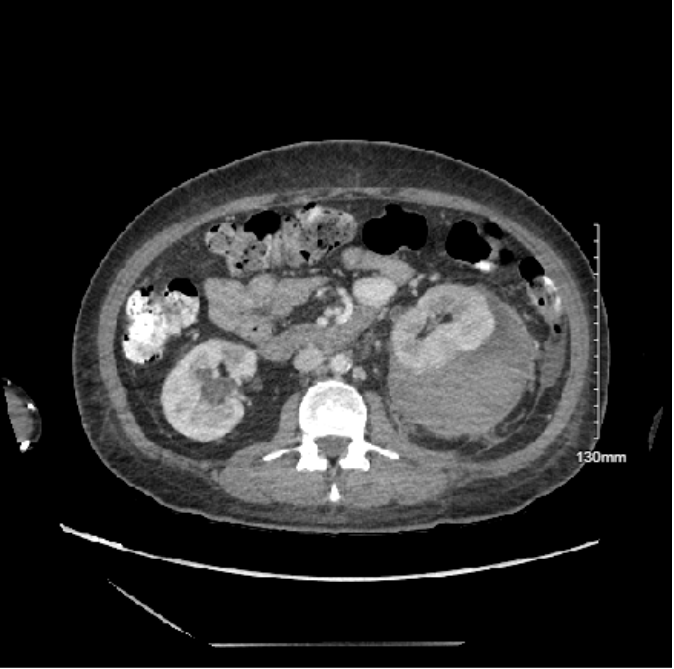
Case Presentation: A 43-year-old woman with uncontrolled type II diabetes mellitus, hypertension, CKD stage 3, and prior history of pyelonephritis complicated by E. coli bacteremia, presented with vomiting, anorexia, fever, chills, and mild abdominal discomfort. Exam was notable for normal vital signs, mild diffuse abdominal tenderness, and no costovertebral angle tenderness. Laboratory studies showed a hemoglobin of 11.1 mg/dL, WBC 15.43 × 10³/µL, and creatinine 2.9 mg/dL. Urinalysis revealed bacteriuria and 616 WBCs. Renal ultrasound demonstrated mild chronic changes, normal kidney size, no hydronephrosis, and no signs of bleeding. The patient was diagnosed with pyelonephritis and started on ceftriaxone. On hospital day four, after receiving fluids and antibiotics, the patient felt well, but hemoglobin dropped to 5.6 mg/dL, and creatinine increased to 4.56 mg/dL. Since the patient felt well, she declined further treatment and left the hospital against medical advice.She was readmitted later the same day with worsening diffuse abdominal pain and projectile non-bloody, non-bilious emesis. Vital signs were remarkable for tachycardia to 111 and blood pressure of 184/111 mmHg. Repeat laboratory studies showed a creatinine of 4.37 mg/dL. CT of the abdomen revealed a large subcapsular hematoma adjacent to the left kidney measuring up to 14 x 8.8 x 6.6 cm with hemorrhagic stranding in the left perinephric space causing compression of the renal parenchyma. The patient was diagnosed with Wunderlich syndrome complicated by Page kidney. She successfully underwent robotic-assisted left perinephric hematoma evacuation. These interventions eventually resulted in resolution of hypertension and improved renal function, with her creatinine downtrending to 2.42-3.16 mg/dL prior to discharge.
Discussion: Wunderlich syndrome (WS) is an uncommon condition marked by spontaneous, nontraumatic hemorrhage into the perirenal, subcapsular and/or pararenal spaces (1). The classic “Lenk’s triad” of flank pain, a palpable flank mass, and hypovolemic shock is associated with WS, but is only present in a small subset of patients. The majority of patients present with nonspecific symptoms, such as fever, nausea, and vomiting. Most cases are due to neoplasm or vasculitis, but, rarely, it can be caused by infection (2). CT scan of the abdomen is the preferred imaging modality for diagnosis (3). Some cases of WS are complicated by a phenomenon called Page kidney, where hypertension develops due to renal parenchymal compression and subsequent activation of the renin-angiotensin-aldosterone system (RAAS) (4,5). While there is no consensus on the management of Page kidney, conservative treatment with oral medications that block the RAAS system may be effective. Percutaneous drainage of the hematoma is required if hypertension persists, although fluid may accumulate. Surgical options include hematoma evacuation, capsulectomy and radical nephrectomy (6).
Conclusions: This case highlights the importance of considering renal hematomas in patients with unexplained abdominal pain, hypertension, and renal dysfunction, particularly in the setting of high-risk conditions like pyelonephritis. While hemorrhage is usually associated with hypotension, Page kidney leads to the opposite since compression of the renal parenchyma and activation of the RAAS system result in hypertension. Prompt imaging and a multidisciplinary approach are crucial for optimal outcomes.