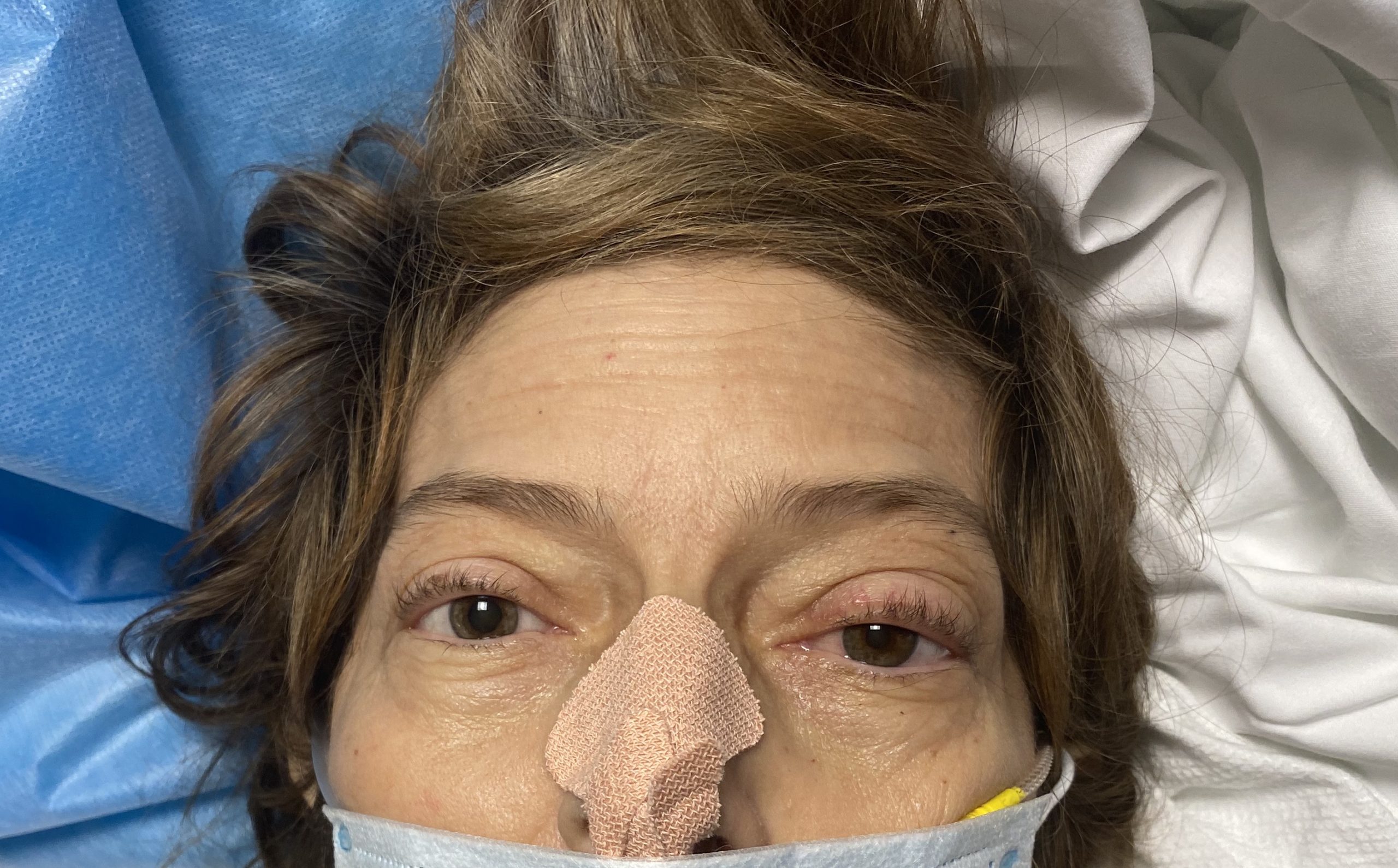
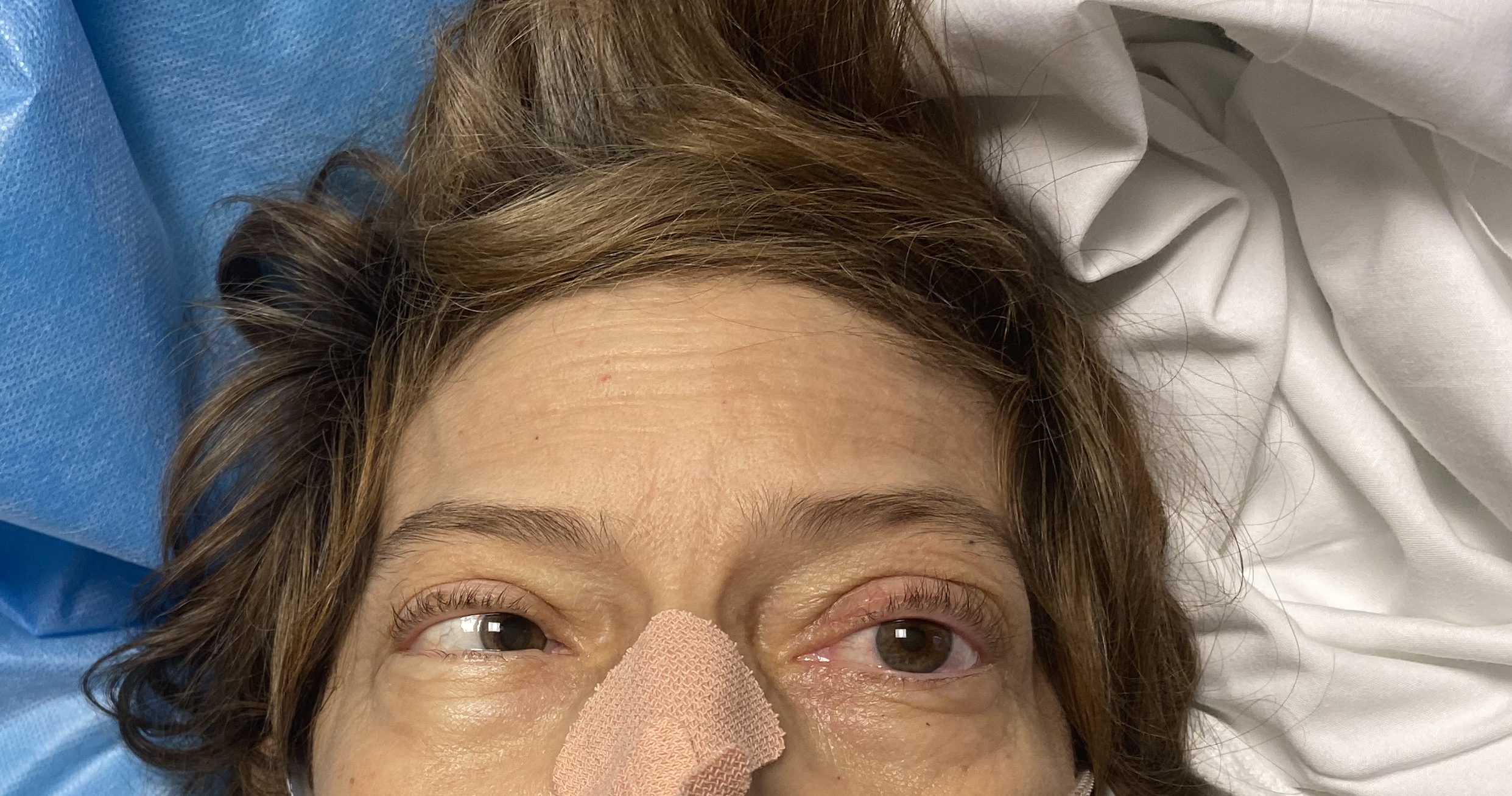
Case Presentation: A 61-year-old female with a history of non-alcoholic steatohepatitis (NASH) cirrhosis complicated by hepatocellular carcinoma (HCC), who underwent a liver transplant 2 months prior, presented to an outpatient clinic complaining of several days of fatigue, headache, nausea, vomiting, abdominal pain and confusion. Her headaches were new since the transplant. She denied any fevers, chills, but did endorse that her daughter had tested positive for COVID, so she was sent to the ED for further evaluation. On examination, she was afebrile and found to have nuchal rigidity. She was only oriented to person and place. Neurologic exam further revealed a left cranial nerve VI palsy with bilateral papilledema. Laboratory workup was pertinent for a normal WBC count, normal liver function tests, hyponatremia, hypokalemia, and hypomagnesemia. CSF studies revealed an opening pressure of 42cmH2O, normal glucose, mildly elevated protein, and neutrophilic pleocytosis. PCR on the fluid was positive for Cryptococcus neoformans and the patient was started on Amphotericin B and Flucytosine. Her hospital course was complicated by refractory elevated intracranial pressure requiring external ventricular drain placement and subsequent ventriculoperitoneal (VP) shunt placement. She still remains in the hospital with a guarded prognosis
Discussion: Cryptococcus neoformans is an invasive fungus known to cause acute to subacute meningitis in immunocompromised patients. HIV and AIDS are acknowledged as the most common risk factors for the development of disseminated infection. However, since the advent of ART, cases secondary to HIV are declining and alternative etiologies, including solid organ transplantation (SOT) are becoming widely recognized [1-2]. One study showed that SOT recipients have an incidence of cryptococcal infection of 0.2% during the first year of transplant, and up to 1 to 2% afterwards [3]. Cryptococcal infection is usually a late post-transplantation complication with a median time to diagnosis around 20 months [3], however, our patient presented around 2 months after SOT, raising concern for unrecognized pre-transplant or donor-derived infection, which generally presents sooner, within the first 30 days [4].Hydrocephalus is a well-known complication of cryptococcal meningitis, occurring in 9-63% of the patients, depending on the cohort [5]. The neurological manifestations can include papilledema and cranial nerve involvement, which is limited to the optic (CN II) and abducens (CN VI) nerves, most commonly the latter, due to its close proximity to the fourth ventricle upon entry to the subarachnoid space [5-6], and can be unilateral or bilateral. Although the mechanism of CSF flow obstruction remains unclear, patients with chronic (pre-transplant) infection, can develop hydrocephalus that does not respond to antifungal treatment and warrants VP shunt placement [7].
Conclusions: SOT recipients presenting with altered mental status should undergo early invasive testing to rule out life threatening conditions with potential neurological sequelae. These patients may have chronic conditions worsened by immunosuppression or newly acquired infections, so a broad differential should be kept in mind when evaluating these patients.