Background: Medical teams may take care of patients on multiple units. Traditionally, alpha-numeric pagers have been the primary means for nurses to contact resident physicians off geographic units. However, mobile devices are increasingly being used and there are few studies that have analyzed their effectiveness as a means of communication compared to pagers.
Purpose: The purpose of the study was to understand current challenges to effective nurse-resident communication and to assess the impact of replacing pagers with cellphones on nurse-resident communication.
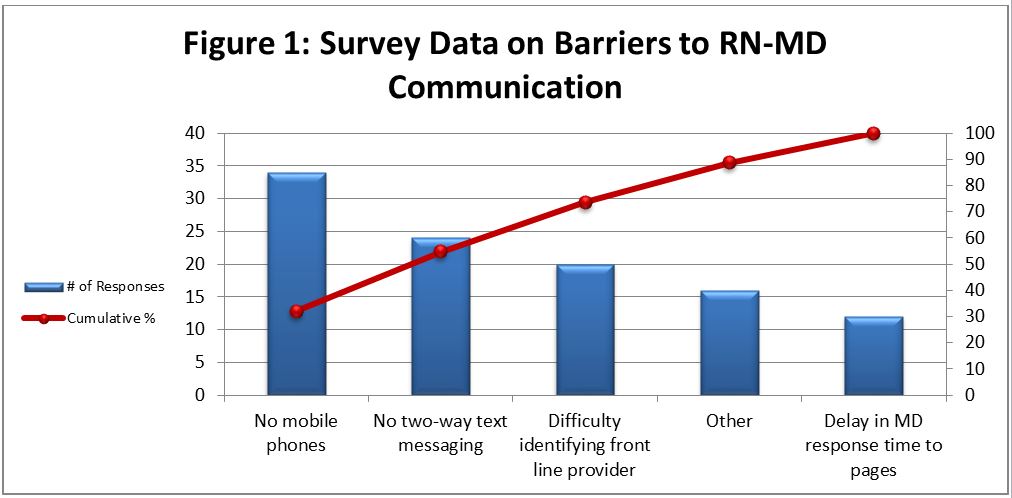
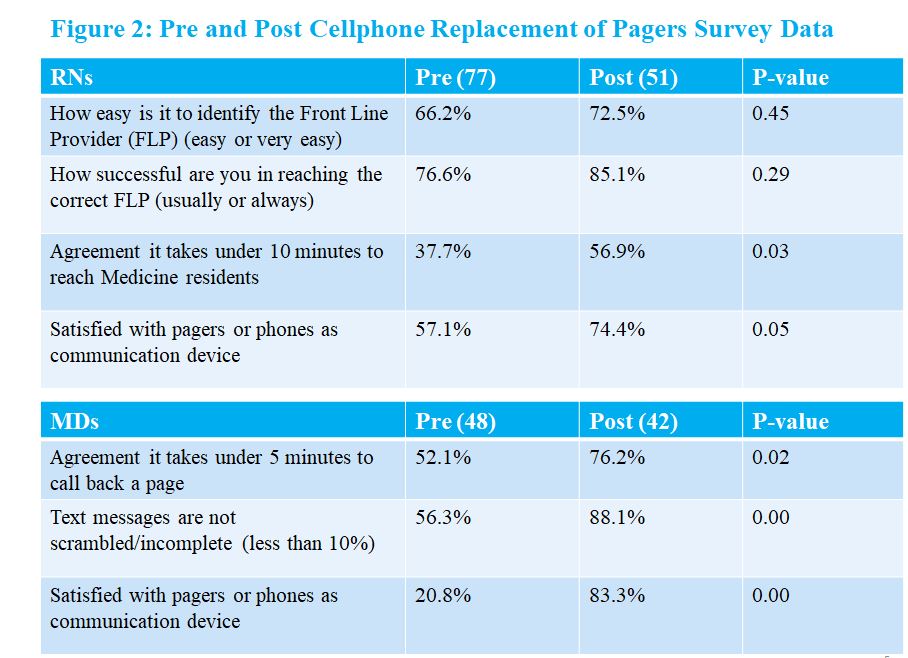
Description: This quality improvement initiative was conducted at a large urban academic hospital. Residents had one-way pagers that were able to receive notifications via telephone paging or alpha-numeric messages via webpage. Prior to the replacement of pagers, an anonymous survey was administered to Internal Medicine residents and to nurses to understand communication challenges and to elicit suggestions for improvement. There were 77 nurse and 48 resident respondents. Themes that emerged from the survey included needing mobile devices for direct communication and the adoption of two-way messaging (fig. 1). After survey data were collected, resident pagers were replaced with cellphones; nurses were not provided cellphones. Similar to the paging system, nurses were able to send text messages to residents via webpage, though residents were unable to send responding texts. For urgent questions or updates, nurses were encouraged to call rather text. Anonymous surveys were collected for both nurses and residents before and after cellphones replaced pagers as a communication device. Both nurses and residents perceived faster response times and were more satisfied with cellphones over pagers (fig. 2). Analysis of only Medical-Surgical floor units indicated that overall satisfaction with device communication rose from 69.64% to 88.46% (P=0.017) after phone implementation, and 23.81% to 64.29% (P=0.017) in the ED.In addition to the survey data, nurses were asked to track resident response times to pages both before and after the implementation of cellphones. Interestingly, a comparison of average resident response times (in minutes) before and after replacing pagers with cellphones showed no statistical significance across all categories of pages, or with overall combined page response time (8.0 vs 10.7, p=0.26).
Conclusions: Based on survey data, we found that there was significant interest in using phones and texting as forms of communication between nurses and residents. The replacement of resident pagers with cellphones resulted in the perception from nurses and residents that both providers of the care team are more accessible to each other. Interestingly, cellphones did not seem to improve average resident response times to pages. This finding likely reflects “texting” culture for non-urgent communication. For urgent issues, nurses had the ability to call residents directly, however, for non-urgent issues nurses still had to wait for residents to call back to texts. HIPAA-compliant texting applications are now available both via phone and the electronic medical record, and further study is needed to see if providing two-way texting between nurses and residents would improve response times.