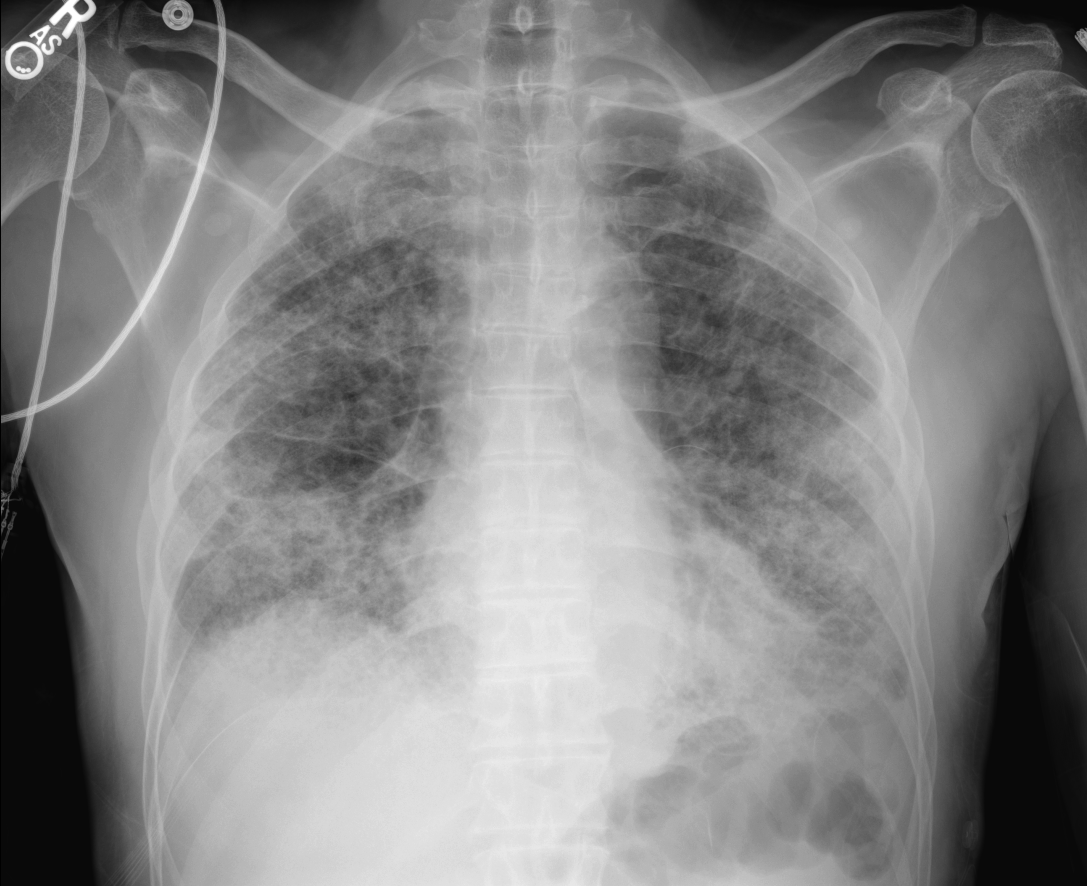
Case Presentation: A 71-year-old African American male presented to the emergency department due to chest pain, fevers and shortness of breath with associated dry cough. The symptoms progressively worsened since onset one month prior to admission. He was HIV negative with a history of Stage IV (T2a N2 M1a) lung adenocarcinoma diagnosed one year ago by diagnostic thoracentesis, and treated with maintenance chemotherapy given 6 cycles of Pemetrexed-Pembrolizumab. Vital signs were significant for low oxygen saturation near 80% on room air and a 102.7 °F temperature, with bilateral coarse breath sounds on lung exam. Chest x-ray (CXR) and CT chest indicated diffuse bilateral infiltrates.
The patient was admitted to the general medical floor and treated with Ceftriaxone and Azithromycin for suspected community-acquired pneumonia (CAP). He continued to spike fevers along with increased oxygen requirements prompting transfer to the ICU to be placed on high flow oxygen (AIRVO). The differential was broad and included Pneumocystis Jiroveci Pneumonia (PJP), Interstitial Pneumonitis, and CAP. He was started on Methylprednisolone, Trimethoprim-Sulfamethoxazole (TMP-SMX), Piperacillin-Tazobactam, and Levofloxacin. Due to tachypnea and desaturation despite being on AIRVO, along with the worsening infiltrates on CXR, he was intubated.
Low tidal volume and high PEEP ventilator settings were used due to suspicion of Acute Respiratory Distress Syndrome. Bronchoscopy was unremarkable and bronchoalveolar lavage (BAL) analysis was sent. Only steroids and TMP-SMX were continued as the Pneumocystis PCR (BAL) returned positive. He was later switched to Clindamycin and Primaquine due to hyperkalemia. Antibiotics were continued for 21 days and steroids for 28 days. He was then transitioned to a tracheostomy with decreased ventilator requirements during the hospitalization.
Discussion: PJP is a life-threatening condition predominantly occurring in immunocompromised individuals. There was an increase in cases during the HIV epidemic in the 1980s that are now reduced due to routine prophylaxis. PJP continues to be a significant cause of severe pneumonia in patients with other types of immunodeficiencies.
Anti-PD1 immunotherapy like Pembrolizumab use host immune response targeting cancer cells and have been reported to cause pneumonitis. On the other hand immune compromise occurs in chemotherapy with Pemetrexed, an antifolate therapy. Although very rare, there are a few reported cases linking PJP in patients receiving regimens containing Pemetrexed, which further bolsters the need to consider this therapy as a potential risk factor for PJP.
CAP is often suspected in patients presenting with cough, fever, and shortness of breath, but PJP pneumonia is not typically included in the differential diagnosis, which may delay diagnosis. Index of wariness should be high in immunocompromised patients and empiric treatment must be considered.
Conclusions: This case illustrates the importance of recognizing PJP as a rare cause of pneumonia in patients with malignancies undergoing treatment with Pemetrexed and Pembrolizumab. Clinicians ought to consider PJP when patients undergoing this treatment are admitted with signs and symptoms of pneumonia.