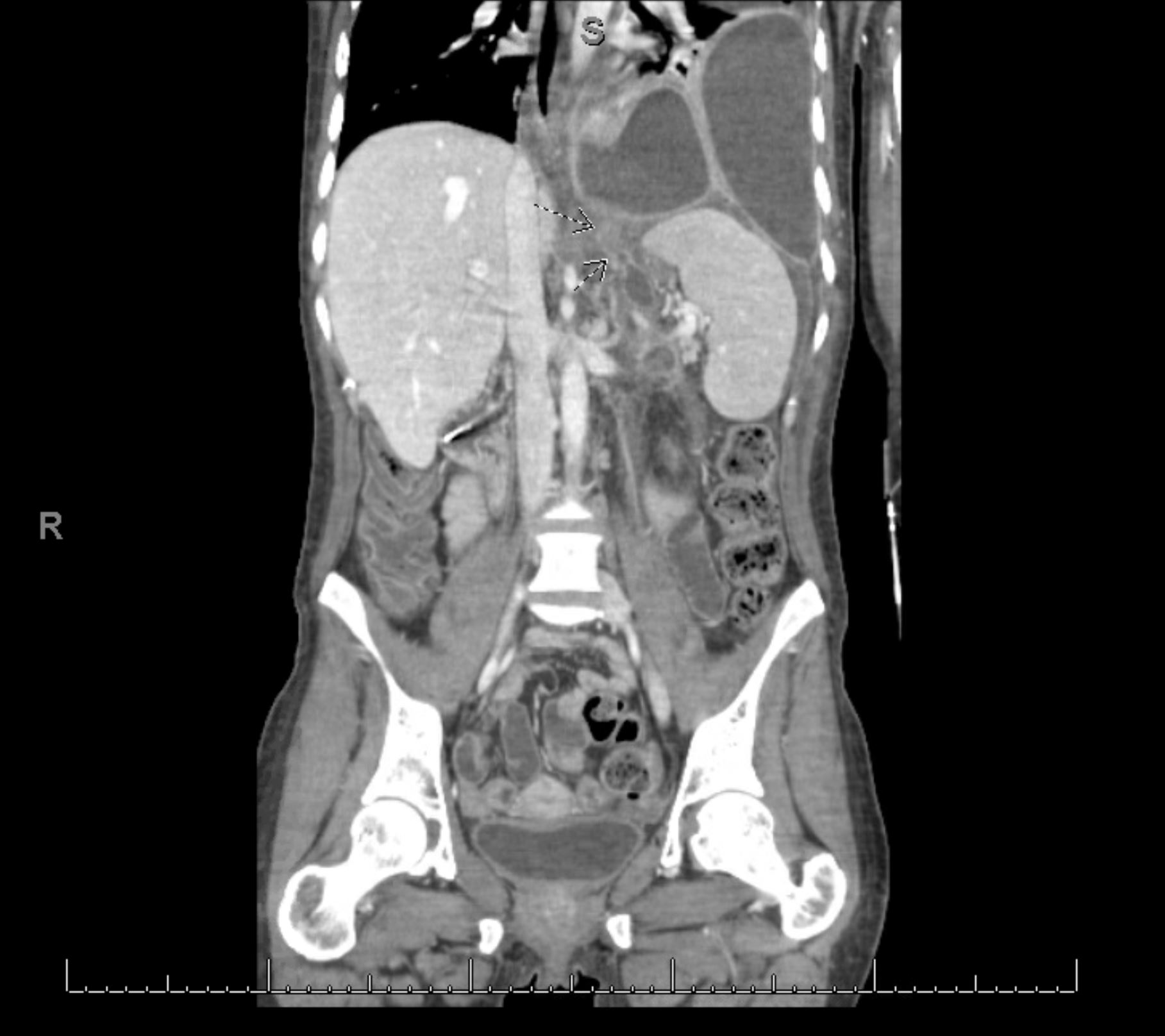
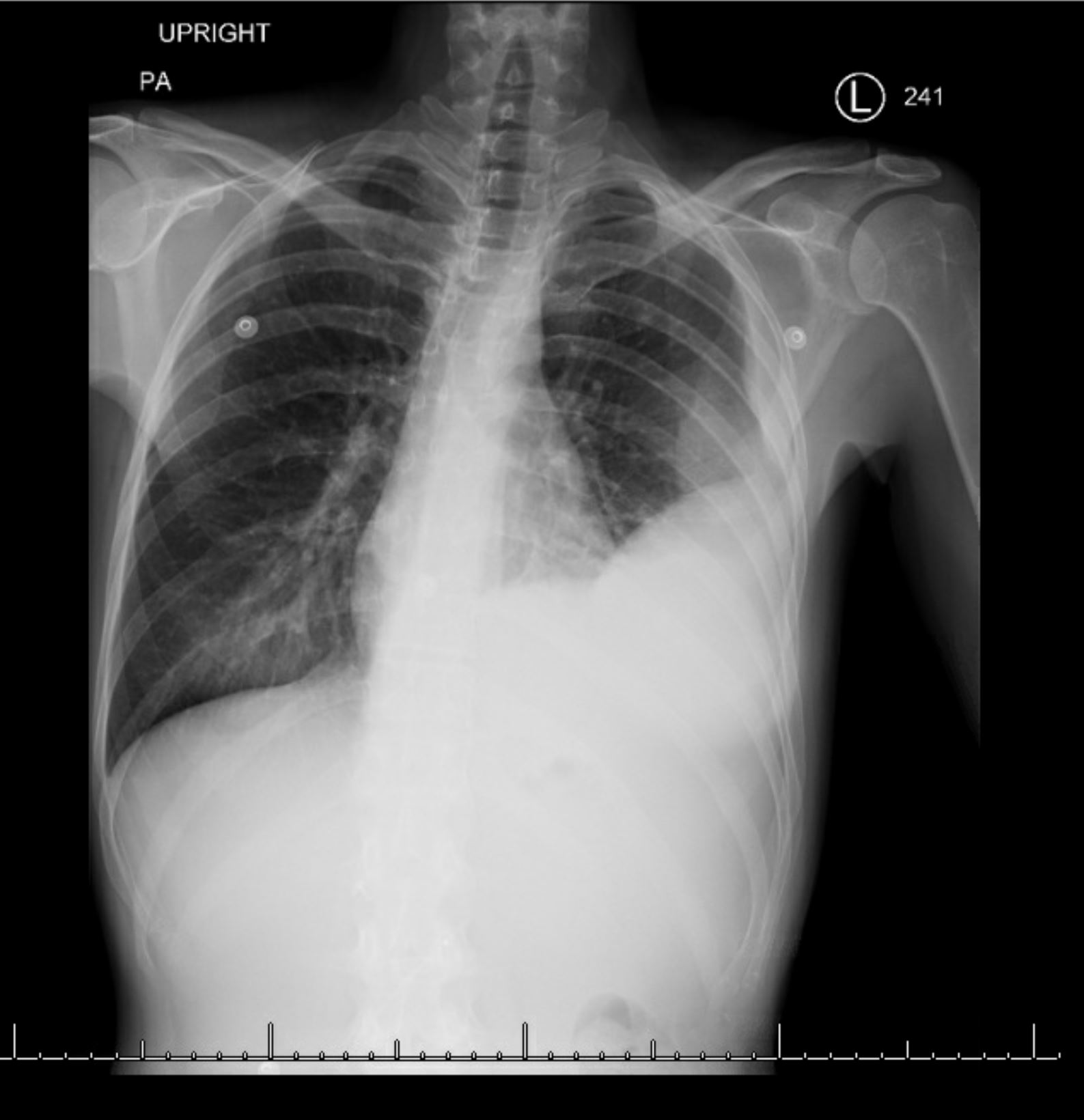
Case Presentation: A thirty-three year old woman with a history of alcohol-induced chronic pancreatitis and sphincter of Oddi dysfunction presented with dyspnea and a non-productive cough. She was admitted to the intensive care unit for acute hypoxic respiratory failure. On arrival, she was febrile and hypoxic, saturating 80% on room air. Labs were notable for a leukocytosis and chest radiograph revealed a new pleural effusion. She underwent multiple thoracenteses, revealing an exudative fluid with elevated lipase and amylase. Ultimately, a pigtail catheter was placed. Magnetic resonance cholangiopancreatography (MRCP) and computed tomography (CT) of the pancreas revealed retropancreatic fluid extending to the left subdiaphragmatic space without definitive findings of a fistulous tract. However, endoscopic retrograde cholangio-pancreatography (ERCP) revealed a leak in the ventral pancreatic duct directed toward the left hemidiaphragm, leading to stent placement. The patient’s oxygenation status improved after initiation of antibiotics and she was discharged with stable pleural effusions. The patient returned two weeks later with a left sided empyema and CT evidence of a pleuro-pancreatic fistulae (PPF). ERCP showed a persistent pancreatic duct leak requiring a larger stent. Ultimately, she underwent a video-assisted thoracoscopic surgery (VATS) and decortication procedure. The patient improved clinically with reduction of empyema on imaging and was discharged. Follow-up ERCP ten weeks later showed a significant reduction in the pancreatic leak. A larger caliber stent was placed to facilitate healing. Her subsequent ERCP revealed that the leak had completely resolved, and the stent was removed. Follow up secretin-enhanced MRCP three months later revealed no evidence of a leak.
Discussion: PPF are rare complications of chronic pancreatitis occurring due to disruption of the main pancreatic duct and tracking of pancreatic fluid into the thoracic cavity. Patients commonly present with refractory unilateral pleural effusions. Initial management consists of thoracentesis with fluid analysis which usually reveals an elevated lipase and amylase. We present a case of a patient who presented with respiratory distress and fluid analysis consistent with a pancreatic leak. ERCP has emerged as both a diagnostic and therapeutic modality, while MRCP is the radiological investigation of choice. The optimal treatment strategy for PPF is currently unknown. It has traditionally been treated with medical management followed by operative therapy for those who fail conservative treatment. Our patient was successfully treated conservatively with multiple stent placements with no further evidence of leakage in subsequent imaging.
Conclusions: Although PPF is considered a rare complication of chronic pancreatitis, occurring in 0.4% of patients with chronic pancreatitis, it is essential to consider it in the differential of a patient with respiratory compromise and history of chronic pancreatitis.