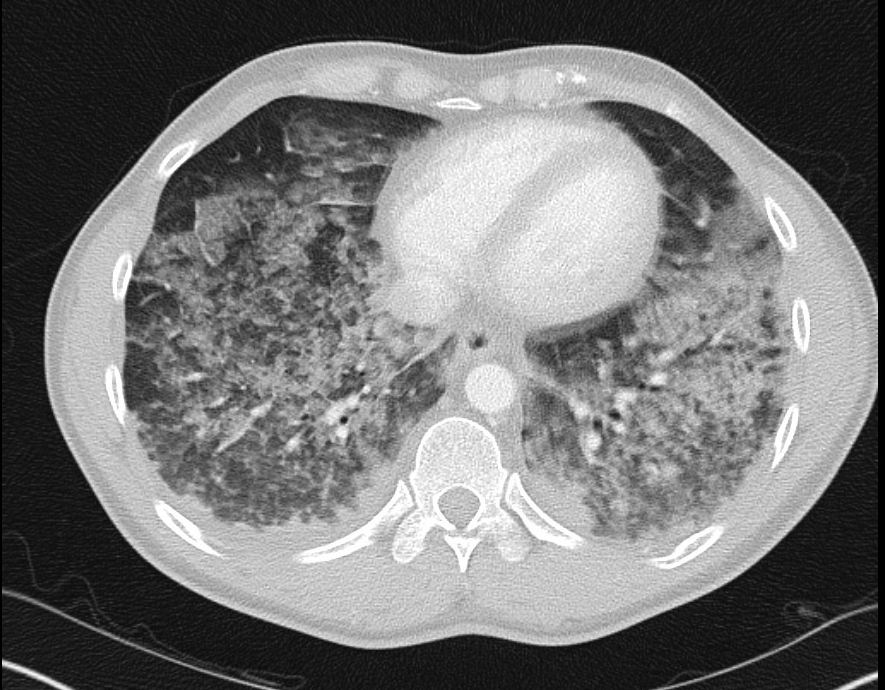
Case Presentation: A 40-year-old Bosnian male presented with five days of subjective fevers and dry cough associated with dyspnea. Patient stated he started smoking cigarettes again 10 days prior to admission after quitting for 7 years. Chest imaging demonstrated diffuse bilateral ground glass opacities and consolidations concerning for acute infection. Serologic workup was significant for peripheral eosinophilia after initially being negative and negative for beta-d-glucan, IgG to Stronglyoides, Aspergillus galactomannan antigen, Blastomyces antibody, Cryptococcus antigen, Histoplasma antigen, HIV, and ANCA. Patient was initially treated for community acquired pneumonia with antibiotics. On day 4, the patient’s respiratory status continued to decline. Chest x-ray showed acute worsening of bilateral airspace opacities, and he required 100% non-rebreather mask to maintain oxygen saturations greater than 90%. Patient was transferred to the medical ICU and was subsequently intubated. Flexible bronchoscopy for bronchoalveolar lavage was performed. P/F ratio and chest imaging findings were consistent with severe ARDS, so neuromuscular blockade was initiated. Bronchoalveolar lavage revealed 28% eosinophils and was negative for ova and parasites, respiratory pathogen panel, gram stain, fungal stain and AFB smear. There was a strong concern for acute eosinophilic pneumonia (AEP) but given patient’s history of residing in a refugee camp prior to entering the US, work up for a parasitic infection was done. Strongyloides was of concern due to the severity of hyperinfection syndrome in the setting of steroids; therefore, infectious disease recommended empiric treatment with ivermectin for two days. Methylprednisolone was started after the first day of ivermectin treatment. Patient had improvement in respiratory status within the first 24 hours of steroid initiation and was successfully extubated the following day. He continued to improve and was transitioned to prednisone 40 mg daily prior to discharge home.
Discussion: Acute eosinophilic pneumonia is an acute febrile illness with severe hypoxemia, diffuse pulmonary infiltrates, BAL showing eosinophilia >25%, and no evidence of infection, drug ingestion, asthma or atopic disease. Parasitic infections can present with peripheral eosinophilia but this is uncommon to see initially in AEP. AEP is a diagnosis of exclusion and other causes of pulmonary eosinophilia must be ruled out. The etiology of AEP can be idiopathic but identifiable causes include recent onset of cigarette smoking (either first time or restarting) or heavy inhalational exposure to smoke, passive smoking, fine sand, and dust. Compared to drug or idiopathic AEP, smoking AEP has been characterized by more severe disease manifestations and patients are more likely to be hospitalized. AEP has a good prognosis if treated early and relapse is uncommon.
Conclusions: Physicians should keep AEP in their differential for smokers with recent alterations in smoking habits who present with suspected pneumonia but fail to respond to antibiotics. Furthermore, the chronic complications of cigarette smoking are often discussed but it is equally as important to inform patients of the acute, potentially life threatening, complications as well.