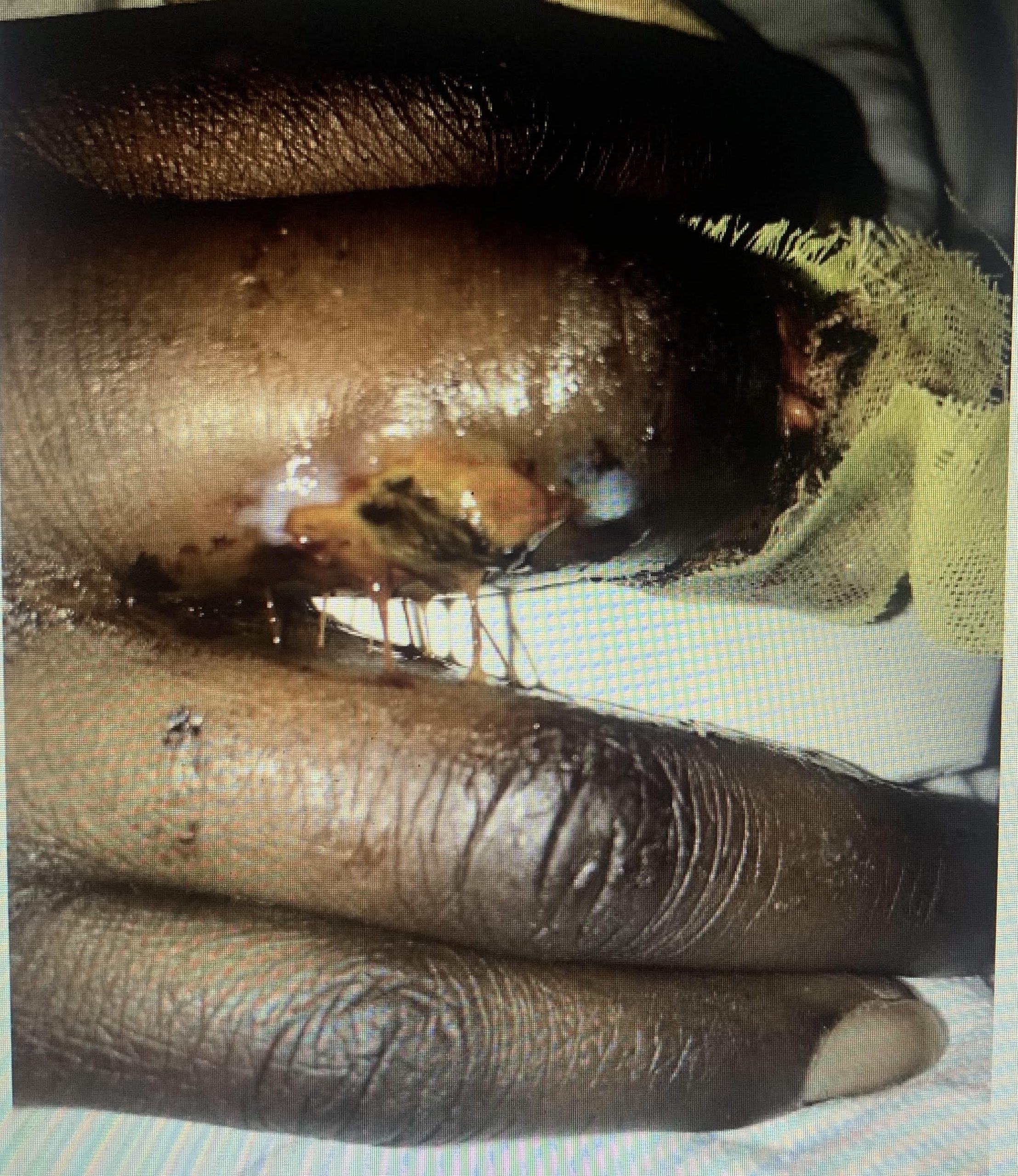
Case Presentation: A 30 year old woman with a history of alcoholic cirrhosis, episodes of alcoholic hepatitis and pancreatitis, was transferred to a tertiary care hospital from a community hospital for a liver transplant evaluation. On admission, she had a MELD score of 33. The patient was not a candidate for liver transplant due to active alcohol use, and was started on prednisolone for her alcoholic hepatitis as her MDF was 108. On day 4 of her hospitalization, she began to experience pain in her right middle finger out of proportion to exam findings. On day 10, she was noted to have blisters on the PIP of the right middle finger, for which plastic surgery was consulted, and the patient was started on Bactrim for presumed cellulitis. Wound cultures grew Enterococcus faecium, so was transitioned to IV vancomycin. She then developed bogginess in her right middle finger with uptrending leukocytosis. On hospital day 18, the patient developed a new lesion on her left forearm, described as a subcutaneous nodule with an overlying necrotic eschar. Additionally, the erosions on the patient’s right middle finger had scabbed over into black eschars as well. Pathology from biopsy completed on hospital day 19 showed filamentous fungus, consistent with Rhizopus species. She was diagnosed with Mucormycosis, started on liposomal amphotericin B. CT scan of the patient’s chest showed concern for pulmonary dissemination of her disease. Her right middle finger was amputated on hospital day 22 and she had repeated debridement of her lesions with plastic surgery. Despite aggressive medical management, the patient developed deteriorating kidney function and worsening mental status. She was transitioned to comfort care on hospital day 31 and expired shortly after.
Discussion: Mucormycosis is a rare opportunistic nosocomial infection in hospitalized patients, with manifestations including rhino-orbital, pulmonary, GI, cutaneous and disseminated disease. Cutaneous mucormycosis has been described in several case reports of patients with severe alcoholic hepatitis and cirrhosis. Initiation of corticosteroids in patients with severe alcoholic hepatitis is not associated with increased rates of bacterial infections, but steroid use is associated with increased incidence of opportunistic fungal infections like Mucormycosis. Several studies report that rates of mucormycosis are rising among hospitalized patients as usage of immunosuppressive therapy increases. Cutaneous mucormycosis can occur in hospital settings due to direct inoculation via IV punctures, contaminated wound dressings, and areas of skin breakdown. Making the diagnosis of cutaneous mucormycosis can be difficult, as histopathological specimens are required for identification of Rhizopus species. However, early diagnosis and treatment with aggressive debridement as well as liposomal amphotericin B are necessary to reduce mortality in these patients.
Conclusions: In cases of cutaneous infections refractory to broad spectrum antibiotics, Mucormycosis should be considered. If index of suspicion for Mucormycosis is high, hospitalists should be encouraged to seek consults to obtain skin biopsy for tissue diagnosis to facilitate early initiation of antifungal treatment and aggressive debridement.