Background: Alcohol Use Disorder (AUD) is prevalent among hospitalized Veterans and is associated with increased mortality.[1] AUD contributes to both morbidity and mortality through its direct physiological effects and its association with various medical, psychiatric, and social consequences. The World Health Organization estimates that alcohol use accounts for approximately 4.7% of all deaths in 2019 or roughly 2.6 million deaths.[2] Approximately 178,000 people in the U.S. die annually due to excessive alcohol consumption.[3] Our prior research indicates that an AUD diagnosis at admission correlates with a 33% five-year mortality risk.[1] Using the same cohort, this study examines the age at death and cause-specific mortality among Veterans admitted to Veterans Health Administration (VHA) hospitals, comparing those with and without AUD diagnoses.
Methods: We conducted a retrospective cross-sectional study of 1,151,815 Veterans admitted to 129 VHA hospitals between fiscal years 2016–2020. Mortality data through December 2022 were obtained from the National Death Index. The follow-up period varied based on the index admission date, with patients in the cohort experiencing a minimum of 2 years and a maximum of 8 years of follow-up, with a median of 5.4 years. AUD diagnoses were identified using ICD-10 codes. Statistical analyses included chi-square tests and odds ratios to assess differences in age at death and cause-specific mortality.
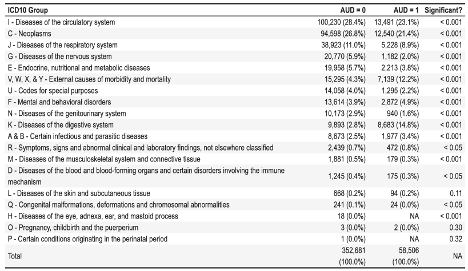
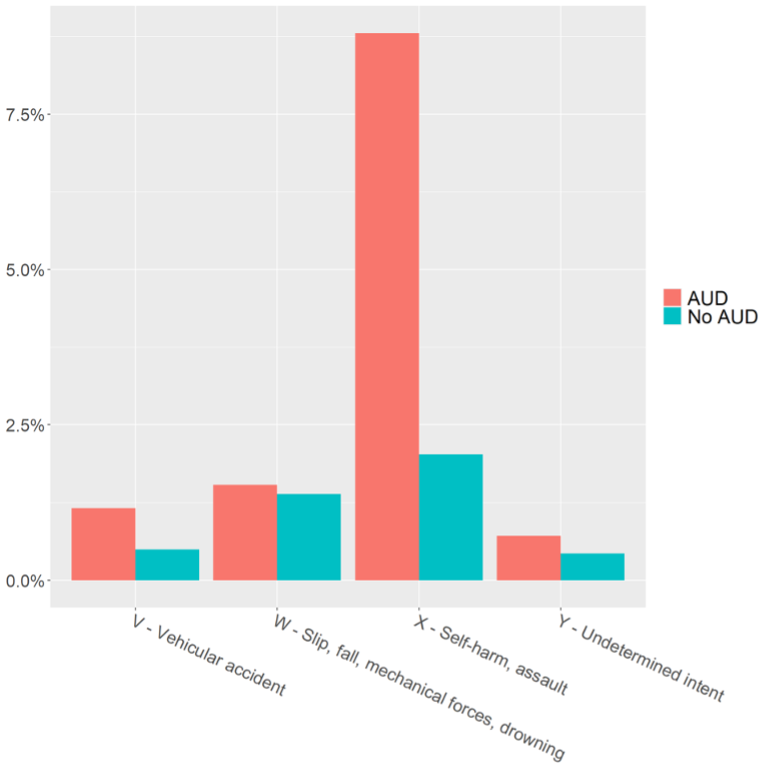
Results: Of 411,187 deaths, 58,506 (14.2%) occurred in patients with AUD diagnoses. Veterans with AUD died at a younger age (mean 62 years) compared to those without AUD (mean 72.7 years). AUD was strongly associated with mortality among younger Veterans (OR 2.43; 95% CI: 2.31–2.57 for ages 18–39). Compared to non-AUD patients, AUD patients had higher proportions of deaths from digestive diseases (14.8% vs. 2.8%) and external causes (12.2% vs. 4.3%), including suicide (8.8% vs. 2.0%; OR 2.91; 95% CI: 2.72–3.12). Deaths from circulatory diseases and neoplasms were less frequent in the AUD group.
Conclusions: Veterans with AUD diagnoses at admission experience premature mortality and are disproportionately affected by suicide and digestive disease-related deaths. These findings underscore the need for targeted interventions during hospitalization, including AUD screening, suicide prevention, and management of alcohol-related health risks.