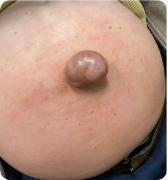
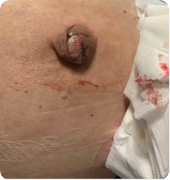
Case Presentation: A 46-year-old male with alcohol use disorder and cirrhosis presented to the emergency department for 1 day of persistent ascitic fluid leakage from his umbilicus. Exam was significant for ascites and a reducible, ulcerated umbilical hernia. The ulcer was cleaned, sealed with skin glue, and the patient was discharged. He presented again 7 days later with the same complaint, and exam showed persistent ulcerated hernia with new surrounding erythema. General surgery temporized the leak with bedside sutures, and the patient was admitted to medicine. Initial vital signs were normal. Labs were significant for creatinine 1.17 (baseline 0.7 mg/dl) and leukocytosis 14×10*9/L, with MELD 3.0 score 11. Paracentesis studies were not consistent with spontaneous bacterial peritonitis (SBP). Due to concern for cellulitis and high risk of SBP from ruptured hernia, he received 7 days of IV antibiotics followed by oral SBP prophylaxis. Albumin-assisted diuresis failed due to renal injury, and surgical risk was deemed too high for urgent hernia repair given ongoing ascites. He underwent a transjugular intrahepatic portosystemic shunt (TIPS) procedure and repeat LVP. Two weeks later, he remains admitted for ongoing complications including upper GI bleed and acute kidney injury. Once volume status is optimized, expedited hernia repair is expected.
Discussion: Coined by Frank B. Flood in 1961, Flood syndrome describes an umbilical hernia rupture in decompensated cirrhosis with spontaneous paracentesis. Flood Syndrome is a rare and underrecognized clinical diagnosis with high morbidity and mortality that should prompt inpatient admission for stabilization and further workup. Complications include bowel incarceration or evisceration, cellulitis, peritonitis, sepsis, and hemodynamic instability. Patients with cirrhosis are at higher risk for umbilical hernias (20% compared to 2% of the general population) due to recurrent ascites, weakened abdominal wall musculature, malnutrition, and umbilical vein recanalization from portal hypertension. Early referral to surgery is crucial, particularly if signs of impending rupture like ulceration or necrosis over the hernia are present.Optimal management strategies for Flood syndrome are elusive due to limited data and high surgical risk inherent to patients with end-stage liver disease (ESLD). Treatment options include supportive management (superficial suture repair, fibrin glue injection, ostomy bag placement, treatment of ascites with TIPS or an intrabdominal drain) or definitive management (surgical hernia repair). All patients should receive antibiotics for SBP prophylaxis. Deciding which course to pursue is difficult, as mortality rates with supportive management are 60-80%, while postoperative mortality rates are 6-20% but with significantly higher morbidity (up to 71%).In our case, TIPS was used to decrease ascites over time to optimize for future hernia repair. One review suggests that Flood Syndrome treatment with TIPS is rare with only 9 cases identified to date, but this is an area for further research.5
Conclusions: Inpatient providers should recognize Flood Syndrome, a rare and underrecognized complication of ESLD, as prompt inpatient admission for stabilization and further workup is warranted. Referral to tertiary care centers for volume status optimization and expedited surgical and gastroenterology evaluation should be pursued given high morbidity and mortality.