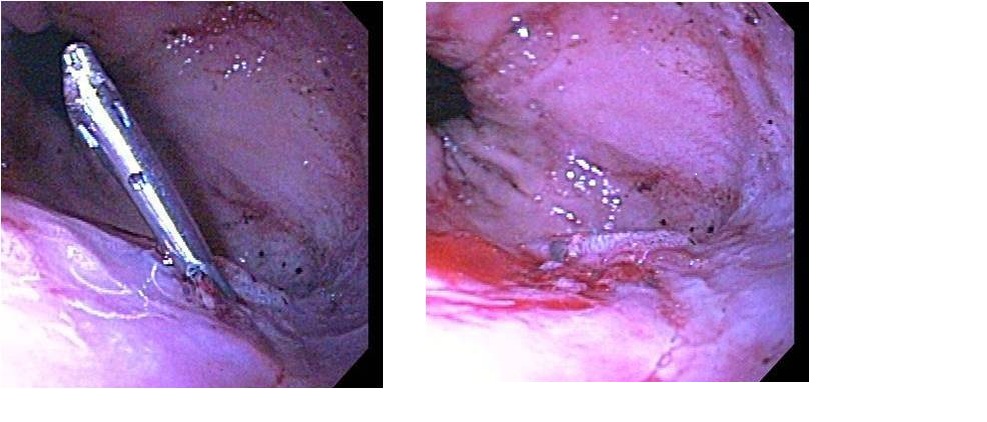
Case Presentation:
A 61 year old male with a history of hiatal hernia, paroxysmal atrial fibrillation on aspirin, hypertension, and diverticulosis presented with non-bloody emesis and blood-tinged diarrhea. He reported many sick contacts with similar symptoms. The patient was admitted to the hospital for dehydration secondary to presumed gastroenteritis. Upon admission, patient complained of increased lightheadedness and was significantly orthostatic.
The following morning, the patient had a large bright red bloody bowel movement. His hemoglobin dropped from 12.6 g/dL to 6.9 g/dL. The gastroenterology service was consulted and an esophagogastroduodenoscopy (EGD) was performed. This revealed a large hiatal hernia in the distal esophagus, with an actively oozing lesion within the hiatal hernia (Cameron lesion). The lesion was injected with epinephrine and one hemoclip was used. There were no active bleeds on endoscopy after the intervention. Patient was transfused four units of blood while in the hospital and did not have any further clinical signs of bleeding. He was discharged on an oral proton pump inhibitor (PPI) once daily. The patient has been followed up in the outpatient setting and has had no further incidence of upper gastrointestinal bleed.
Discussion:
Cameron lesions are linear gastric erosions or ulcers that are present along the mucosal folds located distally within a hiatal hernia. They are often an incidental finding, and are present in approximately 5% of patients with hiatal hernias.
Cameron lesions more commonly present with chronic gastrointestinal bleeds with iron deficiency anemia. These lesions rarely present with acute gastrointestinal bleeds as was the case with our patient. The gold standard for diagnosis is EGD. However, this lesion is also commonly missed on endoscopy.
Historically, treatment involves twice daily PPI and iron replacement therapy. To our knowledge there are no studies that compare different treatment options for Cameron lesions (likely due to the rarity of the disease). Our patient was treated by endoscopic intervention along with once daily PPI with good results. This suggests that the typical double dose PPI may not be necessary for every patient with this lesion, although more data is needed.
Conclusions:
Cameron lesions are a rare cause of acute upper gastrointestinal bleed. Diagnosis is made by EGD, although this may miss lesions as well. More data is needed to determine the optimal treatment regimen for this lesion.