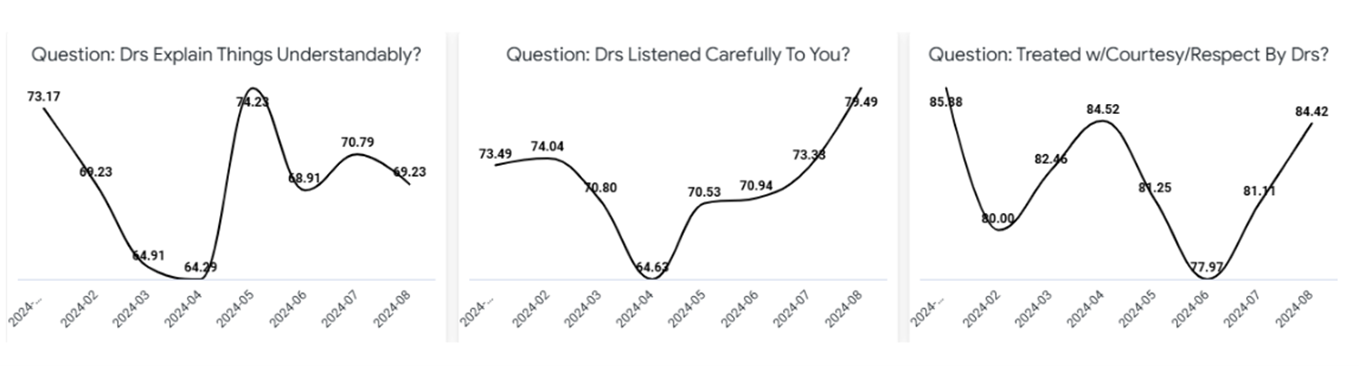
Background: Patient experience is critical in the quality of care delivered in hospitals and is closely linked to better clinical outcomes and patient satisfaction. Hospitalized patients under the care of hospitalists often face challenges related to communication, understanding their plan of care, and feeling connected to their healthcare team. Enhancing patient experience in this setting can improve satisfaction and engagement, while also addressing concerns around care continuity and communication.
Purpose: This project aims to improve the patient experience for hospitalized patients managed by the hospitalist team through targeted interventions that enhance communication, transparency, and patient engagement. Three primary tools were implemented: (1) dedicated afternoon office hours for patients and families to directly contact hospitalists, (2) a welcome letter with 24-hour contact information for hospitalists presented to patients boarding in the Emergency Department (ED), and (3) a shadowing program designed to identify and address patient-specific concerns, focusing on the plan of care, discharge process, and physician communication.
Description: 1. Afternoon Office Hours: A designated time each afternoon was established for patients and families to contact their hospitalist. This initiative aimed to enhance accessibility and improve communication, allowing patients to ask questions and discuss concerns in a structured setting.2. Welcome Letter for ED Boarders: Patients boarding in the ED while waiting for inpatient beds received a welcome letter from the hospitalist team. The letter included an overview of the hospitalist’s role and a 24/7 contact number to reach the hospitalist on call. This intervention aimed to reduce anxiety, foster a sense of support, and provide transparency about care during the boarding period.3. Shadowing Program: A patient-centered shadowing program was implemented, where members of the care team shadowed patients throughout their hospital stay to understand their concerns in real time. The program focused on key areas such as the clarity of the plan of care, discharge planning, and physician friendliness. Feedback was collected and relayed to individual hospitalists to address concerns and implement changes in communication strategies.
Conclusions: The implementation of afternoon office hours, a welcome letter for ED boarders, and a patient shadowing program have the potential to significantly improve the patient experience for hospitalized individuals under the care of the hospitalist team. Initial feedback suggests these interventions increased patient satisfaction with communication and care planning, reduced anxiety around the hospital stay, and enhanced the perception of physician approachability. Ongoing monitoring aims to quantify the impact on patient experience scores, hospital readmission rates, and clinical outcomes, with the goal of refining and expanding these tools to other hospital settings.