Background: The proportion of young adults with complex medical needs and chronic illnesses cared for at pediatric hospitals is substantially increasing. ACGME requires both pediatric and Internal Medicine (IM) residents to manage patients with complex or chronic conditions and coordinate care across the healthcare continuum, including transitioning to adult care. However, barriers to transitioning these patients to adult hospitals for acute care include knowledge gaps and provider discomfort. To inform future educational interventions to address these gaps, this study examined and compared pediatric and IM resident confidence caring for young adult patients with complex medical needs at different stages of training.
Methods: Based on relevant literature and experiential learning theory, we developed a novel survey to explore resident confidence in managing young adults with complex or chronic illnesses admitted to the hospital. Pediatric residents from a free-standing children’s hospital and IM residents from the associated university-affiliated institution were anonymously surveyed through an email invitation. Independent samples were simultaneously surveyed in the first year (PGY1) and senior years (PGY2-3) of residency. Using a Likert scale (1-strongly disagree to 5-strongly agree), the survey assessed confidence in skills needed to care for these hospitalized patients in the following domains: 1) assessing and ordering home GT feedings, 2) assessing and ordering home airway clearance, 3) assessing patient cognitive abilities and capacity, 4) assessing goals of care 5) preparing for discharge and transitioning to outpatient care. Data was collected through Qualtrics software. Data analysis consisted of descriptive statistics and Wilcoxon Rank Sum tests compared the median confidence level in first year vs. senior year pediatric and IM residents.
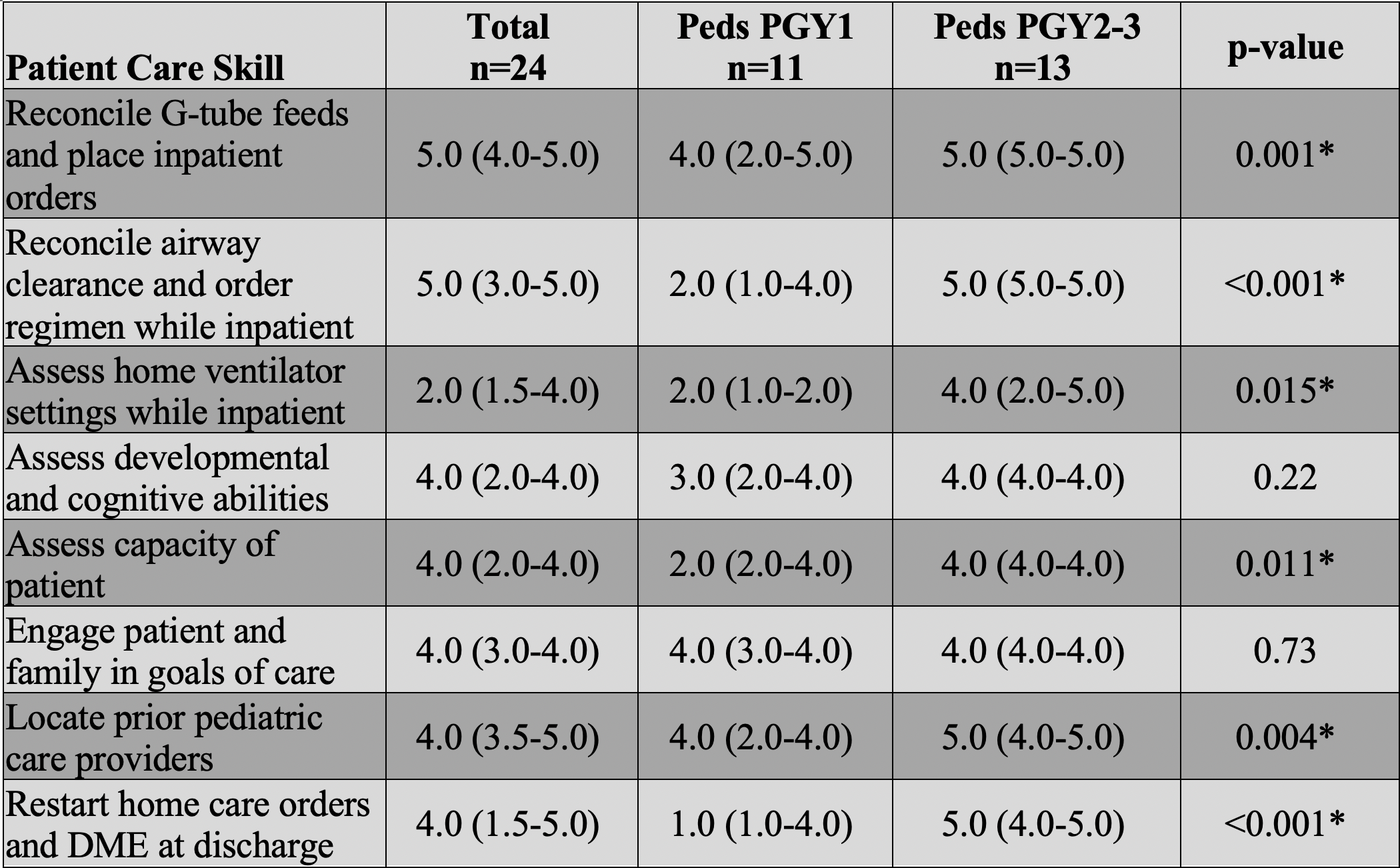
Results: Twenty-four pediatric and twenty-four IM residents completed the survey in November 2020. Survey results revealed confidence levels of intern and senior pediatric residents (Table 1) and IM residents (Table 2) for the various patient care skill domains. Pediatric senior residents had significantly greater confidence than pediatric interns in managing g-tube feed orders, reconciling airway clearance orders, assessing home ventilator settings, assessing capacity, locating prior healthcare providers, and restarting home healthcare and durable medical equipment orders at discharge (Table 1). Conversely, IM resident confidence did not vary between intern and senior years for any of the skills assessed, and IM residents had low confidence in these skills, except engaging in goals of care discussions (Table 2).
Conclusions: Pediatric residents at different levels of training report greater confidence in many aspects of young adult complex care compared to IM residents. It is important that IM physicians feel as prepared to care for these patients when hospitalized. This needs assessment highlights differences between training programs and perhaps a gap in IM residency education. Results represent an opportunity for future curricular collaboration across pediatric and IM residencies to bridge this gap in hospital medicine.