Background: Large-scale sustained medical surges (like the COVID-19 pandemic) can exceed existing hospital capacity and can result in activation of Alternate Care Facilities (ACFs). Traditional ACFs have repeatedly demonstrated limitations including inadequate privacy, HVAC control, infection prevention challenges, lack of integrated clinical systems, and poor patient and staff experience. With grant funding from the Defense Health Agency (DHA) and in conjunction with the National Disaster Medical System (NDMS) pilot, we sought a scalable, rapidly deployable, and patient-centered alternative: converting a hotel into a hospital. Hotels have intrinsic advantages: private rooms, bathrooms, temperature control, food service, laundry, and established infrastructure. They have been used for ACFs previously but usually only for limited medical care. Few have ever been fully converted to provide full med-surg and ICU hospital care.
Purpose: To develop and validate the Hotel-to-Hospital (H2H) conversion playbook (https://www.hotel2hospital.info/uploads/7/4/3/6/74368907/_h2h_guidebook_digital_2025.10.17_reduced.pdf) to provide full hospital-level care within 4 weeks.
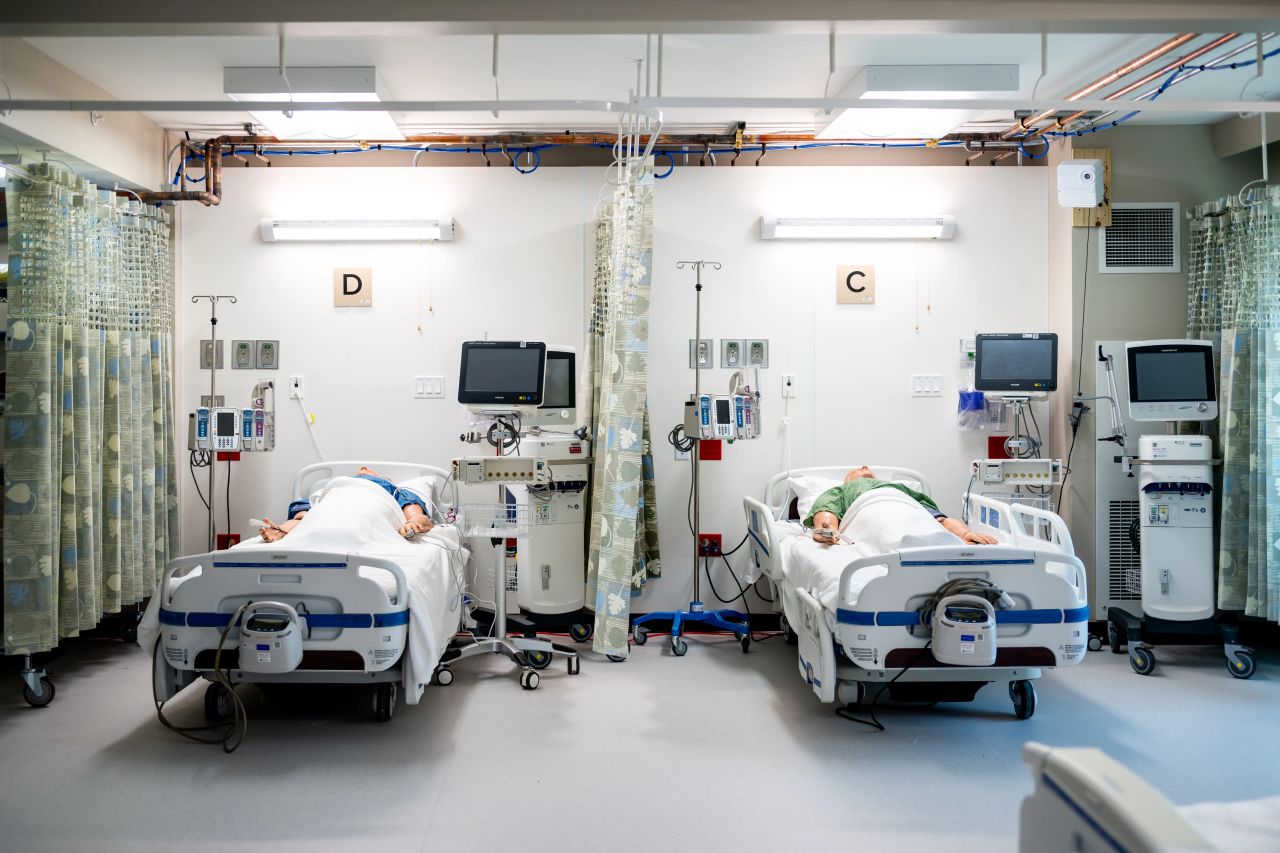
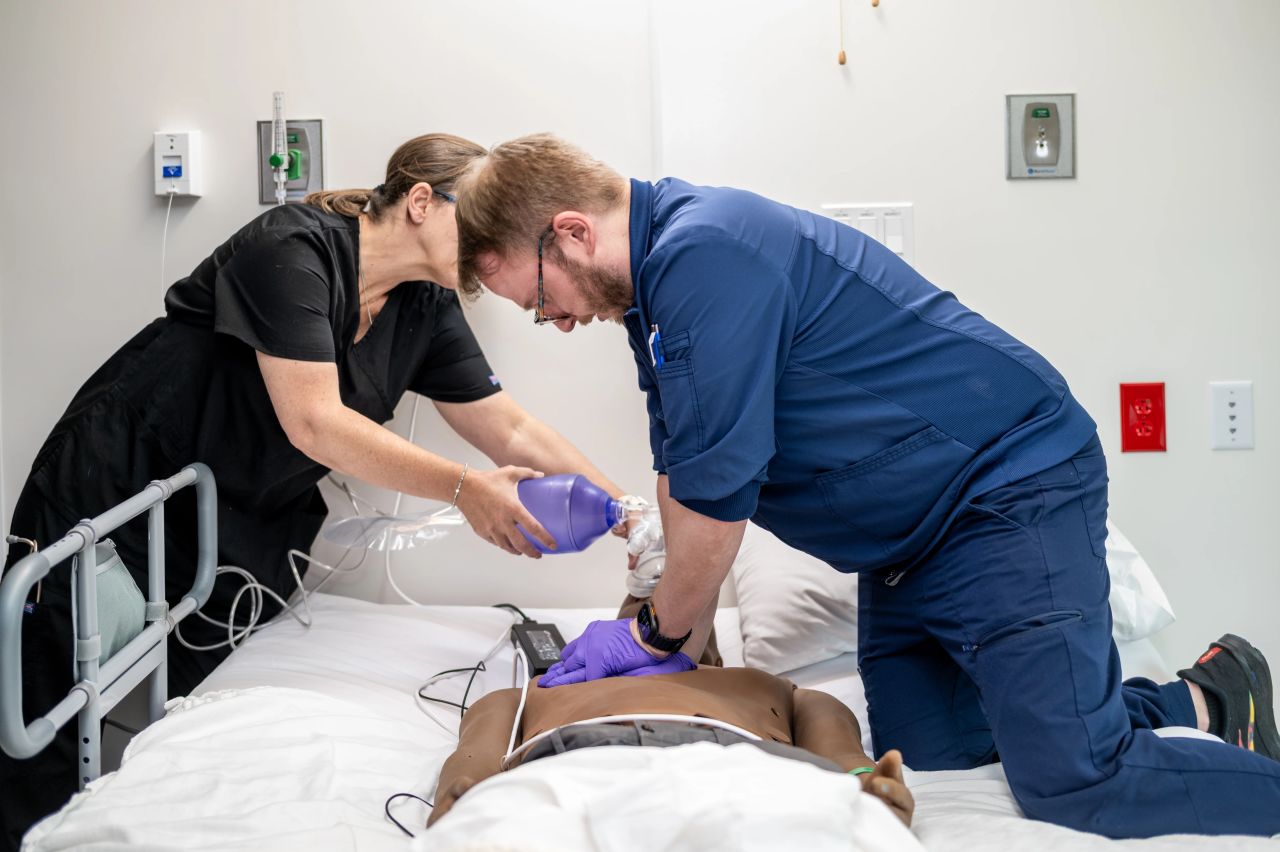
Description: A multidisciplinary team, including experts from emergency management and hospital operations as well as architects, engineers, IT, clinical departments, response partners, and hotel leadership, embarked on a three-year research project to prove a hotel could be a viable solution for an ACF. We converted portions of a hotel into a hospital fully integrated with our hospital’s electronic medical record, supply chain, pharmacy, lab, radiology, respiratory therapy, and infection prevention to operate as a remote “wing” of the managing hospital. Conversion activities included architectural design; creating ICU and med-surg capabilities in hotel rooms and conference rooms; simulating oxygen delivery systems and emergency power; adapting hotel rooms for nurses’ stations, pharmacy, laboratory, and diagnostic imaging. Existing hotel services such as food service, laundry, housekeeping, wayfinding, and maintenance were incorporated to support healthcare operations. The team validated patient flow, admissions, medication management, specimen handling, radiology workflows, telehealth, emergency response, and end-to-end documentation through a “Day in the Life” activities with frontline clinicians.Lessons learned include validating standard patient care in repurposed hotel beds (including CPR quality equivalent to hospital beds); rapid conversion of hotel spaces into single and double occupancy med-surg rooms with integrated headwalls; full integration with IT services including remote telemetry and features such as 5-digit calling; a production build of Epic™ with full feature PACS, EKG, and lab capabilities; establishing point-of-care lab services; and on-site Pyxis™ mediation dispensing from the pharmacy.
Conclusions: The H2H is a viable solution for expanding staffed bed capacity without building new facilities. A hotel can be converted into a functional, hospital-integrated ACF in less than 4 weeks and is capable of safe, patient-centered care during prolonged medical surges. Existing hotel infrastructure and services significantly reduce construction needs, improve patient experience, and support hospital operations. The H2H model represents a reproducible, scalable, and resource-efficient strategy for medical surge planning.