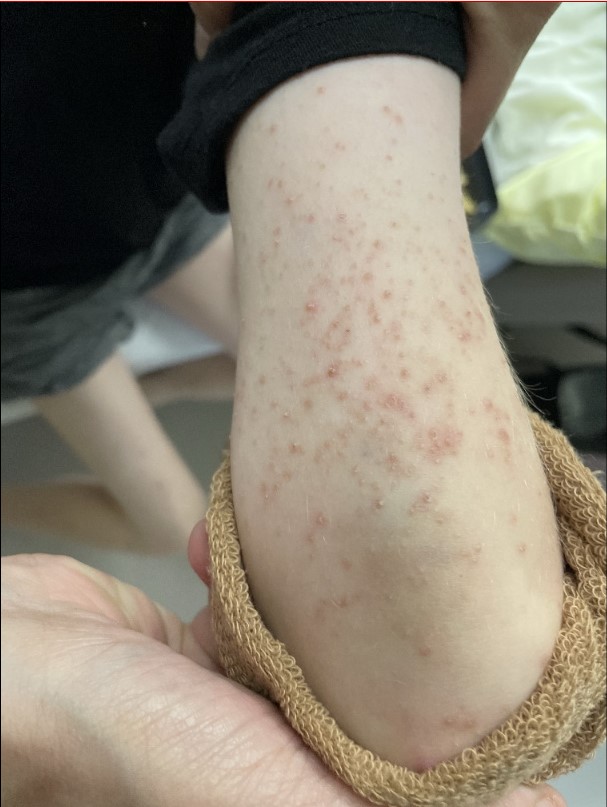
Case Presentation: A 10-year-old boy with autism presented for multiple complaints including recurrent anemia, rash, and eye redness with light sensitivity. All prior care was in a different healthcare system. 9 months prior, he was admitted for severe anemia (hemoglobin 3.5) with iron deficiency, and esophagogastroduodenoscopy (EGD) showed multiple gastric ulcers with bleeding. Hemoglobin improved with transfusions. Bleeding was attributed to ibuprofen use. An interval EGD showed resolution of ulcers. 2 months prior, he was admitted with recurrent anemia. Fecal occult blood was negative. Another EGD was performed which did not show bleeding. Irritation of the esophagus was biopsied, pathology showing hyperkeratosis and parakeratosis, which can be seen in vitamin deficiencies.Shortly after second admission, patient developed a papular rash on his arms and legs, which progressed to the face. Mother also noticed eye redness, rubbing, and sensitivity to light. On presentation, patient had normocytic anemia (hemoglobin 8.0). Iron studies showed adequate stores. No hemolysis. Weight loss of 1.5 kilograms over 9 months was noted. On further questioning, diet was extremely limited, mostly French fries, bread, and oranges with small amounts of a formula supplement. During admission, an extensive workup was initiated to find a unifying diagnosis. Hematology and gastroenterology were consulted with low suspicion for primary bone marrow process or active bleeding. A thorough laboratory evaluation of vitamins and micronutrients was sent and revealed low vitamin A and E, zinc, copper, and fatty acids. Riboflavin and vitamin C were at the lower limit of normal. Dermatology evaluated patient’s rash which was consistent with phrynoderma, associated with vitamin deficiencies.(1,2) Appropriate supplementation was started.
Discussion: This patient’s presenting complaints of recurrent anemia, rash, light sensitivity and weight loss, initially appeared to be separate, but ultimately were all determined to be related to nutrient deficiencies due to a severely restricted diet. There was some anchoring to the initial diagnosis of iron deficiency anemia due to bleeding, which had resolved. Vitamin A deficiency is associated with night blindness but also corneal xerosis, which explains the patient’s light sensitivity and frequent eye rubbing. Anemia develops due to impaired erythropoiesis and maturation of erythrocytes, compounded by the role of vitamin A in iron mobilization and absorption. Copper, zinc, vitamin C and E deficiencies all further contribute to anemia.(1-4) Phrynoderma is a form of follicular hyperkeratosis associated with nutritional deficiencies including vitamins A, B, C, E and essential fatty acids, all of which were low in this patient.(1) It is typically found on the extensor surfaces of the extremities, shoulders and buttocks. Treatment is focused on improvement in nutrition status. For this patient, his rash did improve over the next 2 months.
Conclusions: Severe malnutrition and vitamin deficiencies can present in various ways, especially in children with medical complexity. Children with autism are at risk of malnutrition due to sensory sensitivities and restrictive food preferences.(5) Parents may not volunteer information on diet unless directly asked, as was the case here. Ultimately, the patient’s course illustrates the range of possible long-term effects of micronutrient deficiencies and the importance of searching for a unifying diagnosis for myriad, seemingly disparate symptoms.