Background:
There is increasing emphasis on timely outpatient follow‐up visits after hospital discharge. However, there is little consensus regarding what should take place in the follow‐up visit. In this study, we described the content documented in postdischarge follow‐up visits.
Methods:
We reviewed the medical records of all adult patients discharged to home from the general internal medicine service in June 2012 at a 600‐bed academic medical center. Subjects were included if they had at least 1 outpatient visit with a medical center–affiliated primary care physician (PCP) or specialist within 60 days of discharge. We evaluated the subsequent outpatient note to determine visit content. We measured 5 parameters based on checklists proposed by the California HealthCare Foundation and by other facilities: (1) medication reconciliation or discussion, (2) whether the reason for hospitalization was discussed, (3) follow‐up on pending or recommended tests (if recommended by the discharge summary), (4) assessment of functional status, and (5) discussion of advance directives. To compare the mean parameters documented, t tests were used.
Results:
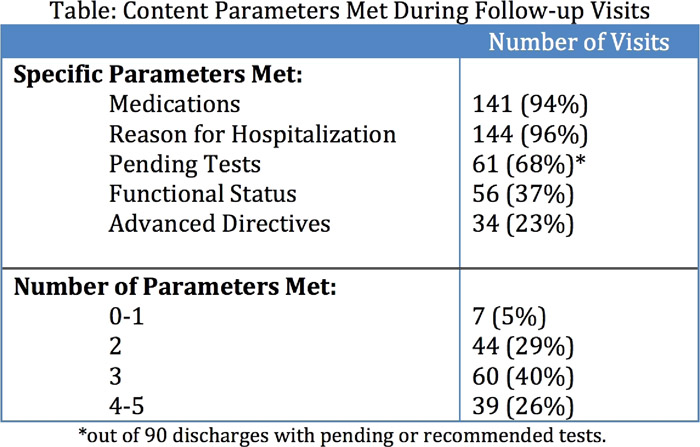
Of the 271 discharges to home during the 1‐month period, we analyzed 150 follow‐up visits (55%) of 142 patients (6 individuals had multiple hospitalizations with follow‐up in this period); 9% of patients had recurrent hospitalizations, ED visits, or died before a follow‐up visit, and 36% had no subsequent visit at the medical center. Of the 142 subjects, the mean age was 61.5±18.7 years, 78 were female (55%), and 64 were white (45%). More than half, 85 (60%), had a PCP in the medical center, and the remaining patients had a specialist. In 97% of cases, discharge summaries were available and completed prior to the outpatient visit. In 150 follow‐up visits, 108 visits (72%) occurred within 2 weeks of discharge, and 72 (48%) were performed by specialists. The content of the visit varied (Table). The mean number of content parameters met did not differ when comparing visits with PCPs and specialists (2.9 vs. 2.8, respectively; P = 0.40), nor did it differ when follow‐up occurred within 2 weeks compared to more than 2 weeks from discharge (3.0 vs. 2.7, respectively; P = 0.21). There were no significant differences by patient age, sex, or race/ethnicity.
Conclusions:
In the postdischarge follow‐up visit, medications and the reason for hospitalization were almost universally addressed; beyond that, visit content varied. Standardization of the postdischarge visit may help the transition between hospital and home.