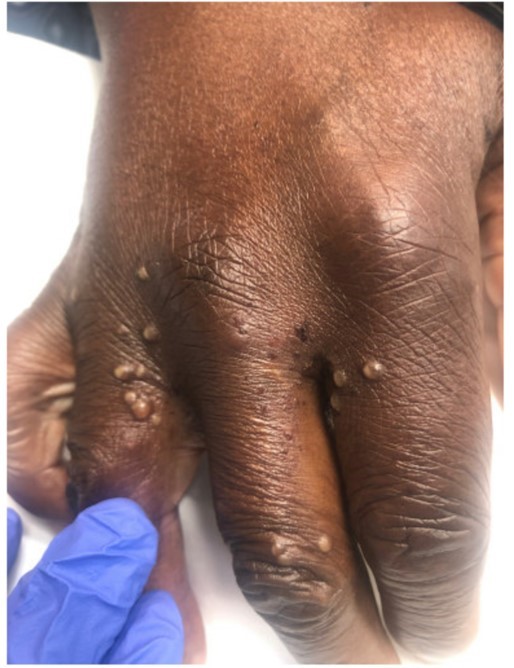
Case Presentation: A 63-year-old man with type 2 diabetes, a previous gunshot wound with left upper extremity contracture, and a prior stroke presented to the emergency room in July 2022 with a rash on his right hand, swelling of the distal right arm, and a few scattered spots on his abdomen and flanks. The patient is wheelchair-bound and relies on home healthcare services for much of his routine daily care. Patient had not been sexually active; he had not been taking any new medications, he had no pets at home, recalled no sick contacts and felt generally well. Over the next day, multiple additional lesions appeared on his right forearm. He was afebrile with normal vital signs; skin exam was notable for scattered pinpoint pustular monomorphic lesions predominantly on the dorsal aspect of the right hand and in the web spaces of his right hand, but also noted over the abdomen and bilateral flanks [image1]. A complete blood count and chemistries were normal. A lesion swab was negative for herpes simplex/zoster. Pustule cultures grew normal skin flora. HIV and syphilis testing were negative. Skin scraping was negative for scabies. After several days in the hospital, an outing to the patient’s home to investigate possible arthropod infestation, and one lost monkeypox result, the patient’s pathology data returned: Orthopoxvirus PCR was negative; punch biopsy revealed epidermal ulceration with abundant eosinophils and no viral cytopathic changes present. These findings were most consistent with arthropod assault. The patient was treated with topical steroids and had evidence of healing lesions at time of discharge. Red imported fire ants (Solenopsis invicta) were acquired from the patient’s front porch, further supporting the diagnosis [image2].
Discussion: This case illustrates the vital importance of taking a good history and considering a broad differential diagnosis, especially during the evolving monkeypox outbreak. The red imported fire ant, a small, reddish-brown insect, is an invasive species of ant native to South America. The arthropod is quite widespread due to its fortuitous genetic characteristics and can be found in all parts of the United States; thus, assault by such creatures is far more likely than infection by the emerging monkeypox virus. Injuries from ants are often called ‘bites’, a description only partly true: the ant merely uses its mandibles to hold on to a victim, then plunges its venomous stinger into the epidermis, and the venom causes a local inflammatory response. The resulting pustules can resemble those following monkeypox infection. Unlike monkeypox, ant stings do not cause an accompanying systemic response. Of the 12,000 ant species, the fire ant was felt to be the most likely offender in our case because of its color, size, pervasiveness, and aggressive nature. What was key in this case was the proper identification of the species of ant, secured by traveling to the patient’s home to collect specimens, in true scientific fashion.
Conclusions: We draw two important conclusions about hospitalist work from this case: 1) Hospitalists can learn valuable diagnostic data by exploring specifically the environments in which our patients live. 2) Hospital medicine is collaborative: the correct diagnosis was obtained by working closely with infectious disease physicians, pathologists, dermatologists, and an amateur myrmecologist. In our case, hospitalists did not discount arthropod assault in the differential diagnosis, even in the face of emerging zoonotic illnesses.