Background: While medical school experience could be very rewarding, it is also known to be unusually stressful to many future physicians. Previous cross sectional studies have shown that symptoms of depression and burnout are higher among medical students compared to age matched general population. A meta-analysis reported overall pooled crude prevalence of depression, or depressive symptoms, at 27.2% (9.3% to 55.9%), and overall cross sectional prevalence of burnout at 56%. Most previous studies were cross sectional and data on longitudinal change of these important variables are limited. Depression and burnout have long term consequences in personal and professional lives. Real world empirical data and trend will be helpful to build a stronger consensus for the need for remedial action starting with the medical school education.
Methods: We are presenting a descriptive analysis from 7 cohorts of medical students who matriculated from 2010 to 2016. This is part of “Health and Wellness among Medical Students” longitudinal study that started in 2009 in a mid-Atlantic private medical school. Every year participants completed an informed consent at the first encounter, based on an approval granted by relevant Institutional Review Board. Depression was measured by the Patient Health Questionnaire depression module (PHQ-9), and burnout with Maslach Burnout Inventory-Human Services Survey (MBI-HSS). Our primary predictor was medical school year (1st Year, 2nd Year, 3rd Year, 4thYear). We fit logistic regression models for both outcomes and adjusted for age, race, gender, marital status and cohort.
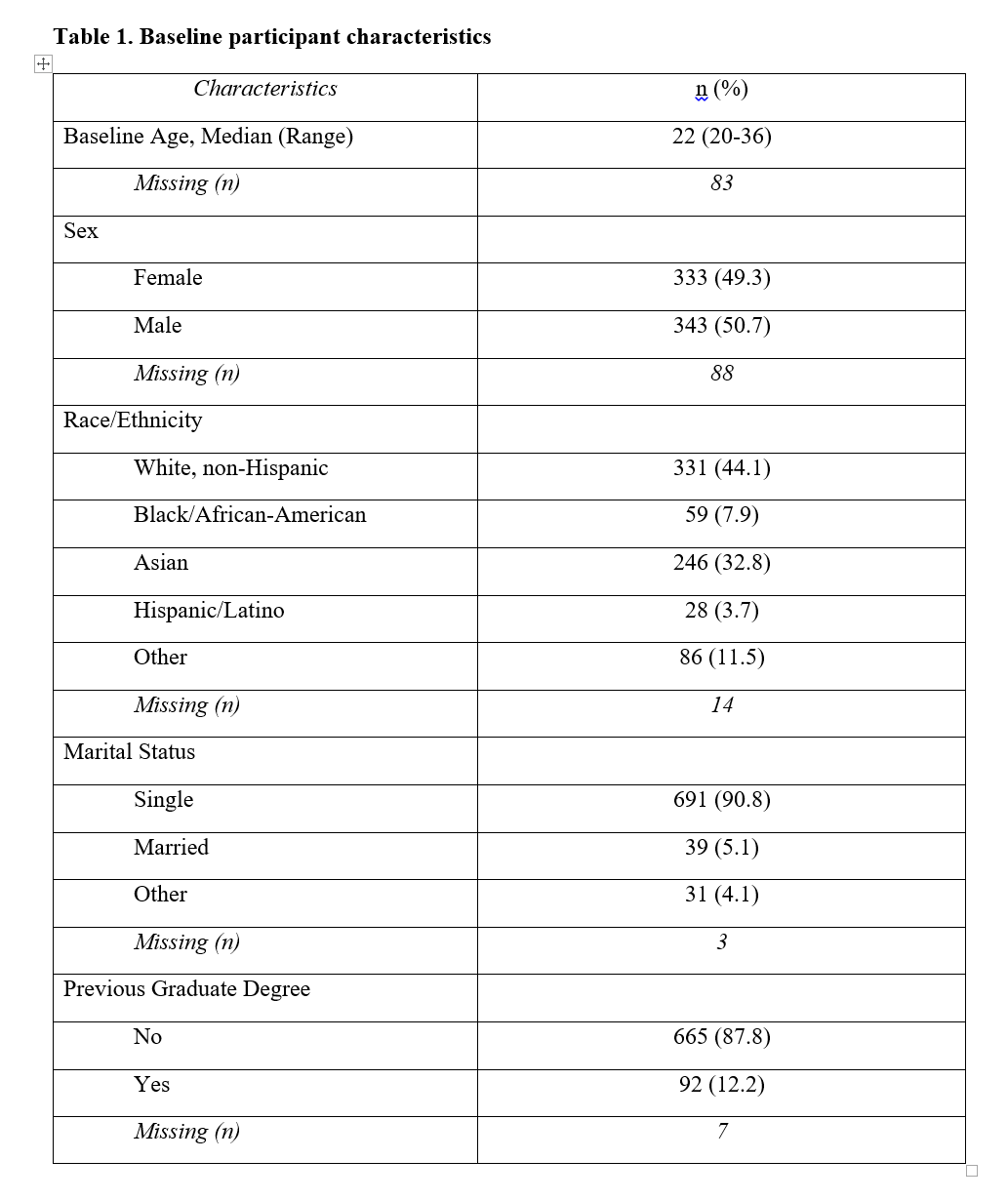
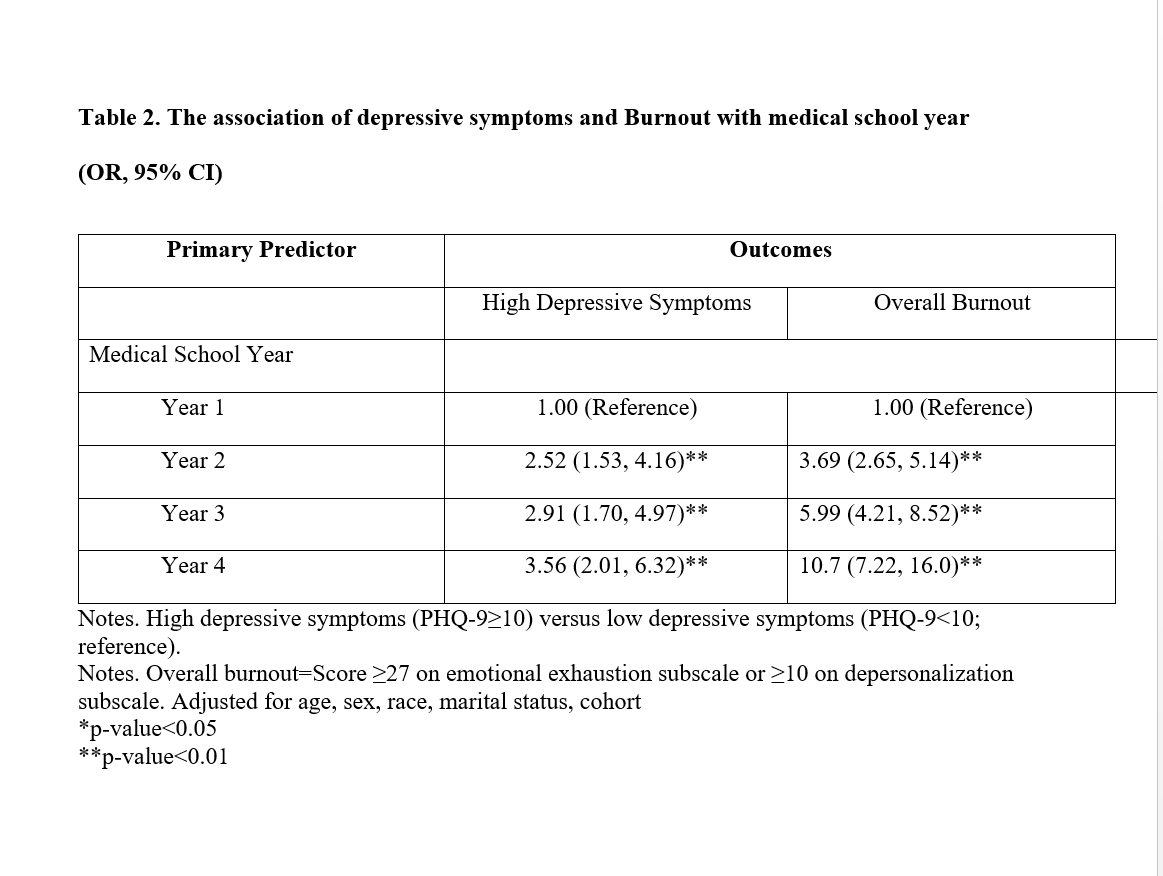
Results: Of the 764 participants across all 7 cohorts who completed the survey at baseline, 509 (66.6%) participants completed during their 2nd year, 369 (48.2%) during their 3rd year, and 250 (32.7%) 4th year follow-up survey. Of the participants, 44.1% were White, non-Hispanic, and 90.8% were single. Across all 4 years, the prevalence of high depressive symptoms was significantly different (χ2=31.4 p<0.01). Among 1st year medical students, the prevalence was 4.3%. Among year 2nd, 3rd, and 4th year medical students this prevalence was 10.5%, 10.9%, and 13.9%, respectively. Among 1st year students, the prevalence of overall burnout was 13.5%, which increased to 60.9% among 4th year students. Across all 4 years, the prevalence of overall burnout was significantly different (χ2=216.0, p<0.01). After adjustment for age, race, gender, marital status, and cohort, year of medical school compared to 1st year medical students, 2nd year students had a greater odds of high depressive symptoms (OR=2.52, 95% CI 1.53, 4.16), as did 3rd year (OR=2.91, 95% CI 1.70, 4.97), and 4th year students (OR=3.56, 95% CI 2.01, 6.32). Compared to 1st year medical students, 2nd year students had a greater odds of overall burnout (3.69, 95% CI 2.65, 5.14), as did 3rd year students (OR=5.99, 95% CI 4.21, 8.52), and 4th year medical students (OR=10.7, 95% CI 7.22, 16.0).
Conclusions: Prevalence of symptoms of depression and burnout increases significantly in each of medical school year. We as academic hospitalists who are medical students’ educators should be mindful about vulnerabilities, risk factors, and trends of depression and burnout during medical school. This knowledge can be vital in making curriculum changes and other interventions, to maximize the opportunity for a medical school entrant to be successful in their entire medical career.