Background: The characteristic profiles of lesbian, gay, bisexual, transgender and queer or questioning (LGBTQ) individuals with heart failure are scarce in the literature. This investigation analyzes the demographics of LGBTQ individuals with heart failure and appropriateness of medical therapy.
Methods: A multi-center retrospective analysis of LGBTQ individuals with a diagnosis of heart failure was conducted within the MedStar health network. Patients over the age of 18 years hospitalized with International Classification of Diseases, Ninth and Tenth Revision (ICD-9 and ICD-10) codes for transsexualism and gender identity disorder from December 2000 to January 2017 were included in the study. Cross-reference with ICD-9 and ICD-10 codes for heart failure with reduced ejection fraction (HFrEF) and heart failure with preserved ejection fraction (HFpEF) was performed. Our search identified 104 patients, of which 16 had an established diagnosis of heart failure.
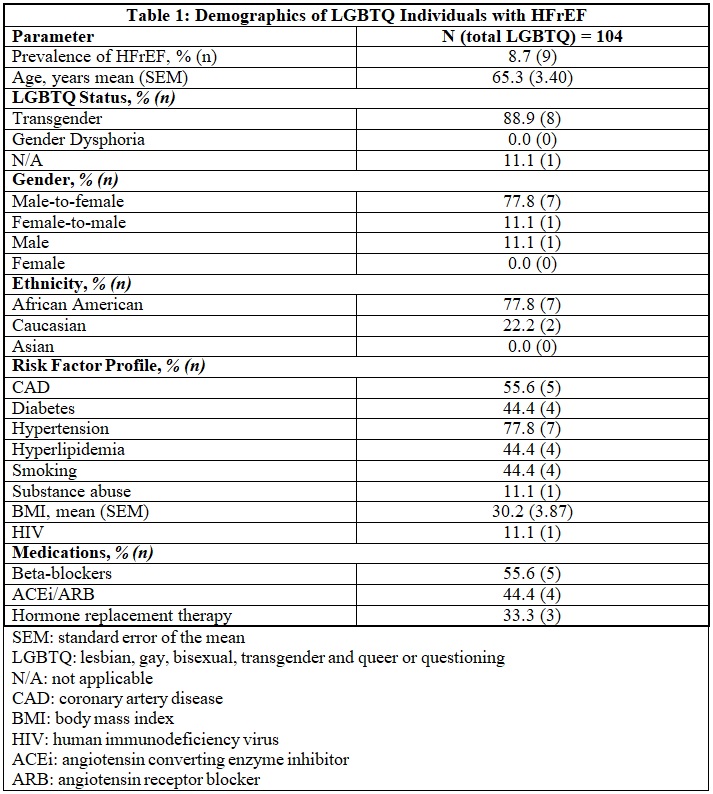
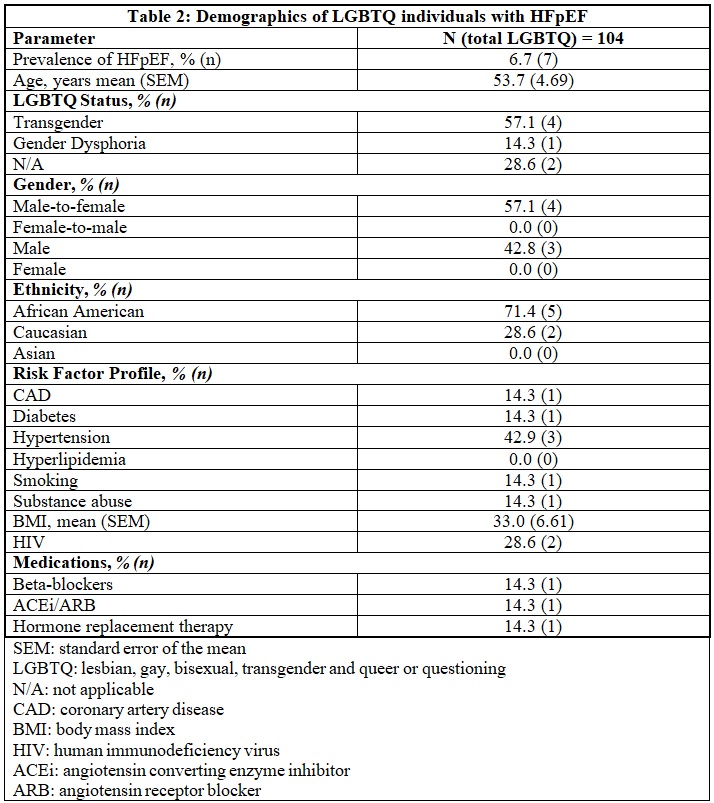
Results: The total number of patients with HFrEF was 9 with a mean age of 65.3 years (standard error of the mean (SEM) of 3.40). The most common gender status among individuals with HFrEF was male-to-female transgender (77.8%). Out of 9 patients, 7 (77.8%) were African-American and two (22.2%) were Caucasian (Table 1). Coronary artery disease was the most common risk factor (55.6%) in this subgroup. Regarding guideline directed medical therapy; only 55.6% were on beta-blocker therapy while 44.4% were receiving angiotensin receptor inhibitors or angiotensin receptor blockers. Regarding HFpEF, the total number of patients was 7 with a mean age of 53.7 years (SEM of 4.69). Out of 7 patients, 5 (71.4%) were African-American and two (28.6%) were Caucasian (Table 2). Hypertension was the most common risk factor in this subgroup (42.9%).
Conclusions: Our investigation is the first US-based analysis studying demographics of LGBTQ individuals with heart failure. African-American male-to-female transgenders were the most common subgroup. Half of LGBTQ individuals with HFrEF are on guideline directed medical therapy. More prospective cohort studies are needed to investigate medication adherence and drivers of failure to provide appropriate medical therapy.