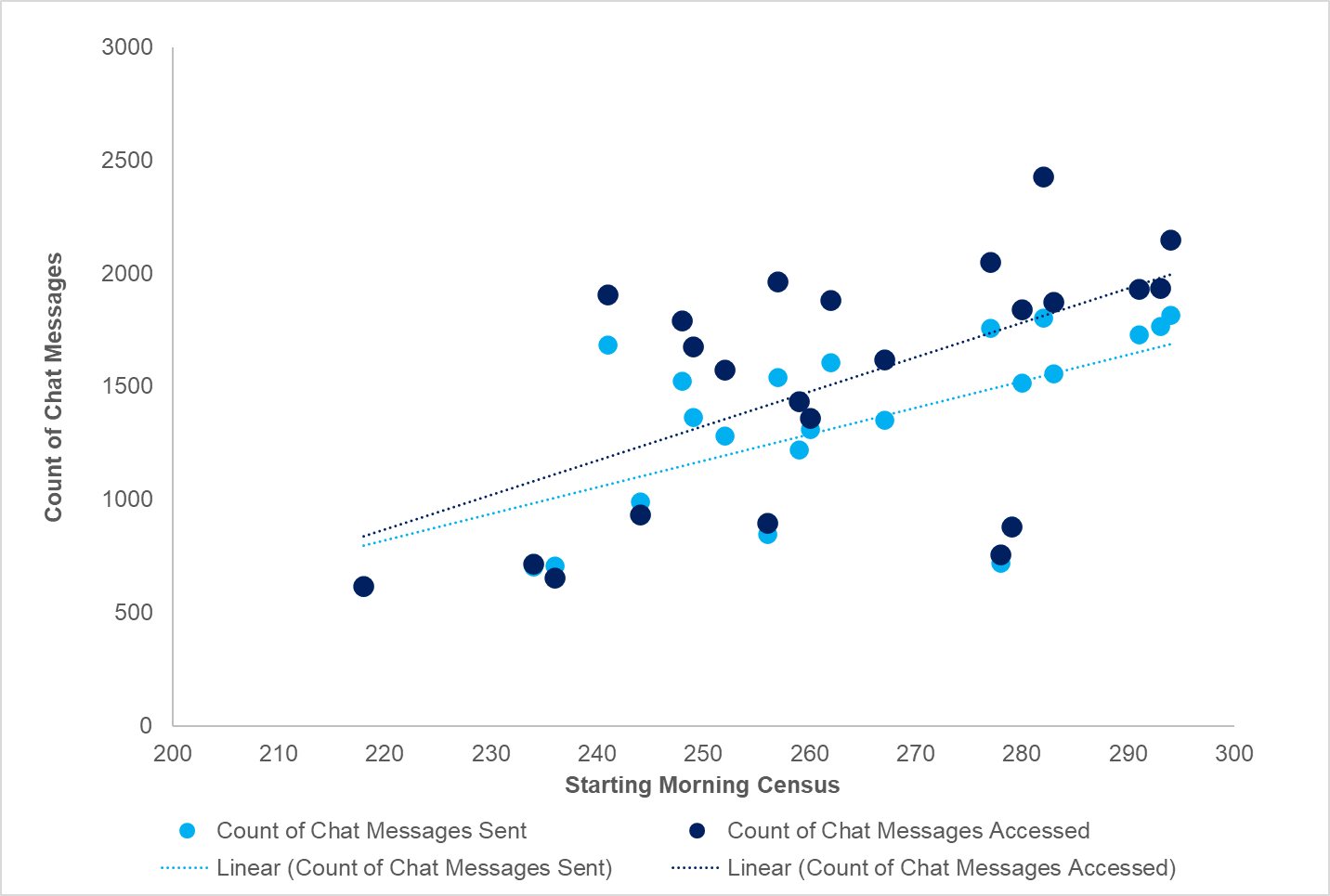
Results: A total of 46 physicians and 42 APPs worked on 14 teams during the 30 days of data collection. Clinicians sent or received an average of 130 (+/- 78) messages per day with an average of 7 (+/- 6) messages sent per hour and 7 (+/-6) received per hour. The median (IQR) time between a message being sent and accessed was 39 seconds (IQR: 6, 252) (Table 1). There was a statistically significant correlation (p< 0.01) between starting morning census and number of conversations per day, number of chats sent per hour, and number of chats accessed per hour, but census did not impact lag time (p= 0.0985) (Figure 1).
Conclusions: Clinicians in the inpatient setting are managing a large volume of messages that demand their time and attention. The lag time for reading these messages is relatively short, suggesting frequent interruptions to workflow which may impact clinical care and provider burnout. Message volume increases as patient volume rises, although there is a wide variation in message volumes. This study is one of the first to provide a more granular analysis of the patterns of electronic messaging use for inpatient clinicians, which may be useful in proactively measuring the impact of work design on work patterns.