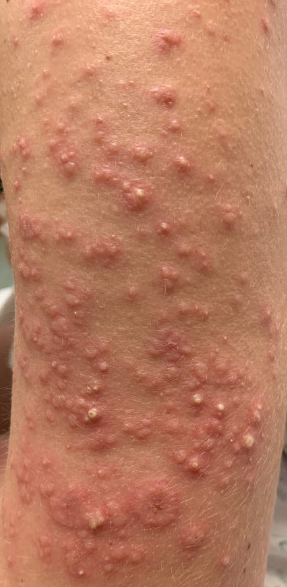
Case Presentation: A 32-year-old female presented to the hospital with a complaint of progressively worsening rash. About 3 days prior to the rash, she had experienced fevers, chills, and malaise. Physical exam was notable for erythematous papules on the forehead, arms, and chest. Blood tests were pertinent for mild leukopenia and anemia, elevated inflammatory markers ESR 67 and CRP 46. Pertinent negative labs included HIV, Hepatitis, and beta-hCG. She denied any medications in the past few months apart from Tylenol. Dermatology was consulted and punch biopsies were performed. Pathology resulted as neutrophilic dermal infiltrate, leukocytoclasia, perivascular acute inflammation, and rare eosinophils. She was started on treatment with prednisone for a total of 6 weeks. On follow-up at 3 weeks into treatment, there was significant improvement in the rash and no new lesions seen.
Discussion: Sweet syndrome or acute febrile neutrophilic dermatosis is a rare inflammatory skin condition caused by a sudden onset of fever and painful rash on the arms, legs, trunk, face or neck. The rash consists of multiple edematous, painful, and erythematous papules, plaques, or nodules that grow rapidly in size, developing into clusters up to approximately an inch in diameter. There can also be extracutaneous involvement, most commonly ocular and musculoskeletal. Sweet syndrome can occur as a reaction to a medication, most commonly granulocyte-colony stimulating factor and all-trans retinoic acid. It is associated with malignancy in approximately 21% of patients; 15% have hematological disease (AML) and 6% have solid tumors, most commonly GU or GI cancer. More than 71% of cases, present as classical or idiopathic Sweet syndrome and within this category, 80% are female and had a prior URI or GI infection. Recurrence occurs in about a third of patients with the classical variant, but is most likely to occur in patients with malignancy-associated disease. Recurrence occurs in about 69% of heme malignancy cases and about 41% of solid tumor cases.
Conclusions: Sweet syndrome is uncommon, and the cause of most cases is unknown; however, there are certain risk factors that can increase one’s risk. These include female gender, adults between the ages of 30 and 60, cancer, inflammatory bowel disease, pregnancy, drug sensitivity, and recent upper respiratory infection. The diagnosis of Sweet syndrome is established when the following major criteria and 2 of the minor criteria are met. Major criteria include abrupt onset of rash and histopathologic evidence of a dense neutrophilic infiltrate without evidence of leukocytoclastic vasculitis. Minor criteria include temperature >38°C, history of associated illness or malignancy, good response to corticosteroid or potassium iodide, and leukocytosis with neutrophilia, ESR > 20, positive CRP. Sweet syndrome is commonly treated with corticosteroids pills, such as prednisone. For patient’s unable to tolerate long-term corticosteroid use, alternative first-line therapies include dapsone, potassium iodide, and colchicine. Signs and symptoms often resolve just a few days after the initiation of treatment. This syndrome can be managed on an outpatient basis, but the signs and symptoms are often concerning for serious infection which leads to hospitalization. It is important to recognize this common presentation of Sweet syndrome to prevent unnecessary testing and treatment.