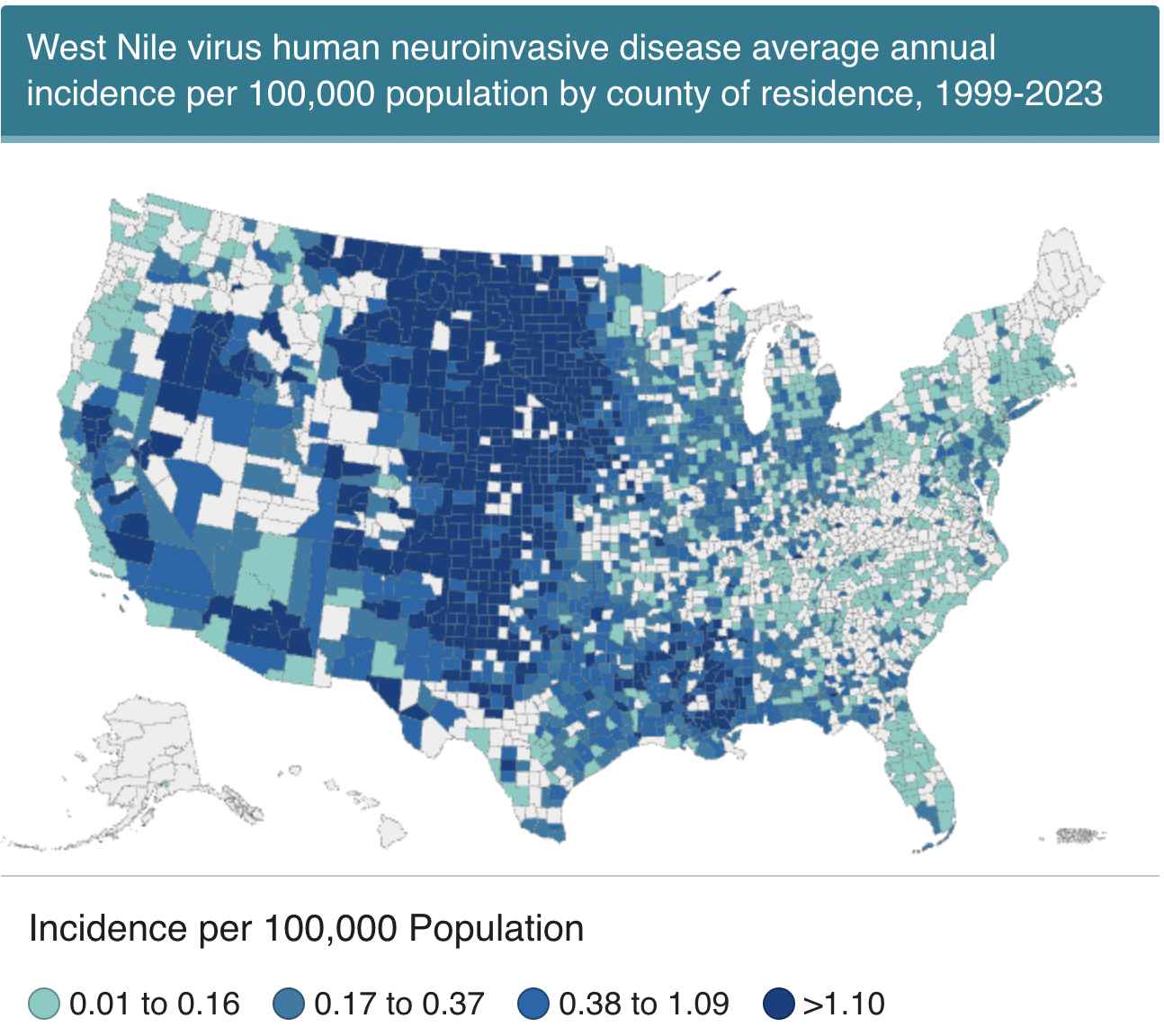
Case Presentation: West Nile Virus (WNV) was first reported in the Western Hemisphere in New York City in 1999. Over the last two decades West Nile Virus has spread to an impressive distribution from central Canada to Southern Argentina. Transmission of the virus is maintained in a cycle between Culex species mosquitos and birds as the hosts. Transmission to humans occurs when people are bitten by an infected mosquito. Human cases have the highest transmission in summer and early fall with 94% reported from July to September. We report a case of a 69-year-old Caucasian female with history of DM, Afib, and Hypothyroidism who was admitted to a hospital in August of 2023 with fevers, lethargy, and generalized weakness. She was initially seen in urgent care one week prior to her admission with complaints of fever and headache. She was told she had a viral URI and was sent home. She had no recent travels. She is retired and spends her spring and summers gardening. On the initial exam she was febrile (100.4 °), lethargic, had bilateral lower extremity weakness, and headache with photophobia, negative Kernig’s, and Brudzinski sign. Her CBC, TSH, urinalysis, upper respiratory panel, and CMP were unremarkable. She was started on Vancomycin and Cefepime due to ongoing fevers. Two days later Acyclovir was added to her regimen by an infectious disease specialist due to concerns of meningitis. She briefly showed improvement in her mentation on antibiotics and antivirals before having worsening encephalopathy. The workup thus far was unrevealing with negative blood culture and pending fungal cultures, MRI brain was unremarkable, Echocardiogram did not show any vegetations. Neurology was consulted for worsening encephalopathy and lumbar puncture. Her lumbar puncture was notable for CSF WBC 50, RBC 6, Glucose 96, Protein 76, meningitis/encephalitis PCR panel testing was negative. Antibiotics were stopped and Acyclovir was continued until HSV PCR was negative. She had a positive West Nile antibody 6 days after her admission and was diagnosed with West Nile Meningitis. She was treated with symptomatic/supportive care and was discharged to subacute rehab with close outpatient Neurology follow up.
Discussion: This is a distinctive case of West Nile Virus as approximately 80% of human WNV infections are asymptomatic and less than 1% of symptomatic cases develop manifestations of neuroinvasive disease. This may be the reason the patient was initially misdiagnosed and sent home. A second reason this case is rare is its location, which is not statistically known as an epicenter for WNV. In recent years there has been a relative rise in the area. The focus of this case shows the complex and elusive presentation of WNV that can delay diagnosis. The diagnostic criteria of WNM are not very specific – includes clinical signs of meningeal inflammation or additional evidence of acute infection from one or more of: temperature >100.4° or < 95° F; CSF pleocytosis (>5 leukocytes/mm3), peripheral leukocytosis >10k, or neuroimaging consistent with acute meningeal inflammation. In our patient most of these signs were only evident later in the course.
Conclusions: WNV is easily misdiagnosed and should be considered in a patient with fever, progressive neurological symptoms and rapid deterioration as this one. This case raises awareness for detecting neuro invasive WNV and avoiding pitfalls of diagnostic bias. This case serves as a learning opportunity for clinicians to be aware of local outbreaks and updated surveillance data on rising infectious diseases in humans.